Research connecting gut health to sleep has expanded over the past five years, but coverage typically conflates two distinct mechanisms. This article focuses on the metabolic pathway: specific gut bacteria regulate blood sugar stability, and when those bacteria are depleted or imbalanced, the downstream effect is nocturnal glycemic instability. A 2022 study of 550 adults found that gut microbiome functional activity independently predicts individual postprandial glycemic variability across more than 30,000 meals — positioning the gut as a primary blood sugar regulator, not just a digestive organ (Tily et al., 2022).
Chronic nocturnal blood sugar instability may accelerate the insulin resistance progression that underlies metabolic syndrome, type 2 diabetes, and cognitive decline. Understanding whether gut dysbiosis is the upstream driver changes the target: dietary fiber and fermented foods — not carbohydrate restriction alone — become relevant tools.
This article covers how specific gut bacteria influence blood sugar, how poor sleep and gut dysbiosis reinforce each other, and what the evidence shows about restoring microbial balance. It does not cover gut-driven inflammatory sleep disruption (gut permeability leading to cytokine-mediated sleep fragmentation — a separate pathway). For the full metabolic picture, see the parent pillar. For the downstream glucose event, see Can a Blood Sugar Drop Wake You Up at 3am?.
Which Gut Bacteria Regulate Blood Sugar — and What Happens When They Are Depleted?
Certain gut bacteria produce short-chain fatty acids — primarily butyrate and propionate — that influence insulin sensitivity. Short-chain fatty acids activate free fatty acid receptors in the gut and stimulate incretin hormone secretion, which modulates insulin release after meals and hepatic glucose output between meals. When the bacteria that produce butyrate and propionate are depleted, this communication chain weakens, and postprandial blood sugar becomes less stable (Withrow et al., 2021).
Arnoriaga-Rodriguez et al. (2023) enrolled 118 participants (60 with obesity, 58 without) and simultaneously measured continuous glucose via a Dexcom G6 monitor for 10 days, sleep architecture via wrist actigraphy, and gut microbiota composition via shotgun metagenomics. Bacteria from the Christensenellaceae family showed positive correlations with REM sleep duration and negative correlations with glucose levels, while Enterobacteriaceae demonstrated the inverse. Glucose variability — measured by standard deviation, coefficient of variation, and interquartile range — was each independently associated with shorter REM sleep duration (beta = -0.350, P < .001). Iron metabolism-related microbial pathways were associated with higher glucose variability and shorter REM, implicating specific metabolic functions in the gut-sleep-glucose relationship.
Chen et al. (2025) took a multi-omics approach in 127 adults with obstructive sleep apnea, integrating serum metabolomics and gut microbiota profiling. Two factors were associated with impaired glucose metabolism in the context of objective daytime sleepiness: dysregulation of serum valine catabolism and dysbiosis of fecal Bacteroides thetaiotaomicron. B. thetaiotaomicron is a polysaccharide fermenter that contributes to short-chain fatty acid production and intestinal barrier function; its dysbiosis may impair the insulin-sensitizing SCFA pathway described above.
An underappreciated distinction exists between compositional dysbiosis — an overall loss of microbial diversity — and functional dysbiosis, a loss of specific metabolite-producing capacity. Romanenko et al. (2025) identified functional metabolite output as more sensitive to circadian and sleep disruption than taxonomic composition alone. Standard 16S sequencing may show a gut community that looks normal by diversity metrics while missing a deficit in SCFA-producing capacity that is already degrading glycemic control.
Does Poor Sleep Cause Gut Dysbiosis — or Does Gut Dysbiosis Cause Poor Sleep?
