The connection between gut bacteria and sleep has moved past the general-wellness stage. Named organisms with measured metabolic outputs now have published trial data tying them to sleep quality in controlled human studies.
The gut microbiome produces neurotransmitters and metabolites that cross into the brain and regulate sleep architecture — the structural pattern of sleep stages across the night. This article covers which bacterial genera appear in insomnia research, the three metabolic pathways they use to influence sleep (GABA production, butyrate and circadian clock regulation, and the tryptophan-to-serotonin-to-melatonin chain), controlled trial evidence for probiotic strains, and the bidirectional loop where poor sleep damages the microbiome in return.
This is distinct from how gut barrier breakdown reaches the brain, which covers intestinal permeability and LPS translocation. This article focuses on which organisms matter and what they produce.
Which Gut Bacteria Are Linked to Insomnia?
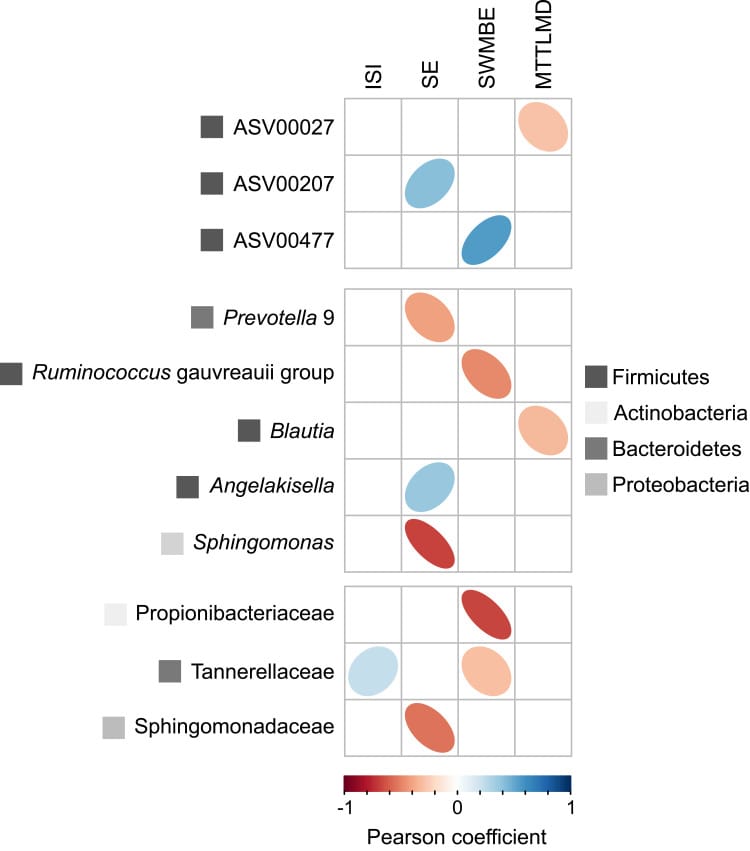
Both Lachnoclostridium and Blautia are short-chain fatty acid producers, which connects them to the butyrate-sleep mechanism covered in the next section. Haimov et al. (2022) used two weeks of actigraphy alongside fecal microbiota sequencing in community-dwelling older adults, and found that sleep quality and cognitive performance together explained 7.5-7.9% of variance in gut microbiota composition. In a complex biological ecosystem, that is a measurable association, and it held using objective sleep measurement rather than questionnaires alone.
On the other side of the ledger, people with insomnia consistently show elevated Proteobacteria — a phylum that serves as a marker of gut dysbiosis (microbial imbalance). The butyrate-producing species consistently depleted in insomnia include Faecalibacterium prausnitzii, Roseburia intestinalis, and Eubacterium hallii — the primary butyrate producers in the human colon.
A 2025 randomized controlled trial provides a direct test of whether changing this microbial pattern affects sleep. When Liu et al. (2025) supplemented Bifidobacterium animalis BLa80 in adults with sleep complaints, the strain reduced Proteobacteria while increasing Bacteroidetes, Fusicatenibacter, and Parabacteroides — moving the microbiome composition away from the dysbiotic pattern associated with insomnia.
How Do Gut Bacteria Affect Sleep?
Pathway 1: GABA (Gamma-Aminobutyric Acid) Production
Certain bacterial strains synthesize GABA (gamma-aminobutyric acid) — the primary inhibitory neurotransmitter responsible for sleep onset and maintenance. A 2025 randomized controlled trial confirmed that Bifidobacterium animalis BLa80 has measurable GABA production capacity via HPLC analysis (high-performance liquid chromatography, a method for identifying and quantifying compounds in solution), and supplementation improved both PSQI (Pittsburgh Sleep Quality Index) and ISI (Insomnia Severity Index) scores compared to placebo (Liu et al., 2025). GABA produced in the gut reaches the brain through the vagus nerve — the primary neural connection between the gut and the brainstem.
