Search “best probiotics for sleep” and the results are supplement listicles. What those pages lack is the strain-level evidence — which bacteria have been tested in human trials for sleep outcomes, what the effect sizes were, and why the vagus nerve is the required relay between gut bacteria and brain function.
This article covers the strains with human sleep trial data, the meta-analytic evidence across 11+ RCTs, and the vagotomy proof that probiotics require an intact vagus nerve to reach the brain. For the gut-vagus-GABA pathway, see How Your Gut Talks to Your Brain Through the Vagus Nerve — and Why It Matters for Sleep. For the full autonomic overview — cortisol-driven hyperarousal, parasympathetic insufficiency, cholinergic REM regulation — see Autonomic Sleep Disruption.
Which Probiotic Strains Have Human Trial Evidence for Sleep?
Bifidobacterium longum 1714. Moloney et al. (2021) conducted a placebo-controlled crossover study in 20 healthy male students during exam stress. Sleep duration improved in the B. longum 1714 group during the exam period compared to placebo (p = 0.039). Stress and depression scores increased in both groups at comparable rates — the probiotic did not reduce stress perception but acted on sleep parameters independently. No improvements were found in working memory, sustained attention, or perception, indicating a sleep-focused rather than broad cognitive effect.
Lactobacillus gasseri CP2305. Nishida et al. (2017) enrolled 32 medical students (21 males, 11 females) consuming heat-killed L. gasseri CP2305 daily for five weeks during cadaver dissection coursework. Sleep quality improved in the probiotic group compared to placebo (p = 0.038). Male participants showed decreased sleep latency (p = 0.035) and increased sleep duration (p = 0.048). An important caveat: female students in the probiotic group experienced aggravated stress scores (p = 0.029), indicating biological sex moderates the response. CP2305 is a heat-killed preparation (paraprobiotic), meaning live bacteria are not required for this strain’s sleep-modulating effects through the gut-brain axis.
Lactobacillus helveticus R0052 + Bifidobacterium longum R0175. Messaoudi et al. (2011) tested this two-strain combination in both rats and a 30-day double-blind human trial in healthy volunteers. The probiotic group showed improved Hopkins Symptom Checklist (HSCL-90) global severity scores (p < 0.05), reduced depression and anger-hostility subscales (p < 0.05), and decreased urinary free cortisol (p < 0.05). Sleep improvement in this trial may occur through HPA axis downregulation — reduced cortisol output reduces the cortisol-driven arousal that fragments sleep.
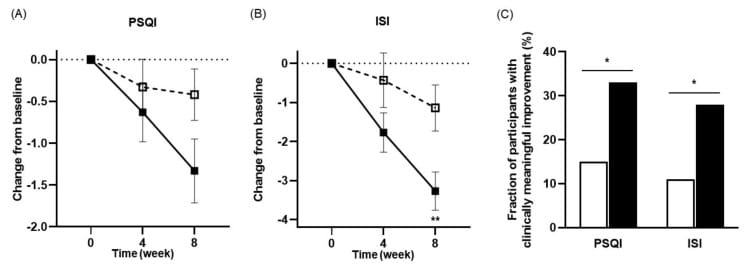
NVP-1704 (L. reuteri NK33 + B. adolescentis NK98). Lee et al. (2021) enrolled 156 adults with subclinical depression, anxiety, and insomnia in an 8-week double-blind trial. Insomnia Severity Index (ISI) scores improved at 8 weeks (−3.27 vs. −1.14, p = 0.006). PSQI trends approached but did not reach statistical significance (−1.33 vs. −0.42, p = 0.068), though the proportion of participants with PSQI improvement was 33.3% in the probiotic group versus 15.3% in placebo (p = 0.021). Serum interleukin-6 decreased in the probiotic group (−0.23 pg/mL) while increasing in placebo (+0.20 pg/mL, p = 0.041) — implicating anti-inflammatory mechanisms alongside the sleep changes.
Multi-strain formulation (2024). Kerksick et al. (2024) enrolled 70 healthy adults in a 6-week double-blind trial using a 4-strain formula containing Limosilactobacillus fermentum, Lacticaseibacillus rhamnosus, Lactiplantibacillus plantarum, and Bifidobacterium longum at 4 x 10^9 live cells per day. The probiotic group showed improvements in PSQI global scores (p < 0.05), with gains in sleep latency and sleep disturbance subscores. Actigraphy-based objective sleep measures — hours asleep, minutes awake, number of awakenings — showed no differences between groups. The improvements were in subjective sleep perception rather than objective sleep architecture, a pattern that recurs across the probiotic-sleep literature.
What Does the Meta-Analytic Evidence Show?
