Get Ahead of Aging, by Rebuilding Your Sleep First.
I’m not getting those fully alert stretches between bedtime & 3 a.m. anymore, that’s definitely moving in the right direction…really happy I’ve stopped using THC products for sleep and and I’m not feeling that my sleep is so splintered.
age better with better sleep
Sleep recovery to support body and brain

Can’t Sleep More Than 5-6 Hours A night?
Join for evidence-based sleep and aging insights, including client examples of going from short, fragmented sleep to full, continuous sleep windows.
- Why Sleep Gets Easier to Break After Midlifeby Kat Fu, M.S., M.S. on June 1, 2026 at 4:22 pm
Today’s piece is a little different: Scott Anderson interviewed me about sleep after midlife, why a full night can still leave someone unrested, what sleep trackers can show, and why 3 a.m. wakeups often need a more personal read.
- “Why Can’t I Stay Asleep Longer Than 5-6 Hours?”by Kat Fu, M.S., M.S. on May 20, 2026 at 2:03 am
Without Addressing Sleep Architecture After 3AM, You’ll Keep Drifting In and Out Instead of Reaching Deeper Stages
- Does Poor Sleep Make Your Organs Age Faster?by Kat Fu, M.S., M.S. on May 18, 2026 at 5:17 pm
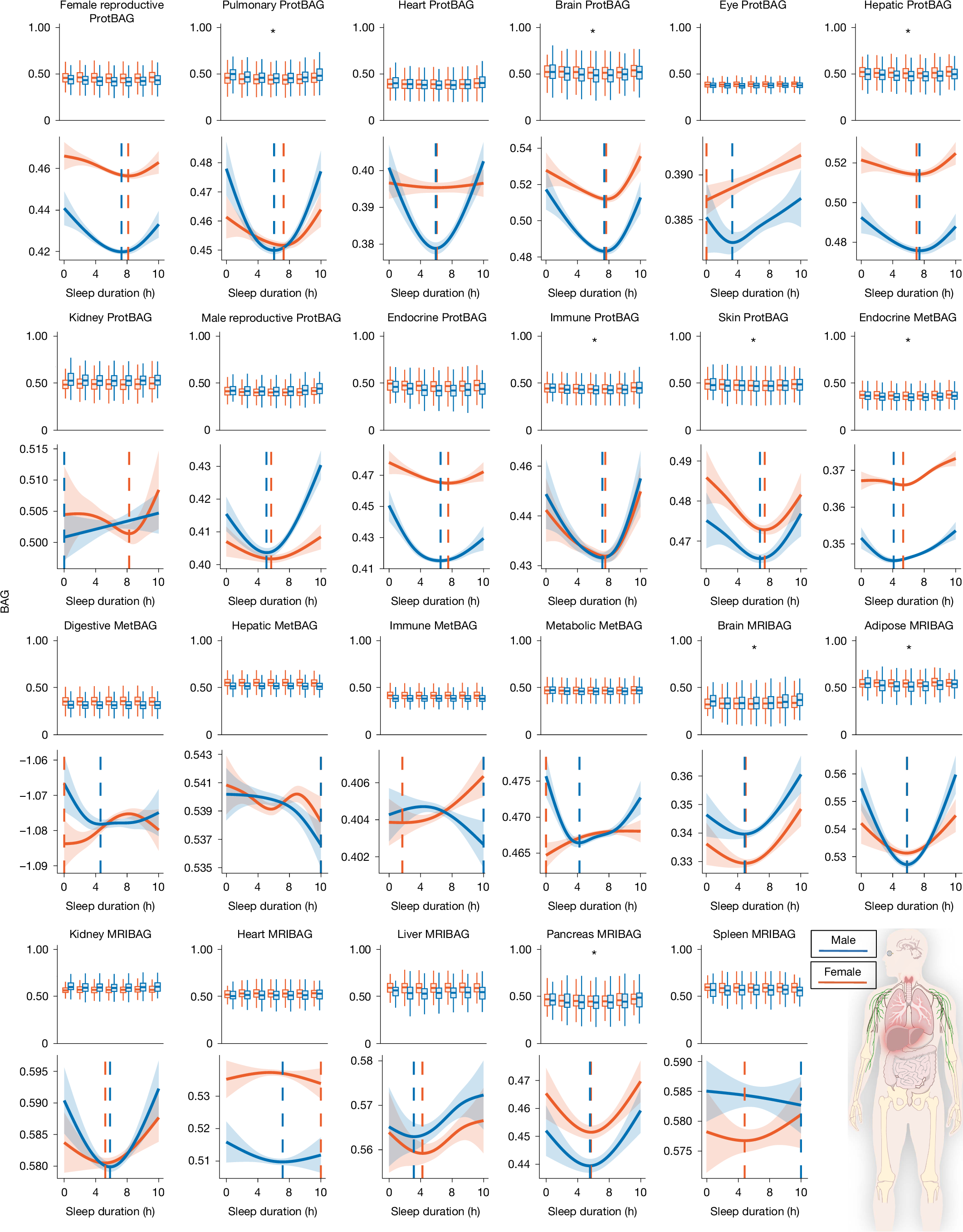
