People taking choline supplements for cognition, liver health, or pregnancy frequently report sleep disruption — but the effect varies between supplement forms. The difference comes down to pharmacokinetics: how quickly and efficiently each form delivers choline to the central nervous system.
This article compares alpha-GPC, CDP-choline, choline bitartrate, and phosphatidylcholine through a sleep-impact lens. It does not cover the full range of autonomic factors that affect sleep — for that, see How Does Autonomic Nervous System Imbalance Disrupt Sleep?. Central cholinergic tone is one of several autonomic inputs that shape sleep architecture. What follows is a form-by-form breakdown of how each choline supplement interacts with that input — and which ones are least likely to keep you awake.
How Do Different Choline Supplements Reach Your Brain?
The Bockmann et al. (2022) trial is a rare head-to-head pharmacokinetic comparison of choline supplement forms in humans. Six healthy adult males received single 550 mg choline-equivalent doses of choline chloride, choline bitartrate, alpha-GPC, and egg-derived phosphatidylcholine in a randomized crossover design. Plasma choline area under the curve (AUC) did not differ across the four forms — meaning total absorption into the bloodstream was equivalent regardless of source (Bockmann et al., 2022).
What did differ was the route each form takes after absorption, and how efficiently it reaches the brain.
Alpha-GPC crosses the blood-brain barrier. A 2025 review noted that alpha-GPC can cross the blood-brain barrier, contributing to its use as a choline source for the central nervous system (Li et al., 2025).
CDP-choline (citicoline) is metabolized into cytidine and choline — both of which cross the blood-brain barrier. Once in the brain, these metabolites support phospholipid synthesis and may support acetylcholine production. CDP-choline also elevates noradrenaline and dopamine concentrations in the central nervous system, a characteristic unique among choline forms (Secades & Frontera, 1995).
Choline bitartrate is water-soluble and absorbs quickly into the bloodstream, but does not cross the blood-brain barrier efficiently. It primarily serves peripheral methyl-donor functions — raising betaine levels for methylation without delivering large amounts of choline to the brain.
Phosphatidylcholine (egg-PC) showed the slowest absorption of all four forms, with plasma choline peaking at approximately 3 hours versus approximately 2 hours for water-soluble forms. It has the lowest blood-brain barrier penetration, producing the mildest central cholinergic effect.
One additional finding from Bockmann et al. (2022): choline bitartrate elevated trimethylamine N-oxide (TMAO), a cardiovascular risk marker, while egg-PC did not. Alpha-GPC, like other water-soluble forms, also elevated TMAO. All forms raised betaine levels equivalently, indicating comparable peripheral methylation support regardless of the form chosen.
Which Choline Supplements Are Likely to Disrupt Sleep?
The sleep disruption risk of a choline supplement depends on how much acetylcholine it delivers to the brain — not how much total choline it puts into the bloodstream. Here is how the four forms rank, from highest to lowest risk.
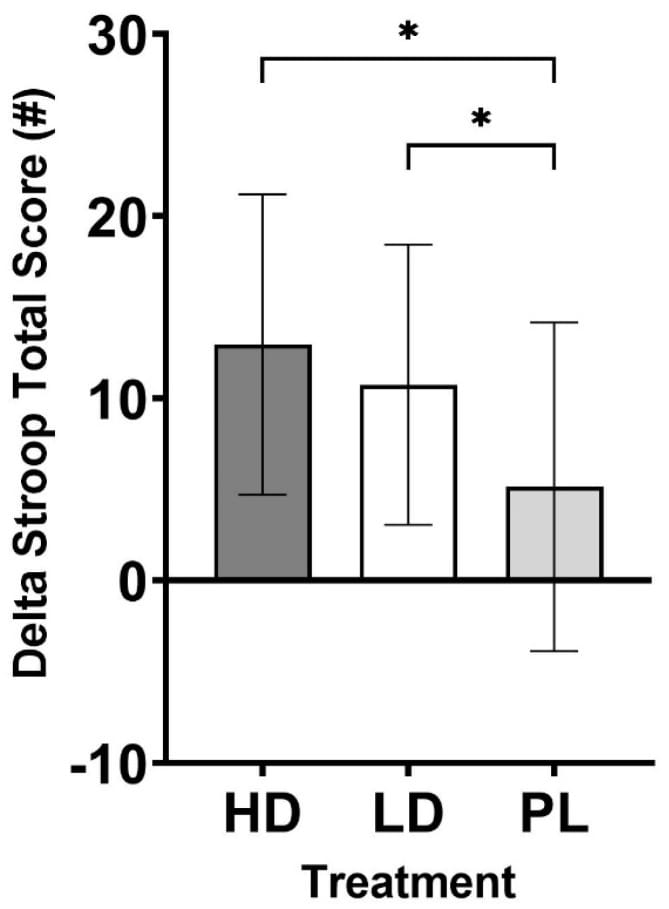
1. Alpha-GPC — Highest risk. Alpha-GPC crosses the blood-brain barrier and delivers choline to the central nervous system. A 2024 double-blind crossover trial in 20 healthy men confirmed that single doses of both 315 mg and 630 mg alpha-GPC improved Stroop test performance (selective attention) at 60 minutes post-ingestion, with effect sizes of d = 0.48-0.61 (Kerksick, 2024). That acute cognitive enhancement is consistent with central cholinergic activity.
