A cool bedroom helps with sleep. That part is well-understood. What receives less attention is that your body runs a circadian temperature rhythm that gates sleep onset independently of room temperature. When this internal thermoregulatory gate is impaired — which becomes more common after 40 — the room can be cool and the person exhausted, but sleep onset stalls because the body cannot offload heat from its core to its extremities.
This article covers the mechanism behind that gate (the distal-proximal temperature gradient and vasodilation), why it weakens with aging, the warm bath paradox, and how body temperature affects deep sleep throughout the night and at sleep onset. Thermoregulatory disruption is one of several circadian mechanisms that fragment sleep; the Circadian Rhythm Disruption overview on circadian sleep disruption covers the broader picture, including how orexin-driven wakefulness is timed by the circadian clock and how melatonin suppresses orexin to enable sleep onset.
?-
Why Does Your Body Temperature Have to Drop Before You Can Fall Asleep?
Your core body temperature follows a circadian rhythm that peaks in the late afternoon or early evening and reaches its lowest point (the nadir) near 4 am. The declining phase — from evening through early night — is when the thermoregulatory gate opens for sleep. The direction of the temperature change, not the absolute number on the thermometer, is what initiates the process.
The mechanism works in a defined sequence. As melatonin onset begins in the evening, blood vessels in distal skin — hands and feet — dilate. Blood flows to these extremities, and heat radiates outward from the skin surface. Core temperature drops. Sleep initiates.
In a constant routine study, Krauchi and colleagues (1999) used stepwise regression to identify which physiological variable best predicted how quickly participants fell asleep. The distal-to-proximal skin temperature gradient (DPG) — the temperature difference between hands/feet and the torso — was the single best predictor of sleep onset latency. It outperformed core body temperature, heart rate, melatonin onset, and subjective sleepiness ratings (Krauchi et al., 1999). The finding was confirmed in a subsequent detailed analysis using a modified constant-routine protocol with 18 male participants (Krauchi et al., 2000).
This means the rate of heat transfer from your core to your skin surface — not how cold your bedroom is — is the primary physiological variable that determines when you fall asleep. The preoptic area of the hypothalamus contains warm-sensitive neurons that are activated during sleep onset and NREM sleep, and are implicated in both thermoregulation and arousal-state control (Szymusiak, 2018).
?-
Why Are You So Hot at Night When You Were Not During the Day?
A 2025 comparative study measured core body temperature continuously in young and middle-aged men during polysomnography. Younger men showed a sustained nocturnal decline in core temperature, and their sleep included more slow-wave sleep and more REM. Middle-aged men had a blunted temperature decline that began rising earlier in the night, and their sleep was more fragmented with less deep sleep and less REM. The age-related attenuation of the core body temperature decline was associated with poorer sleep continuity across multiple measures (Herberger et al., 2025).
