People taking nootropics for cognition, focus, or memory face a recurring problem: the same supplements that sharpen daytime performance can degrade nighttime sleep. The standard advice amounts to “take it earlier” — which is correct but incomplete. Different supplement classes disrupt sleep through different neurotransmitter mechanisms, and the timing window varies by pathway. A cholinergic compound like alpha-GPC needs a 4-6 hour clearance window. Modafinil, with its 15-hour half-life, needs 12 or more.
This article classifies nootropics by their sleep-disruption mechanism, provides timing cutoffs per class, and covers evidence-based evening counterbalancing. It does not cover the full autonomic framework. For the broader picture — vagal tone, GABA, cortisol, and hyperarousal — see the autonomic sleep disruption pillar. Cholinergic modulation is one of several autonomic factors controlling sleep architecture. Here, the focus is narrower: how to keep nootropic benefits without paying for them at night.
Why Do Nootropics Disrupt Sleep? Three Pathways
How Does the Cholinergic Pathway Disrupt Sleep?
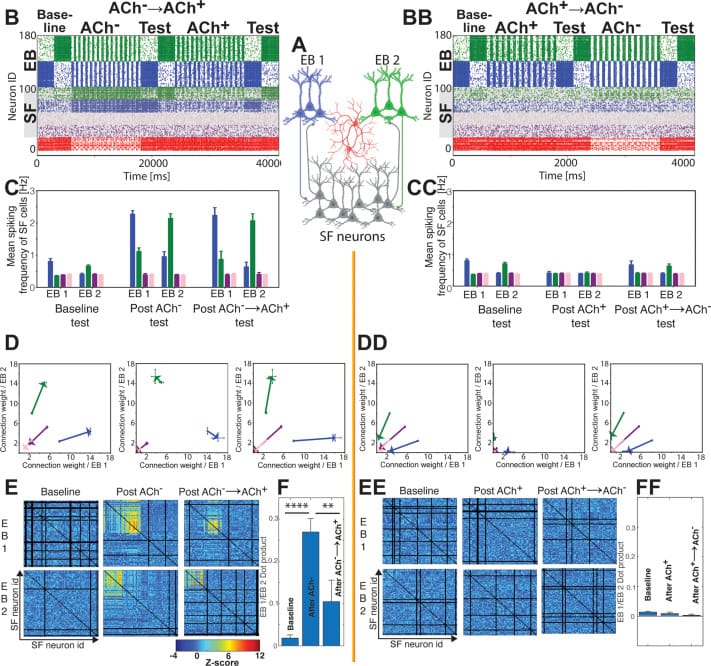
Alpha-GPC, lion’s mane, and huperzine A all raise brain acetylcholine levels. Acetylcholine is the neurotransmitter that drives REM sleep — it activates the brainstem circuits that generate dreaming. In a mouse knockout study, Niwa et al. (2018) showed that muscarinic acetylcholine receptors (Chrm1 and Chrm3) are required for normal REM generation; without them, REM sleep is nearly abolished.
When acetylcholine levels are elevated at bedtime from residual supplement effects, the result is REM intensification: vivid dreams, extended REM periods, and fragmented NREM. NREM — the deep, slow-wave sleep that consolidates declarative memory and supports physical restoration — requires acetylcholine to drop to low levels. A computational modeling study by Satchell et al. (2025) found that low acetylcholine during NREM and high acetylcholine during REM serve sequential, complementary roles in memory consolidation. Their model suggests that disrupting the low-ACh NREM phase with residual supplement effects may impair this consolidation sequence even if total sleep time appears normal.
How Does the Dopaminergic Pathway Disrupt Sleep?
Modafinil, L-tyrosine, and sulbutiamine promote wakefulness through dopaminergic mechanisms. Modafinil has a half-life of approximately 15 hours — an evening dose is never compatible with sleep, and even a late morning dose can persist past bedtime. L-tyrosine has a shorter duration but still extends arousal. The primary effect: difficulty falling asleep and delayed sleep onset.
How Do Glutamatergic Nootropics Interfere With Sleep?
Racetams (piracetam, aniracetam) modulate NMDA glutamate receptors, increasing cortical excitability (Malik & Tlustos, 2022). The effect is difficulty transitioning from wakefulness to N1 sleep — the subjective experience of racing thoughts or an inability to wind down.