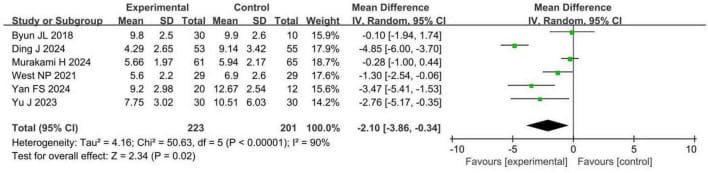
Liu et al. (2025) published the only insomnia-focused meta-analysis to date, pooling 6 RCTs encompassing 424 participants (223 probiotic, 201 control) from China, Japan, South Korea, and Australia. Probiotic supplementation reduced PSQI scores by a mean difference of 2.10 points (95% CI: −3.86 to −0.34, p = 0.02). PSQI scores of 5 or higher define poor sleep quality, so a 2.10-point reduction can move an individual from the “poor sleep” range into the normal range — this crosses the minimally important difference threshold for many people.
Hamilton Depression Scale scores also declined by 7.72 points in probiotic groups compared to controls (p = 0.03), reflecting the bidirectional relationship between insomnia and depression. No clear effects were detected for objective parameters — total sleep time, sleep efficiency, or sleep latency — suggesting that in short-term trials, probiotics affect perceived sleep quality rather than polysomnographically measurable sleep architecture. No statistically significant differences in adverse events were found between probiotic and placebo groups.
Yu et al. (2024) conducted a broader meta-analysis of 11 RCTs covering both diagnosed sleep disorders and stress-induced sub-healthy sleep. The pooled effect was a standardized mean difference of −0.34 (95% CI: −0.56 to −0.13, p = 0.001) — a small but reliable effect. Subgroup analyses identified four moderators: baseline health status, duration of supplementation, strain used, and measurement instrument. Both live probiotics and heat-killed paraprobiotics (including L. gasseri CP2305) demonstrated sleep benefits, confirming that microbial viability is not a prerequisite for gut-brain sleep effects.
Sivamaruthi et al. (2025) published a review of human RCTs and identified Lactobacillus and Bifidobacterium among the genera with published sleep evidence across RCTs. The review identified several mechanisms supported by the literature, including improvement of gut microbiota composition, intestinal integrity, blood-brain barrier function, and neurotransmitter regulation.
Why Do Probiotics Need the Vagus Nerve to Affect Sleep?
Bravo et al. (2011) published the landmark experiment in PNAS. Chronic oral administration of Lactobacillus rhamnosus JB-1 to mice produced region-dependent changes in brain GABA receptor expression. GABA(B1b) receptor mRNA increased in cingulate and prelimbic cortical regions while decreasing in hippocampus, amygdala, and locus coeruleus. Treated mice entered open arms of the elevated plus maze more than controls (p < 0.001), showed reduced immobility in the forced swim test (p < 0.01), and had lower stress-induced corticosterone (p < 0.001).
The vagotomy arm is what made this study causal. A second group of mice received the same probiotic after surgical vagotomy. The behavioral effects and amygdala GABA receptor changes were abolished. GABA receptor changes in the amygdala were prevented, though some hippocampal changes persisted. Corticosterone suppression did not occur. Behavior did not improve. The bacteria were still alive in the gut, still producing metabolites — but without the vagus nerve to carry the information, the behavioral and stress-hormone effects did not emerge. The full vagotomy evidence — how scientists proved probiotics reach your brain through the vagus nerve — is covered in detail here.
Moerkl et al. (2025) extended this to humans. In a randomized controlled trial of 86 participants — 40 with major depressive disorder and 46 healthy controls — a multi-species probiotic improved morning vagal nerve function measured by heart rate variability (HRV) in the MDD subgroup. This is one of the first RCTs to use vagal tone as a probiotic endpoint, and the results indicate that probiotics can measurably increase parasympathetic nervous system activity in people with depression — the same vagal pathway the Bravo mouse study identified as the required relay.
A translation caveat is necessary. Kelly et al. (2017) tested the same JB-1 strain from the Bravo mouse study in a 29-person human RCT for stress and cognition. The strain did not replicate its mouse effects in humans. This does not invalidate the vagus nerve mechanism — other strains (B. longum 1714, L. gasseri CP2305) have stronger human evidence — but it illustrates that mouse-to-human translation is not automatic for any single strain. The mechanism (vagal relay) is supported; the JB-1 strain did not translate. For how to measure vagal function yourself, see What Your Overnight Heart Rate Variability Is Telling You About Your Sleep.
How Should You Choose a Probiotic for Sleep?