Pathway 2: Butyrate and the Circadian Clock
Butyrate — the short-chain fatty acid produced by Faecalibacterium, Roseburia, and Eubacterium — increased non-REM sleep by roughly 50% when administered orally in mice and 70% via intraportal injection (into the vein connecting the gut to the liver). The sleep-promoting effect did not occur with subcutaneous or intraperitoneal delivery, establishing that butyrate acts via a hepatoportal sensory mechanism — meaning the gut-to-liver vein is the detection route, not general blood circulation (Szentirmai et al., 2019). Gut-produced butyrate has a direct anatomical route to this receptor.
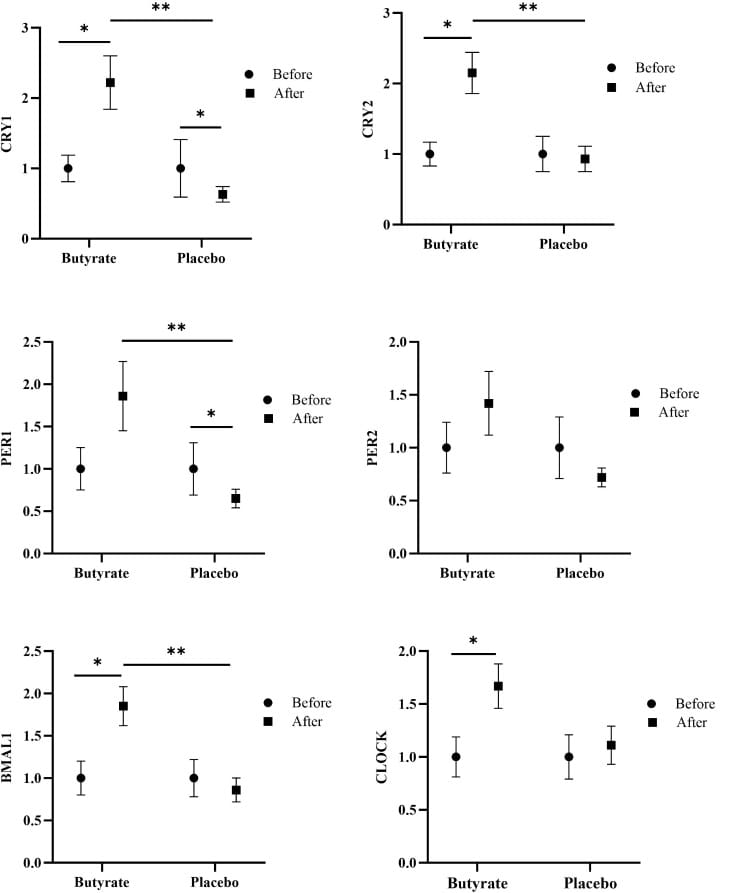
In humans, a 2024 randomized controlled trial found that butyrate supplementation (600 mg/day sodium butyrate for 12 weeks) upregulated circadian clock genes — CRY1, CRY2, PER1, and BMAL1 (all p ≤ 0.005) — while improving PSQI scores by nearly 3 points versus placebo. The placebo group’s sleep worsened during the same period (PSQI change: -2.94 butyrate vs. +1.16 placebo, p < 0.001). This is the first human trial to connect butyrate supplementation to circadian clock gene expression and sleep quality in the same dataset (Firoozi et al., 2024).
Pathway 3: Tryptophan to Serotonin to Melatonin
Approximately 90% of the body’s serotonin is produced in the gut. Gut bacteria metabolize dietary tryptophan into serotonin, which serves as the biochemical precursor for melatonin synthesis in the pineal gland. This pathway is indirect — bacteria do not produce melatonin themselves, but they regulate the raw material supply. When the microbiome is depleted, tryptophan metabolism can divert toward the kynurenine pathway (an inflammatory metabolic route) instead of the serotonin pathway, reducing the substrate available for melatonin production.
Do Probiotics Help with Sleep?