Why Is “Take It Earlier” Incomplete Advice?
A blanket 4-hour buffer works for some cholinergic compounds, but modafinil needs a 12-15 hour window. Racetams vary by half-life. Without classifying by mechanism, timing advice is imprecise: what works for alpha-GPC does not work for modafinil, and what works for modafinil is unnecessarily conservative for L-theanine.
Which Nootropics Are Safe to Take in the Afternoon or Evening?
Which Nootropics Are Safe to Take in the Evening?
L-theanine promotes alpha brain wave activity and supports GABAergic tone without sedation. A 2025 meta-analysis of 18 RCTs (N = 897) found that L-theanine reduced subjective sleep onset latency (SMD = 0.15, p = 0.04) and improved daytime functioning (SMD = 0.33, p < 0.001) (Bulman et al., 2025). A 2026 review found 200-450 mg/day to be the effective therapeutic window (Cotter et al., 2026).
Magnesium glycinate supports NREM consolidation through GABA receptor function. It does not interact with cholinergic, dopaminergic, or glutamatergic pathways.
Creatine supports cellular ATP synthesis. It has no direct neurotransmitter activity and no documented sleep-disruption effects.
Bacopa monnieri has anxiolytic properties through GABA modulation. It is unlikely to raise acetylcholine sufficiently to intensify REM at typical supplemental doses, though it has mild cholinergic activity.
Phosphatidylserine supports cortisol regulation. It is not excitatory and does not interfere with sleep staging.
Which Nootropics Must Be Restricted to the Morning?
- Alpha-GPC, lion’s mane, huperzine A — cholinergic: raise acetylcholine, intensify REM, fragment NREM
- Modafinil, L-tyrosine — dopaminergic: extend wakefulness, delay sleep onset
- Piracetam, aniracetam — glutamatergic: increase cortical excitability
- Caffeine — adenosine antagonist: blocks sleep-pressure accumulation
Which Nootropics Have Variable Sleep Effects Depending on the Individual?
CDP-choline can be unpredictable — its effects on brain acetylcholine vary between individuals, and the sleep impact depends on dose and individual metabolism.
Ashwagandha is generally anxiolytic and sleep-supportive, but a subset of individuals finds it mildly stimulating.
Rhodiola has mild dopaminergic activity. For sleep-sensitive individuals, morning dosing is a reasonable precaution.
A 2025 meta-analysis of 28 RCTs covering dietary supplements found that amino acid and micronutrient supplementation improved sleep efficiency, total sleep time, and sleep latency — with tryptophan, vitamin D, omega-3s, zinc, and antioxidants driving the largest effect sizes (Mei et al., 2025).
What Is the Optimal Timing Window for Each Nootropic Class?
When Should You Stop Taking Cholinergic Nootropics?
For a 10-11 PM bedtime, take cholinergic nootropics by noon. Alpha-GPC clears in approximately 4-6 hours. Lion’s mane, which works partly through acetylcholinesterase inhibition, may persist longer. Huperzine A has the longest half-life of the cholinergic group and accumulates with daily use — its effects can extend well beyond a single dose window.
The reason the cutoff matters: a computational model by Satchell et al. (2025) found that low acetylcholine during NREM and high acetylcholine during REM serve complementary, sequential roles in memory consolidation. Residual cholinergic supplement effects that keep acetylcholine elevated during the first NREM cycles may impair this sequence — even if you fall asleep on time and sleep the expected number of hours.
What Is the Cutoff Time for Dopaminergic Nootropics?
Modafinil: before 8 AM. Its approximately 15-hour half-life means a 10 AM dose still has active metabolites at 1 AM. L-tyrosine: before 10 AM. Sulbutiamine has a shorter half-life but should still be restricted to morning.
When Should Racetams Be Taken to Protect Sleep?
Racetams by early afternoon. Noopept has a shorter half-life and is more forgiving, but afternoon dosing is still the conservative approach.
What Is the Cutoff Time for Caffeine?
Caffeine has a 5-7 hour half-life in typical metabolizers, but CYP1A2 polymorphisms can triple this duration. A 2 PM coffee still has approximately 50% of its adenosine-blocking effect at 9 PM in a typical metabolizer. For people who are sleep-sensitive, noon is a reasonable cutoff.
Can You Counterbalance Stimulating Nootropics With Evening Supplements?