Why does brain acetylcholine matter for sleep? Niwa et al. (2018) used CRISPR knockout in mice to show that two muscarinic acetylcholine receptors — Chrm1 and Chrm3 — are essential for REM sleep. Deleting both receptors diminished REM sleep to almost undetectable levels. These are Gq-type receptors, and acetylcholine signaling through these receptors is required for normal REM sleep. Supplements that increase central acetylcholine availability may shift REM sleep regulation through these receptors, potentially affecting sleep quality.
2. CDP-choline — Moderate, variable risk. CDP-choline does cross the blood-brain barrier, but its sleep effects are unpredictable because it modulates three neurotransmitter populations, not just acetylcholine. More detail on this in the next section.
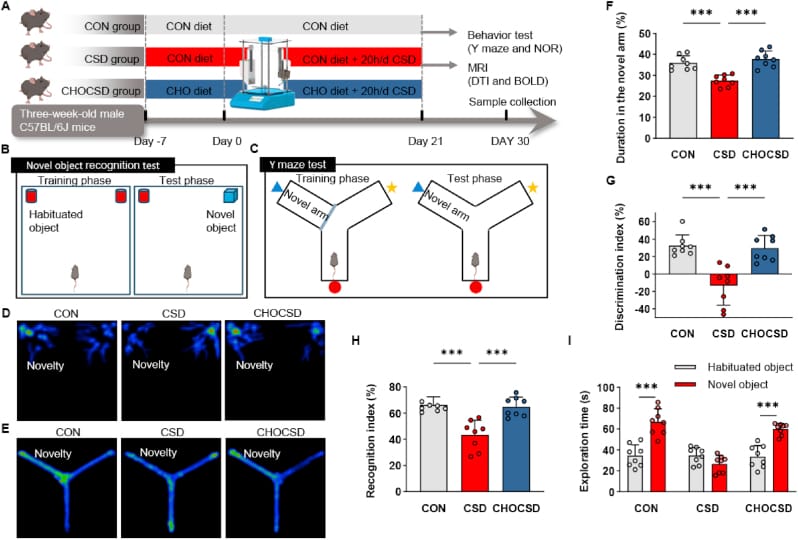
3. Choline bitartrate — Low risk. Poor blood-brain barrier penetration means choline bitartrate raises peripheral choline without delivering large amounts to the central nervous system. A 2025 mouse study found that choline bitartrate protected the blood-brain barrier and reduced neuroinflammation during chronic sleep deprivation — but through the alpha-7 nicotinic acetylcholine receptor (a pathway distinct from the muscarinic receptors linked to REM sleep), not through the muscarinic receptors that drive REM (Huang et al., 2025).
4. Phosphatidylcholine — Lowest risk. The slowest absorption and lowest blood-brain barrier delivery of all four forms. Sleep disruption from phosphatidylcholine at standard supplemental doses is unlikely.
An important implication: dose matters less than form. 550 mg of choline bitartrate may produce less central acetylcholine than 300 mg of alpha-GPC, because the bottleneck is blood-brain barrier crossing, not total choline content.
Does Citicoline Cause Insomnia or Drowsiness?
The Secades & Frontera (1995) review established that CDP-choline elevates noradrenaline and dopamine in the central nervous system beyond its cholinergic effects. This makes CDP-choline pharmacologically distinct from alpha-GPC and choline bitartrate, both of which act primarily through the choline pathway.
The result is unpredictability: three neurotransmitter variables — acetylcholine, dopamine, and noradrenaline — instead of one. Cholinergic activation may affect REM sleep regulation. Dopamine and noradrenaline can drive wakefulness and alertness. But at certain doses or in certain individuals, the net effect appears to promote drowsiness through pathways that are not yet well characterized.
This explains the contradictory user reports. People taking the same dose of CDP-choline report opposite effects — some experience insomnia, others feel sleepy. Individual variation in dopamine receptor density, noradrenaline clearance rates, and baseline cholinergic tone likely determines which effect dominates.