Lee et al. (2021), n = 122: Lactobacillus reuteri NK33 (2.0 x 10^9 CFU) combined with Bifidobacterium adolescentis NK98 (0.5 x 10^9 CFU) for 8 weeks. ISI scores dropped in the probiotic group versus placebo (p = 0.006). The rate of meaningful improvement: 28.6% in the probiotic group versus 11.9% in the placebo group (p = 0.022). IL-6 (interleukin-6, a pro-inflammatory cytokine) also decreased in the probiotic group (p = 0.041), connecting the sleep benefit to reduced inflammation. The gut microbiome changed in composition: Bifidobacteriaceae increased, Enterobacteriaceae and Proteobacteria declined.
Patterson et al. (2024), n = 89: Bifidobacterium longum 1714 for 8 weeks in adults with impaired sleep quality. The PSQI sleep quality component improved at week 4 (p < 0.05), with reduced daytime dysfunction. An honest limitation: actigraphy (objective sleep tracking) did not show differences between groups. The benefit was subjective -- participants reported better sleep, but the wrist-worn device did not detect changes in sleep duration or timing. Subjective improvement without objective confirmation leaves room for placebo effects.
Liu et al. (2025), n = 101: Bifidobacterium animalis BLa80 at 10 billion CFU for 8 weeks. Both PSQI and ISI improved versus placebo. The microbiome moved away from the dysbiotic pattern (reduced Proteobacteria, increased Bacteroidetes). GABA production was confirmed in vitro via HPLC, providing a mechanistic explanation for the sleep benefit.
Ahmad et al. (2025), n = 99: Lactobacillus rhamnosus GG (10 billion CFU) combined with Bifidobacterium longum (5 billion CFU) for 12 weeks. Sleep efficiency improved from 78.5% to 86.2% (p < 0.001) -- a 7.7 percentage point gain that crosses the threshold of what is considered meaningful in sleep medicine. REM sleep latency (the time from sleep onset to the first REM period) decreased by 26 minutes (p < 0.001). Fecal butyrate increased from 12.3 to 16.5 ug/mL (p < 0.001), confirming the short-chain fatty acid mechanism in living subjects rather than in a laboratory dish. Microbial diversity also increased: the Shannon index (a measure of community richness and evenness) rose from 3.8 to 4.2 (p = 0.002).
Does Sleep Deprivation Harm Gut Bacteria?
Sleep deprivation does not just result from a disrupted microbiome — it damages the microbiome in return. The same Proteobacteria elevation seen in people with insomnia appears when sleep is restricted, while beneficial butyrate-producing bacteria decline. This creates a loop: disrupted sleep degrades the microbiome, the degraded microbiome produces less GABA and butyrate, and the reduced metabolite production fragments sleep further.
Two of the probiotic trials provide indirect evidence for breaking this cycle. In the Ahmad et al. (2025) trial, when probiotics increased microbial diversity (Shannon index rose from 3.8 to 4.2, p = 0.002) and butyrate levels climbed, sleep efficiency improved by 7.7 percentage points in the same participants. The Liu et al. (2025) trial showed a parallel pattern: supplementing BLa80 reduced Proteobacteria while improving sleep scores. Both trials suggest that restoring the microbiome can interrupt the downward spiral.
Lee et al. (2021) adds another dimension: in the probiotic group, IL-6 decreased alongside Enterobacteriaceae and Proteobacteria decline. The inflammatory and dysbiotic components moved together. This supports a model where the cycle runs through inflammation as the intermediary — disrupted microbiome composition drives up inflammatory markers, and those inflammatory markers fragment sleep.
Gut-driven inflammation is one contributor to sleep disruption, but it can compound with hormonal changes, metabolic patterns, circadian timing problems, or autonomic dysregulation. Identifying which causes are active helps direct the response.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
Which Gut Bacteria Improve Sleep Duration?
Patterson et al. (2024) found no actigraphy-measured duration change despite subjective sleep quality improvement. Ahmad et al. (2025) improved sleep efficiency (more time asleep within the sleep window) and reduced REM latency, but the gains were architectural — meaning the structure of sleep improved within the existing time frame, not the total hours. Sleep quality scores (PSQI, ISI) and efficiency metrics respond to probiotic supplementation; raw duration has not been reliably shown to change in published trials.
Does the Microbiome Produce Melatonin?
Approximately 90% of the body’s serotonin is produced in the gut. The microbiome regulates the raw material supply for melatonin, but does not produce melatonin itself. When the microbiome is disrupted, tryptophan metabolism can divert toward the kynurenine pathway (an inflammatory route) instead of the serotonin pathway, reducing the substrate available for melatonin. The microbiome’s contribution to melatonin is therefore upstream and indirect: it controls how much tryptophan goes toward serotonin rather than toward inflammatory metabolites.