How Does Glycine Support Sleep Without Opposing Daytime Nootropics?
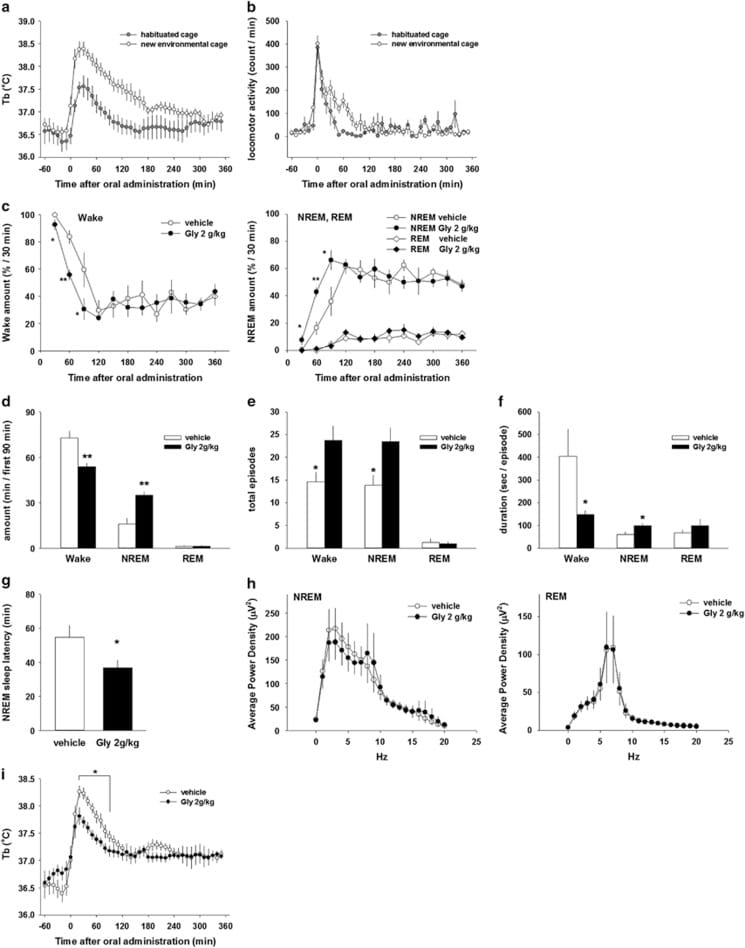
In a rat study, glycine acted on NMDA receptors in the suprachiasmatic nucleus — the brain’s circadian pacemaker — to drive peripheral vasodilation, which lowers core body temperature. This temperature drop is a prerequisite for sleep onset. Kawai et al. (2015) found that NMDA receptor blockade abolished glycine’s sleep-promoting effects, while glycine receptor antagonists had no effect — identifying the glutamatergic NMDA receptor as the molecular target in this animal model. Ablation of the SCN eliminated the response, identifying the circadian control region as the obligate relay. A review by Bannai and Kawai (2012) reported that glycine ingestion before bedtime improved subjective sleep quality in individuals with insomniac tendencies. A separate trial found that glycine reduced next-day fatigue and improved psychomotor vigilance in sleep-restricted volunteers (Bannai et al., 2012b).
Glycine does not oppose cholinergic or dopaminergic pathways. It works through an independent mechanism, making it compatible with all daytime nootropic classes.
How Does L-Theanine Help Sleep Without Causing Sedation?
L-theanine promotes alpha brain wave activity and reduces arousal without sedation. A 2025 meta-analysis of 897 participants found improvements in sleep onset latency and daytime functioning (Bulman et al., 2025). A 2026 review found 200-450 mg/day to be the effective range and noted that L-theanine aids relaxation without causing sedation, making it compatible with daytime cognitive function (Cotter et al., 2026).
Does Magnesium Improve Sleep Quality in People Taking Nootropics?
A 2025 RCT of 155 adults with self-reported poor sleep found that 250 mg/day elemental magnesium as bisglycinate reduced Insomnia Severity Index scores compared to placebo (p = 0.049), with larger effects in participants with lower baseline dietary magnesium intake (Schuster et al., 2025). The bisglycinate form delivers both magnesium and glycine in a single compound.