A just-published Nature study, “Sleep chart of biological ageing clocks in middle and late life,” asked a simple but important question: does sleep duration line up with how quickly different parts of the body appear to be ageing?The researchers used large biobank datasets, especially UK Biobank, and compared self-reported sleep duration with 23 biological ageing clocks built from three data layers:MRI imaging,plasma proteins, andmetabolites.In plain English, these clocks estimate whether a person’s brain, liver, immune system, pancreas, adipose tissue, and other systems look biologically “older” or “younger” than expected for their actual age.The study focused on adults in middle and later life, with UK Biobank participants aged roughly 37–84 years.The key concept is the biological age gap, or BAG. A higher BAG means a system looks older than expected for someone’s chronological age; a lower BAG means it looks closer to, or younger than, expected.
- Does Growth Hormone Affect Dementia Risk?by Kat Fu, M.S., M.S. on May 11, 2026 at 3:22 pm
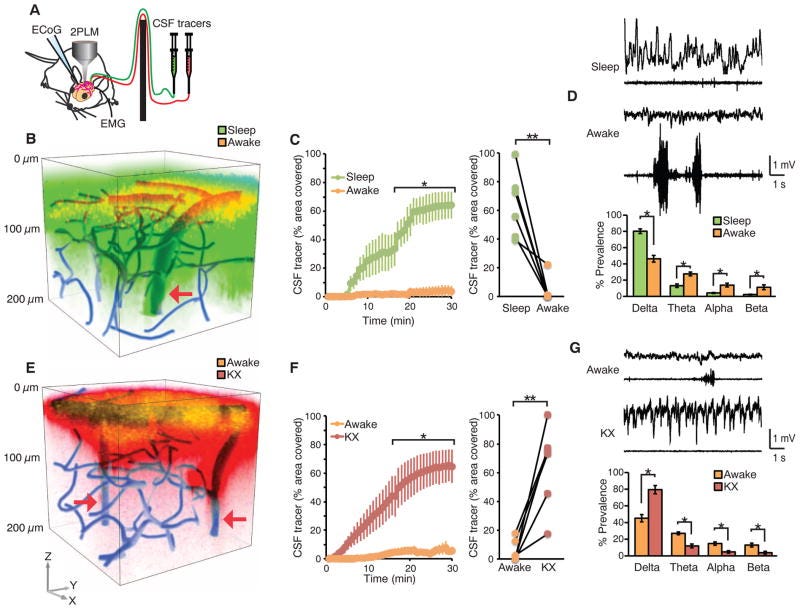
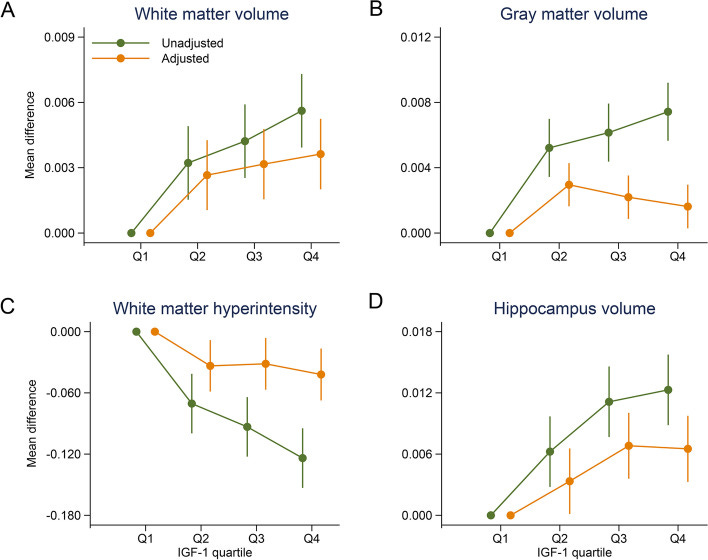
Growth hormone usually enters the longevity conversation through body composition.That makes sense.Growth hormone affects muscle, bone, fat metabolism, and tissue repair. But growth hormone also sits inside a larger overnight process that includes sleep depth, brain health and dementia.In a UK Biobank analysis of 369,711 adults, IGF-1 – the hormone the liver produces in