The problem is not limited to aging. A 2025 controlled laboratory study found that individuals with high sleep reactivity — a measure of vulnerability to insomnia — had distal skin temperatures approximately 2 degrees Celsius lower than the low-sleep-reactivity group, proportional to severity. Their peripheral vasodilation was impaired: the hands and feet were not warming enough to dissipate core heat. Reduced distal skin temperature functioned as a physiological marker of insomnia susceptibility, linking impaired peripheral vasodilation to stress-induced sleep disruption (Bigalke et al., 2025).
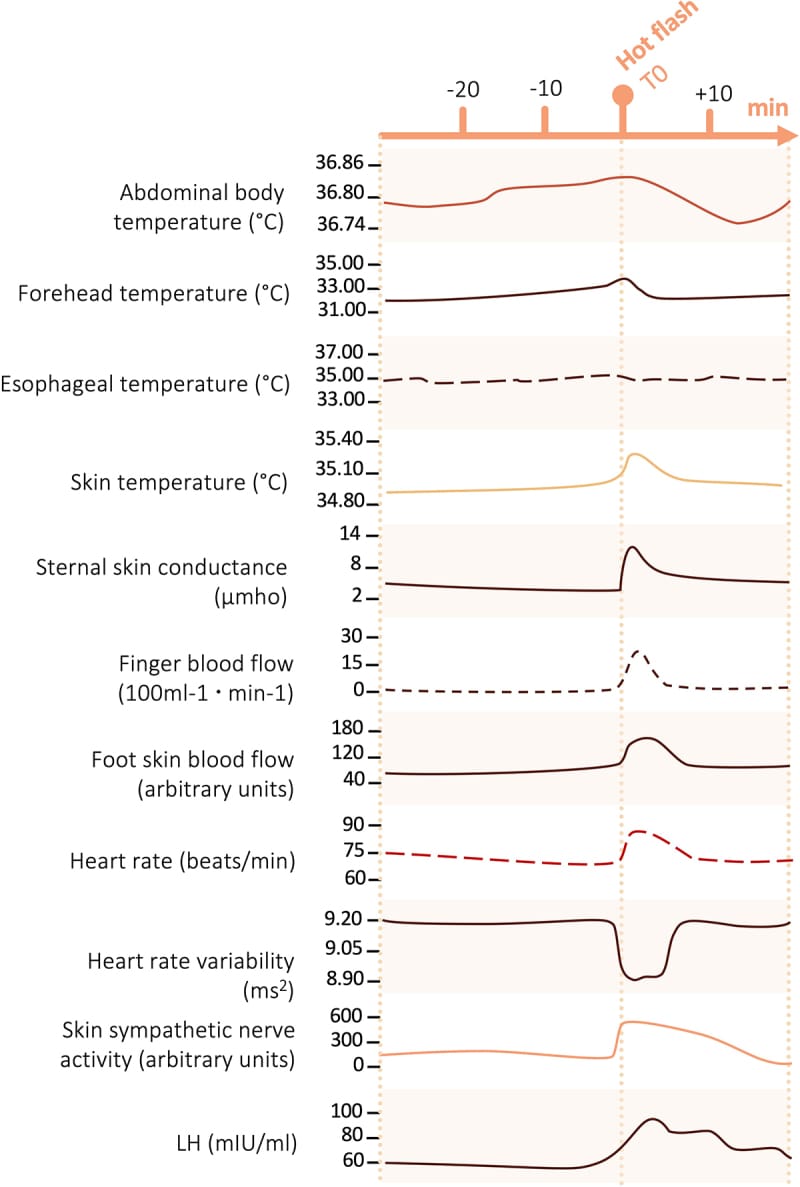
Night sweats are one form of this thermoregulatory impairment. In women, estrogen decline after menopause destabilizes KNDy neurons (kisspeptin/neurokinin B/dynorphin neurons) in the hypothalamic arcuate nucleus. These neurons project to the preoptic thermoregulatory area and, when hyperactive, trigger inappropriate vasodilation and sweating at the wrong circadian phase. The result is a hot flash — the heat-loss machinery firing when it should not be. During REM sleep, the body suspends its ability to sweat or shiver, so nocturnal hot flashes occur preferentially outside of REM and trigger arousals that fragment sleep (Gombert-Labedens et al., 2025).
In men, testosterone decline can affect thermoregulatory efficiency — a pattern that becomes more common after 40 and can compound with the age-related blunting of the core temperature rhythm.
?-
Can a Warm Shower Before Bed Help You Fall Asleep Faster?
The counterintuitive finding — warming the body to cool it down — has quantitative support. Haghayegh and colleagues (2019) conducted a meta-analysis of 17 studies, 13 of which provided quantitative sleep onset data. Water-based passive body heating at 40-42.5 degrees Celsius (approximately 104-108 degrees Fahrenheit), taken 1-2 hours before the target bedtime for at least 10 minutes, significantly shortened sleep onset latency — by an average of approximately 10 minutes (Haghayegh et al., 2019).
Timing matters. Bathing too close to bedtime means core temperature has not had time to drop by the time you get into bed. Bathing too early means the vasodilatory effect has dissipated before the sleep window. The 1-2 hour window before desired sleep time was the range associated with the best outcomes.
The mechanism follows the same sequence that gates sleep onset under normal conditions: warm water causes peripheral vasodilation, blood rushes to the skin surface, heat radiates outward, the distal-to-proximal temperature gradient increases, core temperature drops faster, and the sleep gate opens sooner. The warm water accelerates a process that the body performs on its own — but performs less efficiently with age.
Tai and colleagues (2021) studied 1,094 older adults with a mean age of 72 and found that hot-water bathing 1-3 hours before bed was independently associated with shorter sleep onset latency, accompanied by a higher distal-to-proximal temperature gradient (Tai et al., 2021).
Both showers and baths work — the meta-analysis included studies using showers — so the practical barrier is lower than it may appear. Water temperature of 40-42.5 degrees Celsius, timing of 1-2 hours before bed, and duration of at least 10 minutes are the parameters associated with the best results.
?-
Does Body Temperature Affect Deep Sleep — Not Just Sleep Onset?