A 2024 RCT of magnesium L-threonate — a form with higher blood-brain barrier penetration — found that Oura-ring-derived metrics showed improved deep sleep, REM sleep, and readiness scores compared to placebo (Hausenblas et al., 2024).
Which Common Sleep Aids Do Not Work as Counterbalancing Agents?
Melatonin does not address neurotransmitter disruption. It supports circadian timing, but if acetylcholine or dopamine levels are still elevated, melatonin does not resolve the architectural disruption.
Antihistamines (diphenhydramine/Benadryl) suppress REM sleep — they create a new sleep architecture problem rather than solving the existing one. See: Does Benadryl Destroy Your Sleep? How Anticholinergic Drugs Suppress REM.
In What Order Should You Take Evening Counterbalancing Supplements?
Glycine (3g) + magnesium glycinate (200-400 mg elemental): 30-60 minutes before bed. L-theanine (200 mg): 30 minutes before bed. These work through pathways independent of the cholinergic, dopaminergic, and glutamatergic mechanisms the daytime nootropics engage.
Sleep disruption from nootropic supplements may not be the only factor affecting your rest. Autonomic hyperarousal, GABA receptor changes, metabolic disruptions, or inflammatory processes may also be contributing. When multiple causes overlap, identifying which ones are active is a useful next step.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
Does Caffeine Count as a Nootropic for This Approach?
Can You Build Tolerance to Nootropic Sleep Disruption?
Should You Cycle Nootropics to Protect Sleep?
Are Nootropics Worse for Sleep Than Coffee?
Related Reading
- Autonomic Sleep Disruption: What It Is, How It Fragments Sleep, and How to Recognize It — full overview of autonomic causes including vagal tone, GABA, cortisol, and hyperarousal
- Does Lion’s Mane Affect Your Sleep? Why It Helps Some People and Keeps Others Awake — lion’s mane’s dual mechanism: neurotrophic activity, cholinergic activity, and sleep architecture
- Why Do Cholinergic Supplements Give You Vivid Dreams? — the acetylcholine-REM pathway behind supplement-related vivid dreams
- Which Choline Supplement Is Least Likely to Disrupt Your Sleep? A Form-by-Form Comparison — how different choline forms reach the brain and affect sleep
- Why Can You Not Sleep After COVID? What Happened to Your Vagus Nerve — how post-viral autonomic disruption can affect sleep continuity
- Why Does Your Heart Race at Night After COVID? What the Vagus Nerve Has to Do With It — why post-COVID autonomic instability can show up as nighttime tachycardia
- Can POTS and Dysautonomia Cause Insomnia? Why Your Autonomic Nervous System Will Not Let You Rest — how orthostatic intolerance and autonomic instability can fragment sleep
- Can a Viral Infection Cause Chronic Insomnia? — how viral infections can disrupt autonomic regulation and sleep
- Why Will Your Nervous System Not Let You Sleep? Polyvagal Theory and Insomnia — how polyvagal states map to insomnia, hyperarousal, and unrefreshing sleep
- Why Does Trauma Cause Insomnia? How Your Nervous System Stays on Guard at Night — how trauma can keep sleep shaped by hyperarousal and vigilance
- Why Are You Sleeping 12 Hours and Still Exhausted? The Dorsal Vagal Shutdown Explained — the dorsal vagal pattern behind long sleep that still feels unrefreshing
- Which Probiotic Strains Improve Sleep? What the Vagus Nerve Evidence Shows — which probiotic strains have human sleep evidence and how the vagus nerve may be involved
- How Do Probiotics Reach Your Brain? The Vagotomy Evidence — what vagotomy studies show about gut-brain communication
- Does Poor Sleep Damage Your Gut Microbiome? — the relationship between sleep fragmentation, microbiome disruption, and inflammatory load