response to growth hormone – tracked hippocampal volume.Specifically, lower IGF-1 was associated witha smaller hippocampus,less white matter volume, andmore white matter lesions.The study adjusted for sex, age, ethnicity, educational attainment, smoking status, alcohol intake frequency, vegetable and fruit intake, body mass index, hypertension, diabetes, total cholesterol, and C-reactive protein.In a separate long-term study, adults in the lowest IGF-1 quartile had a 51% higher risk of developing Alzheimer’s dementia over 7.4 years.Growth hormone is also tied to the part of sleep that matters for overnight restoration. The largest growth hormone release of the 24-hour cycle usually occurs during the first 60-90 minutes of sleep, when slow-wave sleep is deepest.During slow-wave sleep, cerebrospinal fluid movement through the glymphatic pathway increases. Recent human data show that sleep-active clearance helps move amyloid beta and tau (proteins involved in Alzheimer’s disease pathology) from brain tissue.But is more growth hormone better?In this article we’ll discuss:what the longevity data supports in relation to growth hormonewhich factors support healthy growth hormone functionwhich factors disrupt growth hormone release or reduce IGF-1 ( insulin-like growth factor-1) response9 things you can do today, to improve growth homone function for optimal brain health & longevity without using peptides or exogenous hormones, regardless of your ageLet’s get started.
