When the body cannot break down histamine efficiently, the brain’s wakefulness circuits stay active through the night — and standard sleep supplements that interact with mast cell pathways can compound the problem rather than resolve it. Addressing histamine clearance is what improves sleep quality, daytime energy, and cognitive function over time. This article covers how diamine oxidase enzyme deficiency connects to insomnia, why common sleep remedies can worsen sleep when histamine is elevated, what the research shows about histamine-targeted approaches, and how mast cell activation extends that disruption. Histamine-driven sleep disruption is one of several inflammatory mechanisms — for the broader picture, see Inflammatory Sleep Disruption.
What Is Histamine Intolerance and How Does It Affect Sleep?
Histamine is one of the brain’s primary wake-promoting neurotransmitters. Histaminergic neurons in the tuberomammillary nucleus (TMN) — a small cluster in the posterior hypothalamus — fire during wakefulness and stop firing during sleep (Thakkar, 2011). When histamine levels stay elevated because the body cannot degrade histamine efficiently, that wakefulness drive persists into the night.
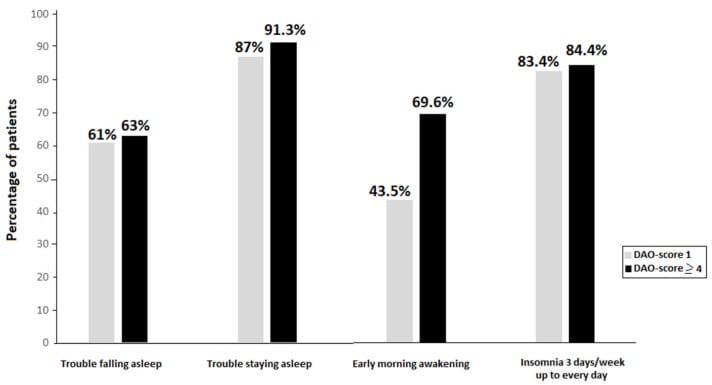
The enzyme responsible for breaking down histamine in the gut and bloodstream is diamine oxidase (DAO). Genetic variants in the AOC1 gene — the gene encoding DAO — reduce the body’s capacity to degrade histamine from food and from endogenous mast cell release. In a 2024 cross-sectional study of 167 adults presenting with insomnia, 82.6% carried AOC1 variants associated with DAO deficiency. Among those with higher genetic burden (four or more single nucleotide polymorphisms), rates of sleep maintenance problems and early morning awakening were elevated compared to those with fewer variants (López García et al., 2024).
The insomnia pattern in histamine intolerance tends to look different from stress-related or circadian-related sleep problems. The predominant complaint in López García’s cohort was difficulty staying asleep (88%), followed by difficulty falling asleep (60.5%). That maintenance-dominant pattern — falling asleep at a reasonable time but waking repeatedly or too early — is consistent with elevated histamine keeping the TMN wakefulness pathway active during the second half of the night.
Beyond sleep, histamine intolerance produces a constellation of overlapping presentations. In a review of 77 individuals with histamine intolerance, Hrubisko et al. (2021) documented respiratory issues in 95%, bloating in 94%, headache in 91%, fatigue in 83%, and postprandial drowsiness in 81%. The drowsiness-fatigue combination is often misattributed to poor sleep alone, when the underlying histamine excess is driving both the daytime fatigue and the nighttime waking.
One reason histamine intolerance goes unrecognized for so long: the presentations vary from episode to episode in the same person after similar exposures, making it difficult to identify a pattern.
What Is the Diamine Oxidase Enzyme and How Does It Affect Sleep?
DAO is produced in the intestinal mucosa. Its primary job is to degrade histamine before it enters the bloodstream. When DAO activity is sufficient, dietary histamine — from aged cheeses, fermented foods, cured meats, alcohol — gets broken down in the gut. When DAO activity is low, that histamine passes into circulation and adds to whatever histamine the body is already producing through mast cell activity.
Several factors reduce DAO activity beyond genetics. Gut inflammation can damage the intestinal cells that produce DAO. Alcohol inhibits DAO directly. Certain medications — including some NSAIDs, antidepressants, and antiarrhythmics — also reduce DAO function (Hrubisko et al., 2021).