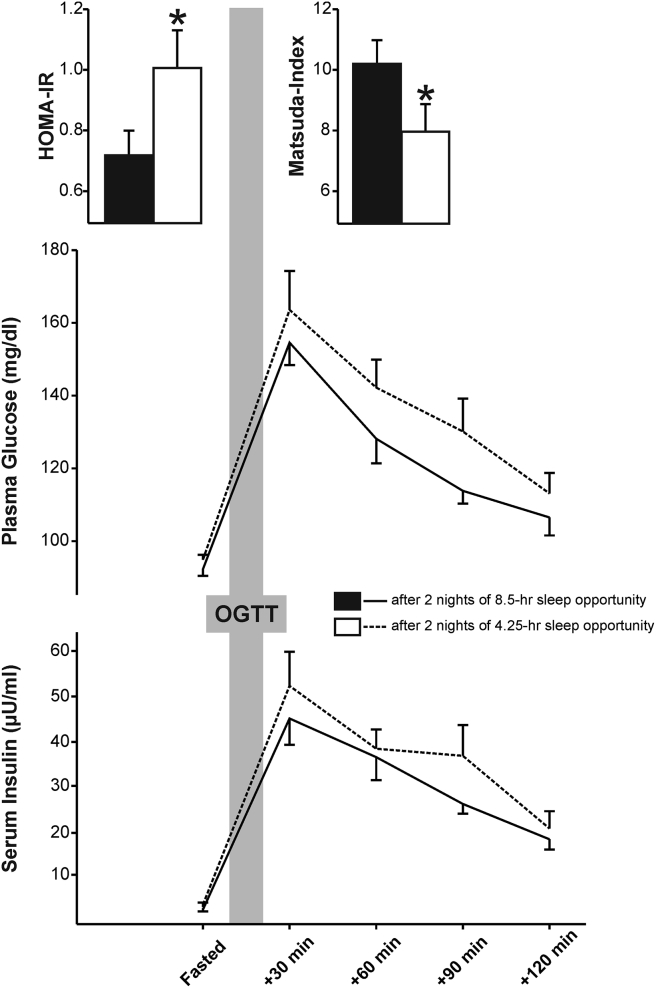
Benedict et al. (2016) conducted a randomized crossover study in nine normal-weight young men comparing two nights of partial sleep deprivation (sleep restricted to 2:45-7:00am) versus normal sleep (10:30pm-7:00am). After partial sleep deprivation, the ratio of Firmicutes to Bacteroidetes increased — a compositional change consistently associated with metabolic impairment in the literature. Coriobacteriaceae and Erysipelotrichaceae showed higher relative abundance, while the phylum Tenericutes was reduced (all P < 0.05). Fasting and postprandial insulin sensitivity both decreased following the two-night sleep restriction compared to normal sleep (P < 0.05). Fecal short-chain fatty acid concentrations did not change. The authors noted that the lack of SCFA change suggests compositional changes in specific taxa, rather than broad metabolite-output changes, may be involved in the acute glucometabolic effect.
Two nights. In normal-weight young men. That is how rapidly sleep restriction alters gut composition and glucose handling.
A 2026 meta-analysis by Supasitdikul et al. pooled 20 studies and quantified the effect of sleep deprivation on the gut microbiome across species. Sleep deprivation reduced alpha diversity (Shannon index SMD = -1.27; 95% CI: -2.20 to -0.34) and increased the Firmicutes-to-Bacteroidetes ratio (SMD = 2.60; 95% CI: 1.61 to 3.59). Human studies showed nonsignificant trends in the same direction — the authors attributed this to small sample sizes and heterogeneous sleep deprivation designs rather than a true null effect.
The other direction of the cycle is equally supported. Holzhausen et al. (2024) enrolled 720 adults (mean age 55 years; 58% female) and found that poor self-reported sleep quality was associated with lower gut microbiome richness and alpha diversity. Greater night-to-night variability in sleep duration — not just short sleep — was associated with reduced microbial richness, suggesting sleep irregularity may be a relevant factor in gut microbial composition independent of sleep duration. Higher wake-after-sleep-onset and lower sleep efficiency were both linked to diminished gut microbiome diversity.

Withrow et al. (2021) suggested that disrupted microbial metabolite output may feed back to affect circadian alignment through gut-brain axis communication, while sleep disruption simultaneously degrades the microbial communities that produce those metabolites. Addressing only one side of the cycle — fixing sleep without attending to gut health, or fixing the gut without improving sleep — leaves the reinforcing loop partially intact.