Preclinical evidence adds another dimension. Cakir et al. (2020) found that CDP-choline administered to REM-sleep-deprived rats reversed memory impairment through two pathways: restoring hippocampal CaMKII phosphorylation (a kinase required for memory encoding) and replenishing antioxidant capacity. These dual pathways — cholinergic and non-cholinergic — suggest CDP-choline may support sleep recovery processes even while modulating the same neurotransmitters that can disrupt sleep. This is preclinical data in rats, so the relevance to human supplementation at oral doses remains uncertain.
If CDP-choline disrupts your sleep, two practical options: move the dose to morning (before noon), or switch to choline bitartrate for peripheral benefits — methylation support, liver function, pregnancy requirements — without the central nervous system activation that drives sleep disruption.
What Is the Safest Way to Take Choline Supplements Without Affecting Sleep?
The timing rationale comes from sleep architecture. Acetylcholine needs to be low during the early part of the night, when NREM deep sleep dominates. The Cooke et al. (2006) polysomnographic study in 76 adults with Alzheimer’s disease found that different acetylcholinesterase inhibitors (donepezil, galantamine, rivastigmine) were associated with different NREM stage distributions — suggesting that the pharmacological profile of a cholinergic compound may influence sleep structure in humans. However, the study found no significant differences in REM sleep between treatment groups and was observational, not controlled.
Alpha-GPC timing: The acute cognitive effects were measurable at 1 hour post-ingestion (Kerksick, 2024). The duration beyond this window has not been established in controlled trials. For a 10-11 PM bedtime, taking alpha-GPC by noon provides a conservative timing buffer.
CDP-choline timing: Because CDP-choline has a longer metabolic processing chain (hydrolysis to cytidine + choline, then blood-brain barrier crossing), earlier dosing may be more appropriate. Individual response varies — some people tolerate afternoon dosing, others need morning-only administration.
Form substitution for non-cognitive goals: If the reason you take choline is methylation support (not cognition), switching from alpha-GPC to choline bitartrate maintains the peripheral benefit. Bockmann et al. (2022) showed that all four choline forms tested (choline chloride, choline bitartrate, alpha-GPC, and egg-phosphatidylcholine) raised betaine levels equivalently — meaning methylation support is comparable regardless of which form you choose. The difference is that choline bitartrate does this without the central nervous system activation that disrupts sleep.
Stacking considerations: Combining alpha-GPC with other supplements that raise acetylcholine — lion’s mane, huperzine A, galantamine — amplifies the cholinergic load on the brain. If you use multiple cholinergic supplements, consolidate all of them into a morning window. The muscarinic receptors that are essential for REM sleep (Chrm1 and Chrm3) respond to central acetylcholine. Spreading cholinergic supplements across the day extends the window during which sleep may be disrupted.
For more on how cholinergic supplements interact with dream intensity and REM architecture, see Why Cholinergic Supplements Give You Vivid Dreams (And What That Means for Sleep Quality). For a full timing and stacking framework, see How to Take Nootropics Without Disrupting Your Sleep: A Neuroscience-Based Approach.
Sleep disruption from choline supplements may not be the only factor affecting your rest. Autonomic hyperarousal, GABA changes, metabolic disruptions, or inflammatory processes may also be contributing. When multiple causes overlap, identifying which ones are active is a practical next step.
Find out which causes may be driving your 3am wakeups →
Frequently Asked Questions
Is Alpha-Glycerylphosphorylcholine Better Than Citicoline for Cognition?
Does Phosphatidylcholine Affect Sleep?
Can Choline Bitartrate Cause Vivid Dreams?
Does Choline Supplementation During Pregnancy Affect Sleep?