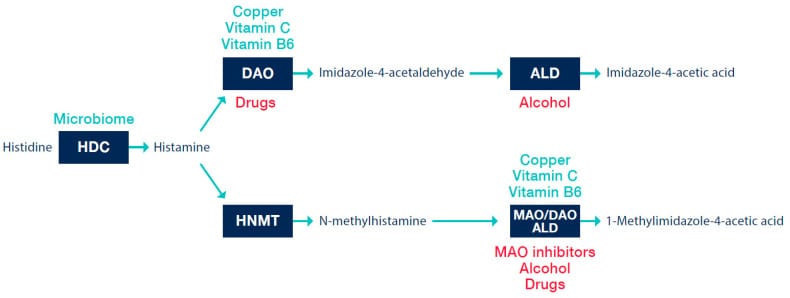
When a genetic predisposition toward low DAO combines with any of these factors, nighttime histamine levels can remain elevated through the hours when TMN wakefulness neurons should be ceasing to fire.
The connection between DAO support and sleep improvement has recent evidence. In a 2025 randomized, double-blind, placebo-controlled trial, 101 adults with insomnia and confirmed AOC1 gene variants received either DAO supplementation or placebo for 28 days. The DAO group showed improvements in Pittsburgh Sleep Quality Index scores — including sleep efficiency and reduced sleep medication use — compared to placebo. Among participants who were also taking melatonin, insomnia severity improvements were greater in the DAO group at both day 7 and day 28 (Ferrer-Garcia et al., 2025).
The DAO-plus-melatonin finding matters. For people whose insomnia involves histamine accumulation, melatonin alone may be insufficient because it does not address the histamine excess. Adding DAO enzyme support allows melatonin to do what melatonin does well: support circadian-driven sleep onset. Without addressing the histamine burden first, melatonin is working against a wakefulness drive it was not designed to override.
The mechanistic link is direct: histamine promotes wakefulness through H1 receptor activation in the TMN. Histaminergic neurons fire exclusively during wakefulness and cease firing during NREM and REM sleep (Thakkar, 2011). Reducing circulating histamine — whether through DAO supplementation, dietary histamine reduction, or both — lowers the substrate that keeps the TMN active at night.
Can Mast Cell Activation Syndrome Cause Insomnia?
Mast cell activation syndrome (MCAS) is a condition in which mast cells degranulate inappropriately — releasing inflammatory mediators without a true allergic trigger. Where histamine intolerance involves impaired breakdown of histamine, MCAS involves excessive production and release of histamine alongside many other mediators.
MCAS carries a heavy sleep burden. Weinstock et al. (2025) surveyed 553 individuals with MCAS and 558 controls and found that insomnia was among the neuropsychiatric conditions elevated in MCAS across both sexes. Women with MCAS reported higher rates of neurologic and psychiatric conditions in 18 of 19 categories studied; men in 17 of 19. When those with MCAS rated the effectiveness of various approaches for their neuropsychiatric presentations, antihistamines received a rating of 6.3 out of 10 — outperforming benzodiazepines at 5.6 out of 10. That finding is relevant: it suggests that addressing histamine and mast cell mediators directly is more effective for MCAS-related insomnia than broad sedation with a drug that does not touch the inflammatory drive.
MCAS also creates sleep disruption through pathways beyond histamine alone. Weinstock et al. (2020) found that 40.8% of individuals with MCAS had restless legs syndrome, compared to 12.9% of spouse controls. In women with MCAS, the prevalence was 6.7 times higher than in age-matched American women. Restless legs syndrome disrupts sleep onset and sleep maintenance independently — meaning people with MCAS can face both histamine-driven early awakening and movement-related sleep fragmentation at the same time.
The compounding nature of MCAS is what distinguishes it from isolated histamine intolerance. When mast cells degranulate, they release histamine, but also prostaglandins, serotonin, cytokines (including TNF-alpha and IL-6), and tryptase. Each of these mediators disrupts sleep through a different mechanism. This is why people with MCAS often describe their insomnia as resistant to every approach they have tried: each remedy addresses one pathway while several others remain active.
Why Do Standard Sleep Remedies Make Histamine Intolerance Worse?
Melatonin is typically the first supplement people reach for when sleep is disrupted. And at a molecular level, melatonin does interact with mast cells beneficially: it suppresses NF-kB activation, which in turn reduces mast cell degranulation and histamine release. Melatonin also binds to MT1 and MT2 receptors and can down-regulate mast cell proliferation (Pham et al., 2021).
In a person with normal mast cell function, this pathway works — melatonin rises in the evening, mast cell activity decreases, histamine levels fall, and the TMN wakefulness neurons cease firing. When mast cell activation is pathologically elevated — as in MCAS or severe histamine intolerance — the volume of mast cell degranulation overwhelms melatonin’s inhibitory capacity. Taking more melatonin adds to a pathway that is already being overridden (Pham et al., 2021).