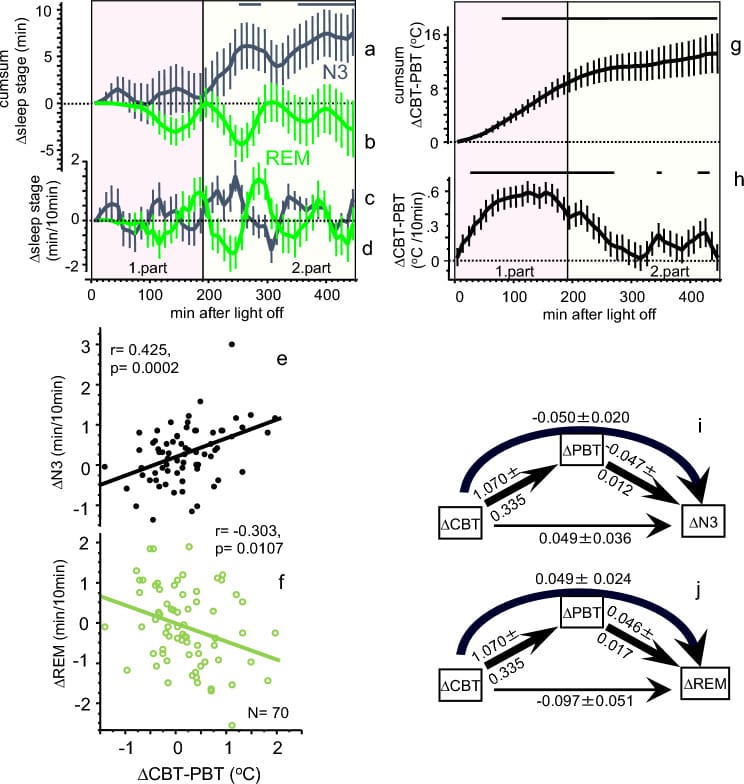
Herberger and colleagues (2024) tested this in 72 participants across varied age, sex, and BMI groups using polysomnography. A high-heat-capacity mattress increased the core-to-skin temperature gradient during sleep. The result: N3 slow-wave sleep increased by approximately 7.5 minutes per night (p = 0.0038), and heart rate decreased by 2.36 beats per minute (p < 0.0001). Both effects were associated with the magnitude of the temperature gradient between core and skin — not with the absolute core body temperature (Herberger et al., 2024).
This extends the gradient principle from sleep onset into sleep maintenance. A cool room helps because it creates a larger gradient between the skin surface and the ambient air, allowing more heat to radiate outward. But the body’s internal vasodilation capacity — its ability to move blood to the skin surface in the first place — has a larger effect on deep sleep than the room thermostat. A person whose peripheral vasodilation is impaired (from aging, stress, or hormonal changes) may sleep in a cool room and still not achieve an adequate core-to-skin gradient for deep sleep.
The preoptic area of the hypothalamus contains warm-sensitive neurons implicated in both thermoregulation and sleep-state control. Their activity promotes and sustains slow-wave sleep (Szymusiak, 2018).
Cooling mattresses, cooling pads, and similar products work through this gradient mechanism — they increase conductive heat loss from the body’s surface, augmenting the core-to-skin gradient that promotes deep sleep.
?-
What Is the Ideal Bedroom Temperature for Sleep?
The 18-20 degrees Celsius range creates a favorable ambient gradient for heat to radiate from the skin surface. But the room temperature is only one side of the equation. The body has to execute the vasodilation — dilating blood vessels in the hands and feet to move heat from the core to the skin — for the gradient to work. A person whose peripheral vasodilation is impaired, whether from aging, chronic stress, or hormonal changes, can lie in a cool room and still have an elevated core temperature at sleep onset (Krauchi et al., 2000).
The DPG mechanism — the rate of heat transfer from distal extremities — has a larger effect on sleep onset than the thermostat. Room temperature creates the gradient opportunity; the body has to execute the vasodilation to use it.
?-
Does Body Temperature Affect Rapid Eye Movement Sleep?
This suspension of thermoregulatory control during REM has a direct consequence for sleep continuity. If core temperature is higher than it should be at a given circadian phase, the body can attempt to correct that during non-REM sleep through sweating and vasodilation. During REM, those mechanisms are offline. The body tolerates whatever temperature it carried into the REM period.
This is also why nocturnal hot flashes and night sweats occur preferentially outside of REM. The KNDy neuron-driven heat-loss response — inappropriate vasodilation and sweating after estrogen decline — requires intact thermoregulatory effectors, which are suppressed during REM. The hot flashes fire during non-REM or during wake periods, often triggering arousals that prevent the transition back into deeper sleep stages (Gombert-Labedens et al., 2025).
?-
Why Do Night Sweats Get Worse With Age?
The KNDy neuron pathway is the best-characterized mechanism. These neurons — which release kisspeptin, neurokinin B, and dynorphin — sit in the arcuate nucleus of the hypothalamus and project to the preoptic thermoregulatory area. Estrogen normally modulates their activity. When estrogen declines through perimenopause and menopause, KNDy neurons become hypertrophic and hyperactive, narrowing the thermoneutral zone — the range of core temperatures the body tolerates without triggering heat-loss or heat-conservation responses. The result: vasodilation and sweating fire at lower thresholds and at inappropriate circadian phases (Gombert-Labedens et al., 2025).