Related Reading
- Autonomic Sleep Disruption: What It Is, How It Fragments Sleep, and How to Recognize It — full overview of autonomic causes including vagal tone, GABA, cortisol, and hyperarousal
- Does Lion’s Mane Affect Your Sleep? Why It Helps Some People and Keeps Others Awake — lion’s mane’s dual mechanism: neurotrophic activity, cholinergic activity, and sleep architecture
- Why Do Cholinergic Supplements Give You Vivid Dreams? — the acetylcholine-REM pathway behind supplement-related vivid dreams
- How Do You Take Nootropics Without Disrupting Your Sleep? A Neuroscience-Based Approach — timing and stacking guidance for preserving sleep while using nootropics
- Why Can You Not Sleep After COVID? What Happened to Your Vagus Nerve — how post-viral autonomic disruption can affect sleep continuity
- Why Does Your Heart Race at Night After COVID? What the Vagus Nerve Has to Do With It — why post-COVID autonomic instability can show up as nighttime tachycardia
- Can POTS and Dysautonomia Cause Insomnia? Why Your Autonomic Nervous System Will Not Let You Rest — how orthostatic intolerance and autonomic instability can fragment sleep
- Can a Viral Infection Cause Chronic Insomnia? — how viral infections can disrupt autonomic regulation and sleep
- Why Will Your Nervous System Not Let You Sleep? Polyvagal Theory and Insomnia — how polyvagal states map to insomnia, hyperarousal, and unrefreshing sleep
- Why Does Trauma Cause Insomnia? How Your Nervous System Stays on Guard at Night — how trauma can keep sleep shaped by hyperarousal and vigilance
- Why Are You Sleeping 12 Hours and Still Exhausted? The Dorsal Vagal Shutdown Explained — the dorsal vagal pattern behind long sleep that still feels unrefreshing
- Which Probiotic Strains Improve Sleep? What the Vagus Nerve Evidence Shows — which probiotic strains have human sleep evidence and how the vagus nerve may be involved
- How Do Probiotics Reach Your Brain? The Vagotomy Evidence — what vagotomy studies show about gut-brain communication
- Does Poor Sleep Damage Your Gut Microbiome? — the relationship between sleep fragmentation, microbiome disruption, and inflammatory load
- How Long Do Probiotics Take to Improve Sleep? What the Research Shows Week by Week — what probiotic sleep studies suggest about timing across weeks
References
- Bockmann, K. A., Franz, A. R., Minarski, M., Shunova, A., Maiwald, C. A., Schwarz, J., Gross, M., Poets, C. F., & Bernhard, W. (2022). Differential metabolism of choline supplements in adult volunteers. European Journal of Nutrition, 61(1), 219-230. https://pubmed.ncbi.nlm.nih.gov/34287673/
- Cakir, A., Ocalan, B., Koc, C., Suyen, G. G., Cansev, M., & Kahveci, N. (2020). Effects of CDP-choline administration on learning and memory in REM sleep-deprived rats. Physiology & Behavior, 213, 112703. https://pubmed.ncbi.nlm.nih.gov/31654682/
- Cooke, J. R., Loredo, J. S., Liu, L., Marler, M., Corey-Bloom, J., Fiorentino, L., Harrison, T., & Ancoli-Israel, S. (2006). Acetylcholinesterase inhibitors and sleep architecture in patients with Alzheimer’s disease. Drugs & Aging, 23(6), 503-511. https://pubmed.ncbi.nlm.nih.gov/16872233/
- Huang, S. Y., Yang, Z. J., Cheng, J., Li, H. Y., Chen, S., Huang, Z. H., Chen, J. D., Xiong, R. G., Yang, M. T., Wang, C., Li, M. C., Song, S., Huang, W. G., Wang, D. L., Li, H. B., & Lan, Q. Y. (2025). Choline alleviates cognitive impairment in sleep-deprived young mice via reducing neuroinflammation and altering phospholipidomic profile. Redox Biology, 81, 103578. https://pubmed.ncbi.nlm.nih.gov/40056720/
- Kerksick, C. M. (2024). Acute alpha-glycerylphosphorylcholine supplementation enhances cognitive performance in healthy men. Nutrients, 16(23), 4240. https://pubmed.ncbi.nlm.nih.gov/39683633/
- Li, J., Zhang, J., Wang, Y., Yang, Y., Su, Y., Gu, L., & Chang, C. (2025). L-alpha-glycerylphosphorylcholine (L-alpha-GPC): A comprehensive review of its preparation techniques and versatile biological effects. Journal of Food Science, 90(6), e70338. https://pubmed.ncbi.nlm.nih.gov/40556032/
- Niwa, Y., Kanda, G. N., Yamada, R. G., Shi, S., Sunagawa, G. A., Ukai-Tadenuma, M., Fujishima, H., Matsumoto, N., Masumoto, K. H., Nagano, M., Kasukawa, T., Galloway, J., Perrin, D., Shigeyoshi, Y., Ukai, H., Kiyonari, H., Sumiyama, K., & Ueda, H. R. (2018). Muscarinic acetylcholine receptors Chrm1 and Chrm3 are essential for REM sleep. Cell Reports, 24(9), 2231-2247.e7. https://pubmed.ncbi.nlm.nih.gov/30157420/
- Secades, J. J., & Frontera, G. (1995). CDP-choline: Pharmacological and clinical review. Methods and Findings in Experimental and Clinical Pharmacology, 17(Suppl B), 1-54. https://pubmed.ncbi.nlm.nih.gov/8709678/
Written by Kat Fu, M.S., M.S. · Last reviewed: May 2026 · 8 references cited