Mast cells also follow circadian activation patterns. Clock genes — Clock, Bmal1, Per1/2, Cry1/2 — regulate mast cell quantity and degranulation timing. The IgE/FcεRI and IL-33/ST2 mast cell activation pathways both show time-of-day variation (Pham et al., 2021). This circadian regulation of mast cells explains why histamine-related insomnia tends to cluster in the early morning hours — between roughly 2 and 4 AM — when the circadian mast cell activation peak coincides with the lowest point of cortisol’s anti-inflammatory influence.
Magnesium is another supplement that frequently worsens histamine-driven insomnia. Magnesium glycinate — one of the widely recommended forms for sleep — can trigger histamine release in individuals with mast cell sensitivity. The glycine component can interact with mast cell pathways, and the result is paradoxical waking rather than deeper sleep.
Other common sleep-adjacent supplements carry the same risk. 5-HTP can increase serotonin, which in turn activates mast cells. Fermented supplements — including some probiotic formulations — contain histamine or histamine-producing bacteria. B6 in certain forms can accelerate histamine production. For someone with impaired histamine clearance, each of these adds to an already excessive histamine load.
This creates a recognizable pattern: cycling through supplement after supplement, finding that each new remedy either does nothing or makes sleep worse. The supplements are not ineffective in general — they are being added on top of an unaddressed histamine burden. Addressing histamine clearance first — through DAO support, dietary histamine reduction, or targeted antihistamine use — changes the equation. Once the histamine load is managed, supplements like melatonin can function as intended.
Histamine-driven waking might be compounding with other causes — autonomic dysregulation, metabolic disruption, hormonal shifts, or circadian misalignment might all be active at the same time. Identifying which causes might be involved is a useful next step before adding or changing anything.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
What Are the Presentations of Histamine Intolerance at Night?
The 2-to-4 AM waking window is the hallmark. This timing corresponds to the circadian peak in mast cell activation and the nadir of cortisol’s anti-inflammatory capacity. People often describe the waking as abrupt — not a gradual return to consciousness but a sudden alertness, sometimes accompanied by a racing heart or a feeling of anxiety that has no obvious emotional cause.
Nasal congestion that appears at night or upon waking is another common indicator. Histamine causes vasodilation and increased mucous production in the nasal passages. Flushing — warmth or redness in the face, ears, or chest — can accompany the waking episode. Some people report urgency to urinate, which results from histamine’s effect on smooth muscle contraction in the bladder.
Cortisol-driven early waking tends to involve a wired, alert feeling paired with hunger — the body mobilizing glucose. Histamine-related waking tends to involve more inflammatory-type presentations: congestion, itching, flushing, heart rate changes. Both can produce anxiety, but the physical accompaniments differ.
Is Waking Up Itchy at Night a Sign of Histamine Intolerance?
Histamine is one of the primary mediators of itch sensation. When circulating histamine levels rise — as they do during the nighttime mast cell activation peak — itch perception increases even in the absence of a local skin condition. This is why people with histamine intolerance may experience itching that moves around the body, appears and disappears unpredictably, and leaves no visible mark.
The absence of a visible rash is a distinguishing feature. Eczema and contact dermatitis produce visible inflammation at the itch site. In histamine intolerance, the itch is driven by circulating histamine acting on nerve endings rather than by a local inflammatory process in the skin. When nocturnal itching appears alongside other histamine intolerance indicators — waking between 2 and 4 AM, nasal congestion, flushing, digestive issues after high-histamine meals — the combination points toward histamine as a common contributor.
Does a Low-Histamine Diet Improve Sleep?
The reasoning is direct: the body has a finite capacity to break down histamine. If dietary histamine from aged cheese, wine, fermented foods, smoked fish, and cured meats is consuming a large portion of that capacity, reducing those foods lowers the total histamine the body must process — including overnight, when histamine elevation disrupts sleep.
Hrubisko et al. (2021) identified a low-histamine diet as one of the evidence-supported management approaches for histamine intolerance. In practice, many people report that eliminating high-histamine foods — particularly at dinner — leads to fewer nighttime awakenings and reduced congestion upon waking.
The limitation is that dietary histamine is only one input. In people with MCAS or high endogenous mast cell activity, the body produces enough histamine internally that dietary restriction alone may not reduce the total burden enough to resolve sleep disruption. A low-histamine diet tends to work better when combined with DAO support and, where appropriate, antihistamine use — addressing both the external and internal histamine sources.
Why Do Antihistamines Make You Sleepy?
Histaminergic neurons in the tuberomammillary nucleus fire exclusively during wakefulness. Their primary receptor target for maintaining wakefulness is the H1 receptor. When a first-generation antihistamine like diphenhydramine crosses into the brain and blocks H1 receptors, it removes the histamine-driven wakefulness input — and the result is drowsiness (Thakkar, 2011).