What Is the Connection Between Irritable Bowel Syndrome and Insomnia?
Firoozi et al. (2024) studied butyrate supplementation in people with ulcerative colitis (a related inflammatory gut condition) and found that sleep quality improved alongside circadian clock gene upregulation and reduced inflammatory markers (fecal calprotectin decreased by 134 units in the butyrate group while increasing by 52 in the placebo group). The gut-brain axis connects intestinal inflammation to brain arousal through both vagal nerve transmission and circulating cytokine release. The relationship is bidirectional: poor sleep worsens gastrointestinal inflammation, and gastrointestinal inflammation fragments sleep.
Related Reading
- Inflammatory Sleep Disruption — the full cause overview covering all inflammatory mechanisms
- Leaky Gut and Insomnia — how gut barrier breakdown and LPS translocation reach the brain
- Chronic Inflammation and Insomnia — the cytokine cycle connecting IL-6, TNF-alpha, and sleep fragmentation
- Brain Fog and Poor Sleep — when neuroinflammation disrupts both cognition and sleep
- Why Is Inflammation Worse at Night? — the NF-kB and circadian clock connection
- Histamine and 3am Waking — why histamine wakes you in the early morning hours
- The Glymphatic Drainage and Sleep — brain waste clearance overnight
- Can Histamine Intolerance Cause Sleep Problems?
- Why Do Men Sleep Worse After 50?
- What Is Autoimmune Insomnia and Why Does It Resist Standard Sleep Approaches?
- Can Inflammation Cause 3am Wakeups?
- Why Does Inflammation Make You Exhausted But Unable to Sleep?
- Can Chronic Stress Cause Insomnia Through Inflammation?
- Does an Anti-Inflammatory Diet Improve Sleep?
References
1. Ahmad, S. R., AlShahrani, A. M., & Kumari, A. (2025). Effects of probiotic supplementation on depressive symptoms, sleep quality, and modulation of gut microbiota and inflammatory biomarkers: A randomized controlled trial. Brain Sciences, 15(7), 761. https://pubmed.ncbi.nlm.nih.gov/40722352/
2. Firoozi, D., Masoumi, S. J., Hosseini Asl, S. M.-K., Labbe, A., Razeghian-Jahromi, I., Fararouei, M., Lankarani, K. B., & Dara, M. (2024). Effects of short-chain fatty acid-butyrate supplementation on expression of circadian-clock genes, sleep quality, and inflammation in patients with active ulcerative colitis: A double-blind randomized controlled trial. Lipids in Health and Disease, 23(1), 216. https://pubmed.ncbi.nlm.nih.gov/39003477/
3. Haimov, I., Magzal, F., Tamir, S., Lalzar, M., Asraf, K., Milman, U., Agmon, M., & Shochat, T. (2022). Variation in gut microbiota composition is associated with sleep quality and cognitive performance in older adults with insomnia. Nature and Science of Sleep, 14, 1753-1767. https://pubmed.ncbi.nlm.nih.gov/36225322/
4. Lee, H. J., Hong, J. K., Kim, J.-K., Kim, D.-H., Jang, S. W., Han, S.-W., & Yoon, I.-Y. (2021). Effects of probiotic NVP-1704 on mental health and sleep in healthy adults: An 8-week randomized, double-blind, placebo-controlled trial. Nutrients, 13(8), 2660. https://pubmed.ncbi.nlm.nih.gov/34444820/
5. Liu, Y., Chen, Y., Zhang, Q., Zhang, Y., & Xu, F. (2025). A double blinded randomized placebo trial of Bifidobacterium animalis subsp. lactis BLa80 on sleep quality and gut microbiota in healthy adults. Scientific Reports, 15(1), 11095. https://pubmed.ncbi.nlm.nih.gov/40169760/
6. Patterson, E., Tan, H. T. T., Groeger, D., Andrews, M., Buckley, M., Murphy, E. F., & Groeger, J. A. (2024). Bifidobacterium longum 1714 improves sleep quality and aspects of well-being in healthy adults: A randomized, double-blind, placebo-controlled clinical trial. Scientific Reports, 14(1), 3725. https://pubmed.ncbi.nlm.nih.gov/38355674/
7. Szentirmai, E., Millican, N. S., Massie, A. R., & Kapas, L. (2019). Butyrate, a metabolite of intestinal bacteria, enhances sleep. Scientific Reports, 9(1), 7035. https://pubmed.ncbi.nlm.nih.gov/31065013/
Written by Kat Fu, M.S., M.S. · Last reviewed: April 2026 · 7 references cited