How Does Gut Dysbiosis Produce the Nocturnal Blood Sugar Swings That Cause 3am Waking?
Gut bacteria do not produce metabolites at a constant rate. In a well-functioning gut, SCFA and secondary bile acid production follows a circadian rhythm, synchronized with the host’s feeding-fasting cycle and hormonal oscillations. Romanenko et al. (2025) reviewed evidence showing that circadian disruption — from rotating work schedules, irregular sleep timing, or chronic sleep deprivation — reduces microbial oscillation rhythmicity and diminishes functional metabolite output. This functional disruption is more sensitive to circadian disturbance than taxonomic composition, meaning standard microbiome sequencing approaches underestimate the metabolic damage.
The body’s overnight glucose regulation depends on a circadian-synchronized pattern of incretin hormone activity and insulin secretion. Microbial metabolite timing partly drives this pattern: SCFAs stimulate incretin hormone secretion from intestinal cells, and secondary bile acids activate receptors including FXR in the liver that modulate hepatic glucose output. When microbial metabolite production is temporally uncoupled from the host’s circadian schedule, overnight glucose management is impaired — insulin secretion is mistimed relative to hepatic glucose output, and glycemic variability increases during the hours when the body is least equipped to compensate.
The scale of the gut’s contribution to glycemic variability is measurable. Tily et al. (2022) analyzed more than 30,000 meals consumed by 550 adults using metatranscriptomic sequencing combined with continuous glucose monitoring. A model incorporating gut microbiome functional activity, anthropometrics, and food macronutrients achieved a Pearson correlation of R = 0.77. Individuals consuming identical meals produced widely different glycemic responses, and the functional state of the gut microbiome explained a large portion of that interpersonal variability. This predictive power may apply overnight as well: two people with the same dinner and the same bedtime may have different overnight glucose trajectories based on their gut microbial functional capacity.
Arnoriaga-Rodriguez et al. (2023) showed the glucose-sleep connection in overnight conditions using 10-day CGM data. Glucose variability metrics — standard deviation, coefficient of variation, interquartile range — each independently correlated with shorter REM sleep duration (beta = -0.350, P < .001). The gut's influence on glycemic stability may contribute to the REM sleep fragmentation associated with glucose variability.
Dos Santos and Galie (2024), in a review of 36 studies, identified shared pathophysiological links between hyperglycemia, insulin resistance, and sleep-disruption-associated gut dysbiosis. The nocturnal glucose swing is both cause and consequence — gut dysbiosis increases glycemic variability, which fragments sleep, which worsens gut dysbiosis, which increases glycemic variability further.
Many people have more than one cause contributing to their sleep disruption. Gut-dysbiosis-driven blood sugar instability may compound with cortisol timing abnormalities, insulin resistance, or circadian misalignment. Identifying which causes might be involved is a useful next step.
Find out which causes might be driving your 3am wakeups →
Does Restoring Gut Bacteria Improve Blood Sugar Stability and Sleep?
Dos Santos and Galie (2024) evaluated three categories of gut-targeted approaches across 36 studies: dietary pattern modification, dietary supplementation (fiber, polyphenols), and probiotic supplementation. All three demonstrated capacity to alter microbiota composition while improving both sleep quality metrics and metabolic markers. Dietary pattern modification — increasing fiber diversity, fermented food consumption, and overall dietary diversity — showed the strongest evidence for modulating both microbial composition and the metabolite output relevant to glycemic stability.
Romanenko et al. (2025) proposed that meal timing optimization aligned with circadian rhythms could realign microbial and host metabolic rhythms and reduce dysbiosis. This proposal is consistent with the circadian uncoupling mechanism: if the gut’s metabolite production has become desynchronized from the host’s circadian schedule, eating within a consistent window that matches the body’s expected feeding period may help re-entrain microbial oscillation patterns. This remains a theoretical framework with supportive preclinical evidence but limited controlled human trial data.