This is also why antihistamines can be more effective than standard sedatives for people with histamine intolerance or MCAS. A benzodiazepine or an orexin antagonist works by suppressing brain activity broadly — but it does not address the histamine excess that is driving the wakefulness in the first place. An antihistamine targets the overactive wake-promoting pathway directly. Weinstock et al. (2025) found that individuals with MCAS rated antihistamines 6.3/10 for neuropsychiatric relief compared to benzodiazepines at 5.6/10 — consistent with the idea that addressing the histamine pathway directly is more effective than general sedation when histamine is the primary driver.
Second-generation antihistamines (cetirizine, loratadine) are designed not to cross the blood-brain barrier, which is why they relieve allergy presentations without causing drowsiness.
Related Reading
- Inflammatory Sleep Disruption — the full cause overview covering all five inflammatory mechanisms
- Why Does Histamine Wake You Up at 3am? — how brain-resident mast cells and the circadian histamine peak drive early-morning waking
- Why Is Inflammation Worse at Night? — how NF-kB and the circadian clock create a pre-dawn inflammatory vulnerability window
- How Does Leaky Gut Affect Sleep? — how gut permeability and LPS translocation trigger neuroinflammation that fragments sleep
- Does Poor Sleep Cause Brain Inflammation? — the bidirectional loop between neuroinflammation, brain fog, and sleep loss
- How Does the Glymphatic System Work During Sleep? — how the brain’s waste clearance pathway depends on deep sleep
- What Is the Connection Between Chronic Inflammation and Insomnia? — the wired-but-tired cycle of cytokines, sleep loss, and 24-hour hyperarousal
- Why Do Men Sleep Worse After 50?
- What Is Autoimmune Insomnia and Why Does It Resist Standard Sleep Approaches?
- Can Inflammation Cause 3am Wakeups?
- Why Does Inflammation Make You Exhausted But Unable to Sleep?
- Can Chronic Stress Cause Insomnia Through Inflammation?
- Gut Bacteria and Insomnia: Which Microbes Affect Your Sleep (and Which Ones Help)
- Does an Anti-Inflammatory Diet Improve Sleep?
References
1. López García, R., Ferrer-Garcia, J., Sansalvador, A., & Quera-Salva, M.-A. (2024). Prevalence of diamine oxidase enzyme (DAO) deficiency in subjects with insomnia-related symptoms. Journal of Clinical Medicine, 13(16), 4583. https://pubmed.ncbi.nlm.nih.gov/39200725/
2. Ferrer-Garcia, J., Navarro, M. D., Abadias, M., López-García, R., Sansalvador, A., Gris, G., & Uscamaita, K. (2025). Effect of diamine oxidase (DAO) enzyme dietary supplementation in subjects with insomnia symptoms and single nucleotide polymorphisms of the AOC1 gene: A randomized double-blind placebo-controlled study. Sleep Medicine X, 11, 100167. https://pubmed.ncbi.nlm.nih.gov/41437955/
3. Hrubisko, M., Danis, R., Huorka, M., & Wawruch, M. (2021). Histamine intolerance-the more we know the less we know. A review. Nutrients, 13(7), 2228. https://pubmed.ncbi.nlm.nih.gov/34209583/
4. Pham, L., Baiocchi, L., Kennedy, L., Sato, K., Meadows, V., Meng, F., Huang, C.-K., Kundu, D., Zhou, T., Chen, L., Alpini, G., & Francis, H. (2021). The interplay between mast cells, pineal gland, and circadian rhythm: Links between histamine, melatonin, and inflammatory mediators. Journal of Pineal Research, 70(2), e12699. https://pubmed.ncbi.nlm.nih.gov/33020940/
5. Weinstock, L. B., Afrin, L. B., Reiersen, A. M., Brook, J., Blitshteyn, S., Ehrlich, G., Schofield, J. R., Kinsella, L., Kaufman, D., Dempsey, T., & Molderings, G. J. (2025). Prevalence and treatment response of neuropsychiatric disorders in mast cell activation syndrome. Brain, Behavior, and Immunity – Health, 48, 101048. https://pubmed.ncbi.nlm.nih.gov/40686928/
6. Weinstock, L. B., Walters, A. S., Brook, J., Kaleem, Z., Afrin, L. B., & Molderings, G. J. (2020). Restless legs syndrome is associated with mast cell activation syndrome. Journal of Clinical Sleep Medicine, 16(3), 401–408. https://pubmed.ncbi.nlm.nih.gov/31994488/
7. Thakkar, M. M. (2011). Histamine in the regulation of wakefulness. Sleep Medicine Reviews, 15(1), 65–74. https://pubmed.ncbi.nlm.nih.gov/20851648/
Written by Kat Fu, M.S., M.S. · Last reviewed: April 2026 · 7 references cited