In men, the mechanism is less thoroughly characterized but may involve analogous disruptions. Testosterone decline in middle age can affect thermoregulatory efficiency, and the age-related blunting of the nocturnal core body temperature decline — documented in the Herberger et al. (2025) comparative study of men — compounds the problem.
The circadian sleep disruption pillar covers how these thermoregulatory changes interact with other age-related sleep disruptions, including orexin decline with aging and how cytokines can suppress circadian clock genes.
?-
Temperature regulation and sleep are connected through the circadian clock — but thermoregulatory disruption might compound with hormonal changes, metabolic changes, autonomic imbalance, or inflammatory processes. In adults over 40, multiple causes of sleep disruption often overlap. Identifying which causes might be contributing is a useful next step.
→ Find out which causes might be driving your 3 AM wakeups
?-
Related Reading
- Circadian Rhythm Disruption: How a Misaligned Internal Clock Fragments Sleep, Drives 3AM Wakeups, and Reduces Sleep Depth — the full overview of circadian sleep disruption, including melatonin, cortisol, body temperature, peripheral clocks, and early-morning waking
- Does Your Circadian Clock Control When Insulin Works? Prediabetes, the Dawn Phenomenon, and Sleep — how circadian insulin timing, glucose rhythm, and dawn physiology affect sleep continuity
- Can Fixing Your Gut Fix Your Sleep? How Gut Bacteria Entrain Your Body Clock — how gut bacteria, the vagus nerve, and microbial rhythms interact with sleep timing
- Can Chronic Inflammation Disrupt Your Circadian Clock Genes? — how cytokines and NF-kB signaling suppress central and peripheral clock genes
- Why Are You Still Exhausted After Months on CPAP? — how intermittent hypoxia can suppress clock genes even after breathing normalizes
- Do Beta Blockers Suppress Melatonin? What Blood Pressure Medication Does to Your Body Clock — how beta blockers, melatonin suppression, and medication timing affect circadian sleep
References
Bigalke, J. A., Murvich, A. M., Brothers, R. M., & Carter, J. R. (2025). Distal skin temperature is reduced in individuals with trait vulnerability to stress-related sleep disturbance. American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 329(1), R1-R12. https://pubmed.ncbi.nlm.nih.gov/40392698/
Gombert-Labedens, M., Vesterdorf, K., Fuller, A., Maloney, S. K., & Baker, F. C. (2025). Effects of menopause on temperature regulation. Temperature (Austin), 12(2), 92-132. https://pubmed.ncbi.nlm.nih.gov/40330614/
Haghayegh, S., Khoshnevis, S., Smolensky, M. H., Diller, K. R., & Castriotta, R. J. (2019). Before-bedtime passive body heating by warm shower or bath to improve sleep: A systematic review and meta-analysis. Sleep Medicine Reviews, 46, 124-135. https://pubmed.ncbi.nlm.nih.gov/31102877/
Herberger, S., Penzel, T., Fietze, I., Glos, M., Cicolin, A., Fattori, E., Grimaldi, D., Reid, K., Zee, P., Mason, M., & Krauchi, K. (2024). Enhanced conductive body heat loss during sleep increases slow-wave sleep and calms the heart. Scientific Reports, 14, 4669. https://pubmed.ncbi.nlm.nih.gov/38409133/
Herberger, S., Lederer, K., Cicolin, A., et al. (2025). Effects of nocturnal decline in core body temperature and heart rate on sleep: A comparative study of two age groups. Somnologie, 29, 185-191. https://doi.org/10.1007/s11818-025-00519-1 [Not indexed in PubMed]
Krauchi, K., Cajochen, C., Werth, E., & Wirz-Justice, A. (1999). Warm feet promote the rapid onset of sleep. Nature, 401(6748), 36-37. https://pubmed.ncbi.nlm.nih.gov/10485703/
Krauchi, K., Cajochen, C., Werth, E., & Wirz-Justice, A. (2000). Functional link between distal vasodilation and sleep-onset latency? American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 278(3), R741-R748. https://pubmed.ncbi.nlm.nih.gov/10712296/
Szymusiak, R. (2018). Body temperature and sleep. Handbook of Clinical Neurology, 156, 341-351. https://pubmed.ncbi.nlm.nih.gov/30454599/
Tai, Y., Obayashi, K., Yamagami, Y., Yoshimoto, K., Kurumatani, N., Nishio, K., & Saeki, K. (2021). Hot-water bathing before bedtime and shorter sleep onset latency are accompanied by a higher distal-proximal skin temperature gradient in older adults. Journal of Clinical Sleep Medicine, 17(6), 1257-1266. https://pubmed.ncbi.nlm.nih.gov/33645499/
Written by Kat Fu, M.S., M.S. ? Last reviewed: May 2026 ? 9 references cited