Because gut microbiome functional activity predicts individual postprandial glycemic response at R = 0.77 (Tily et al., 2022), modulating microbial function is a personalized target for blood sugar control. But the specific change needed — which fiber types, what quantity of fermented foods, which probiotic strains — depends on the individual’s microbial deficits. A person depleted in butyrate-producing Christensenellaceae faces a different functional deficit than someone with low Bacteroides thetaiotaomicron.
One mechanism that is often conflated with the metabolic pathway but functions separately: gut bacteria are involved in tryptophan metabolism, and tryptophan is the precursor to serotonin and melatonin. Arnoriaga-Rodriguez et al. (2023) found that iron metabolism-related microbial pathways correlated with higher glucose variability and shorter REM — a finding specific to the metabolic gut-sleep pathway, not the tryptophan-melatonin pathway. The melatonin connection is plausible mechanistically, but quantitative data on gut-derived tryptophan’s contribution to circulating melatonin in humans is not yet established.
What the evidence supports as starting points: dietary diversity (a wider range of plant fibers feeding a wider range of microbial communities), regular inclusion of fermented foods (providing both live microbes and substrates), and consistent meal timing aligned with daytime hours. What it does not yet support: specific probiotic strains, fiber doses, or supplement regimens for improving nocturnal glycemic stability.
Frequently Asked Questions
Can Gut Problems Cause Insomnia?
Benedict et al. (2016) demonstrated that even two nights of partial sleep restriction produced measurable gut compositional changes and insulin sensitivity reduction in normal-weight young men — establishing that the metabolic pathway is rapidly responsive, not a slow-developing condition. The Firmicutes-to-Bacteroidetes change and the postprandial insulin sensitivity decrease appeared within 48 hours, in people with no pre-existing gut or metabolic conditions.
Holzhausen et al. (2024) found in a population of 720 adults that sleep efficiency, wake-after-sleep-onset, and night-to-night sleep variability were each associated with gut microbiome richness — not only in people with identified gut conditions but across a general population. The metabolic pathway is likely relevant when waking correlates with food choices, meal timing, or blood sugar-related sensations (hunger, sweating, racing heart).
What Is the Gut-Brain Axis and How Does It Affect Sleep?
Dos Santos and Galie (2024) identified shared gut-brain axis biomarkers across sleep disturbances and metabolic syndrome components including hyperglycemia, dyslipidemia, and central obesity — indicating these are not parallel problems but a common pathophysiological substrate. The gut-brain axis carries the feedback loop described throughout this article: once dysbiosis impairs glycemic stability and fragments sleep, the resulting poor sleep further degrades microbial diversity (Supasitdikul et al., 2026), reinforcing the cycle from both ends.
Does Leaky Gut Cause Sleep Problems?
This distinction matters practically. Someone focusing on the metabolic pathway (improving dietary fiber diversity, fermented food intake, meal timing) may see no improvement if gut permeability is the primary mechanism — and the reverse is equally true. Withrow et al. (2021) reviewed both pathways and described them as running in parallel rather than as the same mechanism. The indicator for the metabolic pathway: 3am waking that correlates with food choices, timing of the last meal, or post-meal blood sugar patterns. The inflammatory pathway tends to be less time-locked to meals.
How Does the Microbiome Affect Melatonin Production?
Arnoriaga-Rodriguez et al. (2023) found that iron metabolism-related microbial pathways correlated with both higher glucose variability and shorter REM sleep — a finding distinct from the tryptophan-melatonin pathway and specific to the metabolic gut-sleep connection. The melatonin connection is plausible mechanistically but should not be used to justify probiotic supplementation for sleep without strain-specific human trial evidence. The glycemic variability evidence base — not the tryptophan-melatonin hypothesis — is where dietary and microbial approaches have the strongest support.
Related Reading
- Metabolic Sleep Disruption
- Can a Blood Sugar Drop Wake You Up at 3am?
- Why Do You Wake Up Hungry at 3am?
- Does Cortisol Wake You Up at 3am?
- Can a Calorie Deficit Cause Insomnia?