Strain-level identification matters. A product label reading “Lactobacillus rhamnosus” without a strain designator tells you the genus and species but not the strain. Lactobacillus rhamnosus GG, L. rhamnosus JB-1, and L. rhamnosus from the Kerksick 2024 multi-strain trial are different organisms with different evidence profiles. The JB-1 strain showed anxiolytic effects in mice but did not replicate in a human trial (Kelly et al., 2017). L. rhamnosus in the multi-strain formulation contributed to PSQI improvement (Kerksick et al., 2024). Same species, different outcomes. Look for the full strain number on the label.
Dose matching. Trial doses across the studies reviewed here ranged from 1 x 10^9 to 10 x 10^9 CFU per day. The Kerksick 2024 multi-strain trial used 4 x 10^9 live cells daily. The Moloney 2021 trial of B. longum 1714 used 1 x 10^9 CFU. Products providing less than 1 x 10^9 CFU of the relevant strain have no trial data supporting their use for sleep.
Multi-strain vs. single-strain. The meta-analytic evidence supports both approaches. Multi-strain formulations (Kerksick et al., 2024; Yu et al., 2024) produced subjective sleep improvements and may address broader gut ecology. Single-strain products allow you to match the organism tested in a trial — B. longum 1714 for stress-related sleep disruption, L. gasseri CP2305 for sleep latency.
Timeline expectations. The Moloney 2021 trial of B. longum 1714 measured improvements during an exam period spanning several weeks. The Lee 2021 NVP-1704 trial found ISI improvements at 8 weeks. The Kerksick 2024 multi-strain trial found PSQI improvements within 6 weeks. Across the literature, 4-8 weeks is the window where sleep effects have been measured. For the evidence-based timeline of what to expect week by week, see the probiotic sleep timeline. For the reverse direction — how poor sleep disrupts the gut microbiome — see the vicious cycle article.
This article does not recommend brands. The reader chooses based on strain evidence, dose, and formulation. The data above provides the strain identifiers and trial doses needed to evaluate any product against the published evidence.
The gut-vagus-brain pathway may not be the only factor affecting your sleep. Autonomic hyperarousal, metabolic disruptions, inflammatory processes, or circadian misalignment may also be contributing. When multiple causes overlap, identifying which ones are active is a useful next step.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
Can Probiotics Keep You Awake at Night?
Do Probiotics Work for Everyone’s Sleep?
Can You Get Sleep-Supporting Probiotics From Food?
Related Reading
- Autonomic Sleep Disruption: What It Is, How It Fragments Sleep, and How to Recognize It — full overview of autonomic causes including vagal tone, GABA, cortisol, and hyperarousal
- Does Lion’s Mane Affect Your Sleep? Why It Helps Some People and Keeps Others Awake — lion’s mane’s dual mechanism: neurotrophic activity, cholinergic activity, and sleep architecture
- Why Do Cholinergic Supplements Give You Vivid Dreams? — the acetylcholine-REM pathway behind supplement-related vivid dreams
- Which Choline Supplement Is Least Likely to Disrupt Your Sleep? A Form-by-Form Comparison — how different choline forms reach the brain and affect sleep
- How Do You Take Nootropics Without Disrupting Your Sleep? A Neuroscience-Based Approach — timing and stacking guidance for preserving sleep while using nootropics
- Why Can You Not Sleep After COVID? What Happened to Your Vagus Nerve — how post-viral autonomic disruption can affect sleep continuity
- Why Does Your Heart Race at Night After COVID? What the Vagus Nerve Has to Do With It — why post-COVID autonomic instability can show up as nighttime tachycardia
- Can POTS and Dysautonomia Cause Insomnia? Why Your Autonomic Nervous System Will Not Let You Rest — how orthostatic intolerance and autonomic instability can fragment sleep
- Can a Viral Infection Cause Chronic Insomnia? — how viral infections can disrupt autonomic regulation and sleep
- Why Will Your Nervous System Not Let You Sleep? Polyvagal Theory and Insomnia — how polyvagal states map to insomnia, hyperarousal, and unrefreshing sleep
- Why Does Trauma Cause Insomnia? How Your Nervous System Stays on Guard at Night — how trauma can keep sleep shaped by hyperarousal and vigilance