- Is the gut-sleep link finally real, or wellness hype?by Kat Fu, M.S., M.S. on May 4, 2026 at 4:12 pm
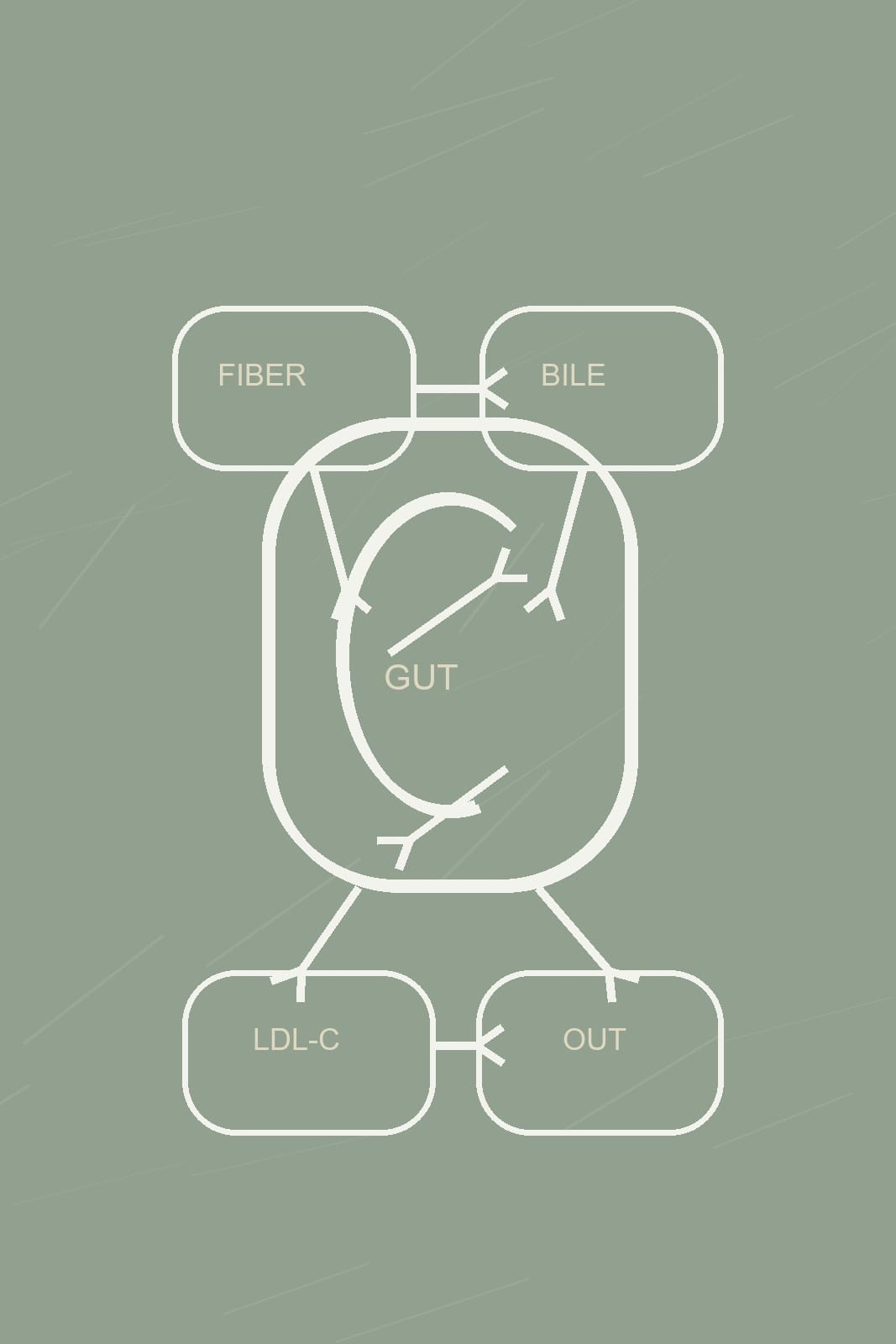
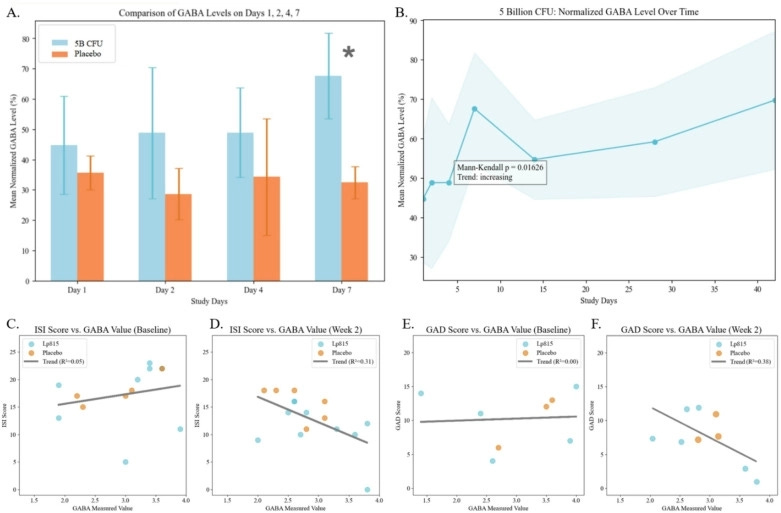
What if your gut was influencing how well you sleep each night?GABA — gamma-aminobutyric acid — is one of the brain’s main calming molecules, and many sleep medicines work by boosting its effects. Gut microbes can also make GABA. But whether that gut-made GABA reaches the brain, and whether it matters for sleep, is a question the field is only now beginning to answer with human data.GABA in blood is thought to reach the brain in only small amounts, if at all, under typical conditions — and human evidence about GABA crossing the blood–brain barrier is currently limited. Few human studies measure gut GABA and sleep at the same time, and even fewer also measure brain GABA.So does gut-produced GABA affect human sleep — and if so, how?This review will discuss:What is gut-produced GABA, and how do microbes make it?What pathways exist for gut-made GABA to affect human sleep (even if it does not cross the blood-brain-barrier)?Human evidence linking gut GABA to sleepPractical implications: is optimizing gut-made GABA a practical strategy for improving your sleep?