- Adrenal Fatigue and 3am Waking
- Insulin Resistance and Insomnia
- Prediabetes and Sleep Problems
- CGM, Nocturnal Glucose, and Sleep
- Intermittent Fasting, Blood Sugar, and Sleep
- Keto and 3am Waking
- Visceral Fat, Growth Hormone, and Sleep
- The Dawn Phenomenon in Non-Diabetics
- Fatty Liver and Sleep Problems
- Late-Night Eating, Blood Sugar, and Sleep
References
- Arnoriaga-Rodríguez, M., Leal, Y., Mayneris-Perxachs, J., Pérez-Brocal, V., Moya, A., Ricart, W., Fernández-Balsells, M., & Fernández-Real, J. M. (2023). Gut microbiota composition and functionality are associated with REM sleep duration and continuous glucose levels. The Journal of Clinical Endocrinology and Metabolism, 108(11), 2931-2939. https://pubmed.ncbi.nlm.nih.gov/37159524/
- Benedict, C., Vogel, H., Jonas, W., Woting, A., Blaut, M., Schürmann, A., & Cedernaes, J. (2016). Gut microbiota and glucometabolic alterations in response to recurrent partial sleep deprivation in normal-weight young individuals. Molecular Metabolism, 5(12), 1175-1186. https://pubmed.ncbi.nlm.nih.gov/27900260/
- Chen, L., Chen, B., Dai, Y., Sun, Q., Wu, J., Zheng, D., Vgontzas, A. N., Tang, X., & Li, Y. (2025). The association of objective daytime sleepiness with impaired glucose metabolism in patients with obstructive sleep apnea: A multi-omics study. Sleep, 48(2), zsae240. https://pubmed.ncbi.nlm.nih.gov/39549285/
- Dos Santos, A., & Galié, S. (2024). The microbiota-gut-brain axis in metabolic syndrome and sleep disorders: A systematic review. Nutrients, 16(3), 390. https://pubmed.ncbi.nlm.nih.gov/38337675/
- Holzhausen, E. A., Peppard, P. E., Sethi, A. K., Safdar, N., Malecki, K. C., Schultz, A. A., Deblois, C. L., & Hagen, E. W. (2024). Associations of gut microbiome richness and diversity with objective and subjective sleep measures in a population sample. Sleep, 47(3), zsad300. https://pubmed.ncbi.nlm.nih.gov/37988614/
- Romanenko, M., Bartsch, M., Piven, L., Hahn, A., & Müller, M. (2025). Gut microbiota and circadian disruption in humans: Is there a rationale for metabolic disorders? Chronobiology International, 42(9), 1244-1264. https://pubmed.ncbi.nlm.nih.gov/40742095/
- Supasitdikul, T., Mazariegos, J. R. R., Nhat, N. N., Tung, Y. T., Yang, D. F., Lee, L. J., Gunawan, S. P., & Chen, Y. C. (2026). Sleep deprivation alters gut microbiome diversity and taxonomy: A systematic review and meta-analysis of human and rodent studies. Journal of Sleep Research, 35(2), e70125. https://pubmed.ncbi.nlm.nih.gov/40562421/
- Tily, H., Patridge, E., Cai, Y., Gopu, V., Gline, S., Genkin, M., Lindau, H., Sjue, A., Slavov, I., Perlina, A., Klitgord, N., Messier, H., Vuyisich, M., & Banavar, G. (2022). Gut microbiome activity contributes to prediction of individual variation in glycemic response in adults. Diabetes Therapy, 13(1), 89-111. https://pubmed.ncbi.nlm.nih.gov/34799839/
- Withrow, D., Bowers, S. J., Depner, C. M., González, A., Reynolds, A. C., & Wright, K. P., Jr. (2021). Sleep and circadian disruption and the gut microbiome-possible links to dysregulated metabolism. Current Opinion in Endocrine and Metabolic Research, 17, 26-37. https://pubmed.ncbi.nlm.nih.gov/34805616/
Written by Kat Fu, M.S., M.S. — Last reviewed: May 2026 — 9 references cited