- Why Are You Sleeping 12 Hours and Still Exhausted? The Dorsal Vagal Shutdown Explained — the dorsal vagal pattern behind long sleep that still feels unrefreshing
- How Do Probiotics Reach Your Brain? The Vagotomy Evidence — what vagotomy studies show about gut-brain communication
- Does Poor Sleep Damage Your Gut Microbiome? — the relationship between sleep fragmentation, microbiome disruption, and inflammatory load
- How Long Do Probiotics Take to Improve Sleep? What the Research Shows Week by Week — what probiotic sleep studies suggest about timing across weeks
References
Bravo, J. A., Forsythe, P., Chew, M. V., Escaravage, E., Savignac, H. M., Dinan, T. G., Bienenstock, J., & Cryan, J. F. (2011). Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. Proceedings of the National Academy of Sciences, 108(38), 16050-16055. https://pubmed.ncbi.nlm.nih.gov/21876150/
Kelly, J. R., Allen, A. P., Temko, A., Hutch, W., Kennedy, P. J., Farid, N., Murphy, E., Boylan, G., Bienenstock, J., Cryan, J. F., Clarke, G., & Dinan, T. G. (2017). Lost in translation? The potential psychobiotic Lactobacillus rhamnosus (JB-1) fails to modulate stress or cognitive performance in healthy male subjects. Brain, Behavior, and Immunity, 61, 50-59. https://pubmed.ncbi.nlm.nih.gov/27865949/
Kerksick, C. M., Moon, J. M., Walden, K. E., Hagele, A. M., Allen, L. E., Gaige, C. J., Krieger, J. M., Jager, R., Pane, M., & Mumford, P. (2024). Multi-strain probiotic improves subjective sleep quality with no impact on body composition, hemodynamics, and physical activity. Beneficial Microbes, 15(2), 179-194. https://pubmed.ncbi.nlm.nih.gov/38350465/
Lee, H. J., Hong, J. K., Kim, J. K., Kim, D. H., Jang, S. W., Han, S. W., & Yoon, I. Y. (2021). Effects of Probiotic NVP-1704 on Mental Health and Sleep in Healthy Adults: An 8-Week Randomized, Double-Blind, Placebo-Controlled Trial. Nutrients, 13(8), 2660. https://pubmed.ncbi.nlm.nih.gov/34444820/
Liu, Y., Yu, Y., Lu, S., Tan, K., Jiang, P., Liu, P., & Peng, Q. (2025). Impact of probiotics on sleep quality and mood states in patients with insomnia: a systematic review and meta-analysis. Frontiers in Microbiology, 16, 1596990. https://pubmed.ncbi.nlm.nih.gov/40740336/
Messaoudi, M., Lalonde, R., Violle, N., Javelot, H., Desor, D., Nejdi, A., Bisson, J. F., Rougeot, C., Pichelin, M., Cazaubiel, M., & Cazaubiel, J. M. (2011). Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in rats and human subjects. The British Journal of Nutrition, 105(5), 755-764. https://pubmed.ncbi.nlm.nih.gov/20974015/
Moerkl, S., Narrath, M., Schlotmann, D., Sallmutter, M.-T., Putz, J., Lang, J., Brandstaetter, A., Pilz, R., Lackner, H. K., Goswami, N., Steuber, B., Tatzer, J., Lackner, S., Holasek, S., Painold, A., Jauk, E., Wenninger, J., Horvath, A., Spicher, N., Barth, A., Butler, M. I., & Wagner-Skacel, J. (2025). Multi-species probiotic supplement enhances vagal nerve function – results of a randomized controlled trial in patients with depression and healthy controls. Gut Microbes, 17(1), 2492377. https://pubmed.ncbi.nlm.nih.gov/40298641/
Moloney, G. M., Long-Smith, C. M., Murphy, A., Dorland, D., Hojabri, S. F., Ramirez, L. O., Marin, D. C., Bastiaanssen, T. F. S., Cusack, A. M., Berding, K., Fouhy, F., Allen, A. P., Stanton, C., Clarke, G., Dinan, T. G., & Cryan, J. F. (2021). Improvements in sleep indices during exam stress due to consumption of a Bifidobacterium longum. Brain, Behavior, & Immunity – Health, 10, 100174. https://pubmed.ncbi.nlm.nih.gov/34589719/
Nishida, K., Sawada, D., Kawai, T., Kuwano, Y., Fujiwara, S., & Rokutan, K. (2017). Para-psychobiotic Lactobacillus gasseri CP2305 ameliorates stress-related symptoms and sleep quality. Journal of Applied Microbiology, 123(6), 1561-1570. https://pubmed.ncbi.nlm.nih.gov/28948675/
Sivamaruthi, B. S., Chaiyasut, C., Sisubalan, N., & Kesika, P. (2025). The Impact of Probiotic Supplementation on the Sleep Quality of Humans: A Review of Results of Randomized, Blinded, Controlled Studies. Current Pharmaceutical Design, 31(39), 3128-3138. https://pubmed.ncbi.nlm.nih.gov/40337962/
Yu, B., Wang, K. Y., Wang, N. R., Zhang, L., & Zhang, J. P. (2024). Effect of probiotics and paraprobiotics on patients with sleep disorders and sub-healthy sleep conditions: a meta-analysis of randomized controlled trials. Frontiers in Neurology, 15, 1477533. https://pubmed.ncbi.nlm.nih.gov/39479010/
Written by Kat Fu, M.S., M.S. · Last reviewed: May 2026 · 11 references cited