- How Long Do Probiotics Take to Improve Sleep? What the Research Shows Week by Week — what probiotic sleep studies suggest about timing across weeks
References
- Bannai, M., & Kawai, N. (2012). New therapeutic strategy for amino acid medicine: glycine improves the quality of sleep. Journal of Pharmacological Sciences, 118(2), 145-148. https://pubmed.ncbi.nlm.nih.gov/22293292/
- Bannai, M., Kawai, N., Ono, K., Nakahara, K., & Murakami, N. (2012b). The effects of glycine on subjective daytime performance in partially sleep-restricted healthy volunteers. Frontiers in Neurology, 3, 61. https://pubmed.ncbi.nlm.nih.gov/22529837/
- Bulman, A., D’Cunha, N. M., Marx, W., Turner, M., McKune, A., & Naumovski, N. (2025). The effects of L-theanine consumption on sleep outcomes: A systematic review and meta-analysis. Sleep Medicine Reviews, 81, 102076. https://pubmed.ncbi.nlm.nih.gov/40056718/
- Cooke, J. R., Loredo, J. S., Liu, L., Marler, M., Corey-Bloom, J., Fiorentino, L., Harrison, T., & Ancoli-Israel, S. (2006). Acetylcholinesterase inhibitors and sleep architecture in patients with Alzheimer’s disease. Drugs & Aging, 23(6), 503-511. https://pubmed.ncbi.nlm.nih.gov/16872233/
- Cotter, J., Caddick, C. E., Harper, J. L., & Ebajemito, J. K. (2026). Examining the effect of L-theanine on sleep: A systematic review of dietary supplementation trials. Nutritional Neuroscience, 29(2), 224-238. https://pubmed.ncbi.nlm.nih.gov/41176609/
- Hausenblas, H. A., Lynch, T., Hooper, S., Shrestha, A., Rosendale, D., & Gu, J. (2024). Magnesium-L-threonate improves sleep quality and daytime functioning in adults with self-reported sleep problems: A randomized controlled trial. Sleep Medicine: X, 8, 100121. https://pubmed.ncbi.nlm.nih.gov/39252819/
- Kawai, N., Sakai, N., Okuro, M., Karakawa, S., Tsuneyoshi, Y., Kawasaki, N., Takeda, T., Bannai, M., & Nishino, S. (2015). The sleep-promoting and hypothermic effects of glycine are mediated by NMDA receptors in the suprachiasmatic nucleus. Neuropsychopharmacology, 40(6), 1405-1416. https://pubmed.ncbi.nlm.nih.gov/25533534/
- Li, J., Zhang, J., Wang, Y., Yang, Y., Su, Y., Gu, L., & Chang, C. (2025). L-alpha-glycerylphosphorylcholine (L-alpha-GPC): A comprehensive review of its preparation techniques and versatile biological effects. Journal of Food Science, 90(6), e70338. https://pubmed.ncbi.nlm.nih.gov/40556032/
- Malik, M., & Tlustos, P. (2022). Nootropics as cognitive enhancers: Types, dosage and side effects of smart drugs. Nutrients, 14(16), 3367. https://pubmed.ncbi.nlm.nih.gov/36014874/
- Mei, M., Zhou, Q., Gu, W., Li, F., Yang, R., Lei, H., & Liu, C. (2025). Dietary supplement interventions and sleep quality improvement: A systematic review and meta-analysis. Nutrients, 17(24), 3952. https://pubmed.ncbi.nlm.nih.gov/41470897/
- Niwa, Y., Kanda, G. N., Yamada, R. G., Shi, S., Sunagawa, G. A., Ukai-Tadenuma, M., Fujishima, H., Matsumoto, N., Masumoto, K. H., Nagano, M., Kasukawa, T., Galloway, J., Perrin, D., Shigeyoshi, Y., Ukai, H., Kiyonari, H., Sumiyama, K., & Ueda, H. R. (2018). Muscarinic acetylcholine receptors Chrm1 and Chrm3 are essential for REM sleep. Cell Reports, 24(9), 2231-2247.e7. https://pubmed.ncbi.nlm.nih.gov/30157420/
- Satchell, M., Butel-Fry, E., Noureddine, Z., Simmons, A., Ognjanovski, N., Aton, S. J., & Zochowski, M. R. (2025). Cholinergic modulation of neural networks supports sequential and complementary roles for NREM and REM states in memory consolidation. PLOS Computational Biology, 21(6), e1013097. https://pubmed.ncbi.nlm.nih.gov/40526789/
- Schuster, J., Cycelskij, I., Lopresti, A., & Hahn, A. (2025). Magnesium bisglycinate supplementation in healthy adults reporting poor sleep: A randomized, placebo-controlled trial. Nature and Science of Sleep, 17, 2027-2040. https://pubmed.ncbi.nlm.nih.gov/40918053/
Written by Kat Fu, M.S., M.S. — Last reviewed: May 2026 — 13 references cited