- What Causes Circadian Sleep Disruption? 10 Underappreciated Factorsby Kat Fu, M.S., M.S. on April 27, 2026 at 3:37 pm
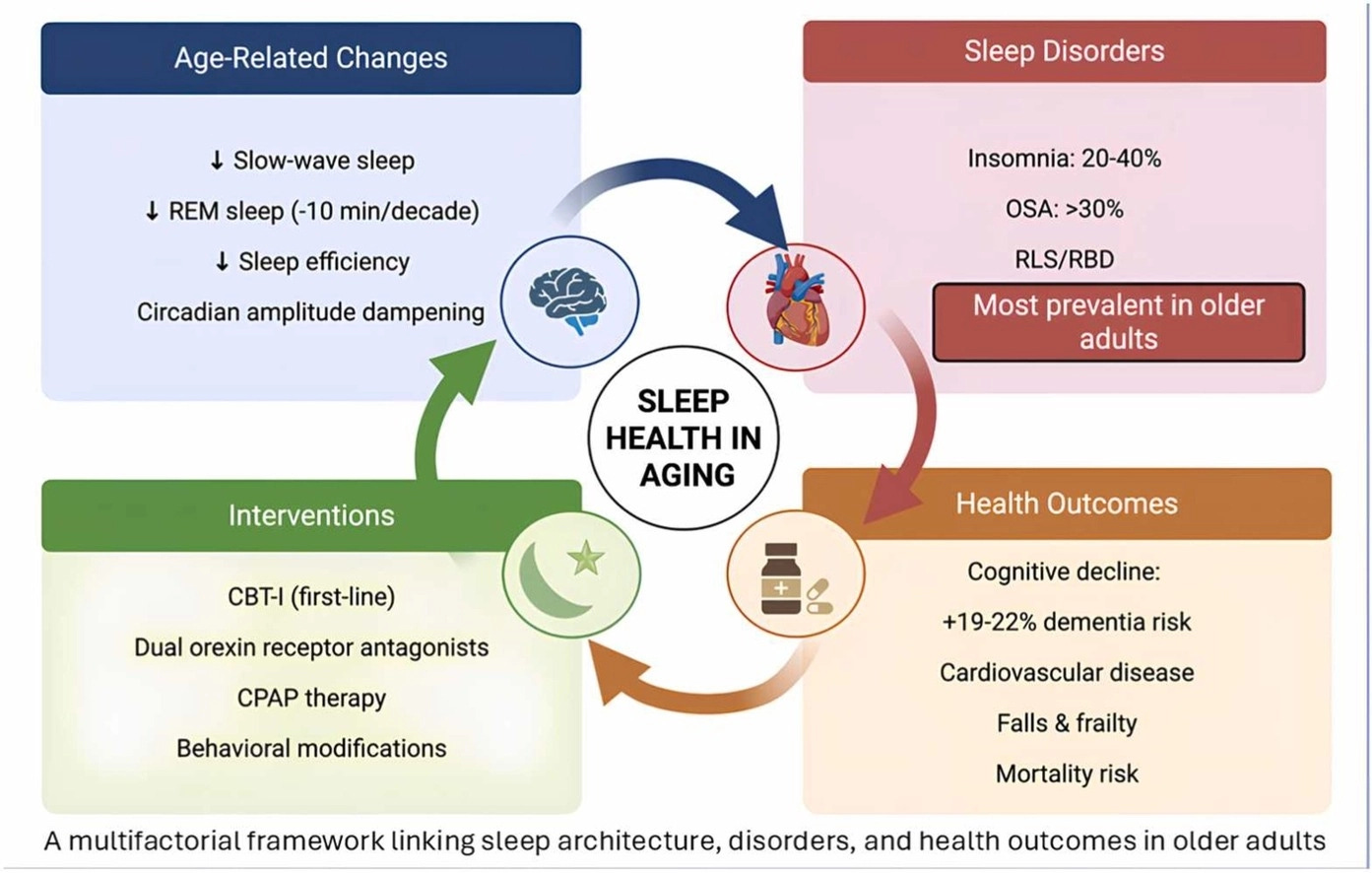
The suprachiasmatic nucleus is the master pacemaker, but it is not the only clock. Every organ — the liver, gut, kidneys, adrenal glands, skeletal muscle — has its own peripheral clock running the same molecular loop. The suprachiasmatic nucleus synchronizes these peripheral clocks through neural projections, hormones (including cortisol and melatonin), and autonomic nervous output (Albrecht, Neuron, 2012).When circadian timing is intact, these distributed clocks coordinate: body temperature drops in the evening, melatonin rises, cortisol falls, and the brain transitions from wakefulness into consolidated sleep. When circadian timing breaks down, each of these coordinated outputs can go wrong independently.The health consequences of circadian disruption extend beyond sleep: cardiovascular risk, metabolic regulation, cognitive function, and immune timing are all circadian-controlled.How Does Circadian Disruption Fragment Sleep and Contribute to 3AM Wakeups and Light Shallow Sleep?Circadian disruption fragments sleep through multiple independent pathways: mistimed wake-promoting orexin neurons that intrude into sleep, peripheral organ clocks that decouple from the brain’s master clock, a thermoregulatory gate that doesn’t open on schedule, a cortisol rhythm that advances too early, and a melatonin timing cue that moves the sleep window away from intended bedtime.