The “wired but tired” pattern is one of the most commonly described sleep complaints among GLP-1 drug users, with hundreds of self-reports on Reddit alone. Most online content lists possible causes without explaining the underlying mechanism.
This article explains the specific neuroscience — how GLP-1 receptor agonists reach the brain and activate wakefulness neurons — and why this creates a simultaneous state of fatigue and insomnia. It does not cover all GLP-1 sleep effects; for the full overview, see the parent article linked below.
GLP-1 drugs can disrupt sleep through several distinct pathways. This article covers the orexin-arousal mechanism. Other articles in this series cover blood sugar crashes, vivid dreams, and appetite-related sleep disruption.
Does Semaglutide Activate the Brain’s Wakefulness Switch
Orexin neurons (also called hypocretin neurons) are a small cluster of cells in the lateral hypothalamus that function as metabolic sentinels. They link the body’s energy state to arousal — when energy is low, orexin neurons fire to keep the brain alert so the organism searches for food. When energy is abundant, orexin firing decreases and sleep becomes easier.
In 2004, Acuna-Goycolea and van den Pol demonstrated through electrophysiology experiments in rat brain slices that GLP-1 receptor agonists depolarize orexin neurons through sodium-dependent, G-protein-mediated nonselective cationic channels. The GLP-1 agonist exendin-4 increased both the firing rate and the excitatory synaptic drive onto orexin neurons. The response was dose-dependent and fully blocked by the GLP-1 receptor antagonist exendin 9-39, confirming receptor specificity. The same study tested melanin-concentrating hormone neurons — the sleep-promoting population located in the same brain region — and found no detectable response to GLP-1 (Acuna-Goycolea & van den Pol, 2004).
Based on these rodent findings, GLP-1 drugs appear to activate the wakefulness side of the lateral hypothalamus without simultaneously engaging the sleep side.
The evolutionary logic for this circuit was established by Yamanaka et al. (2003), who showed in mice that orexin neurons are directly inhibited by glucose and leptin (signals of energy abundance) and excited by ghrelin (a hunger signal). Orexin-deficient mice failed to increase wakefulness during fasting — confirming that orexin neurons are required for the arousal response to negative energy balance. GLP-1 is part of this same metabolic signaling network, meaning therapeutic GLP-1 receptor agonists engage a circuit designed to regulate wakefulness based on nutrient status.
The question of whether semaglutide actually reaches orexin-relevant brain regions in therapeutic doses was addressed by Gabery et al. (2020). Using fluorescently labeled semaglutide in rodents, the researchers showed that semaglutide enters the brain through circumventricular organs — specialized brain regions without a blood-brain barrier — and activates a relay from the brainstem through the lateral parabrachial nucleus to the hypothalamus. While the lateral hypothalamus was not among the regions showing direct c-Fos activation from semaglutide in this study, GLP-1 receptors are expressed there, and the hypothalamic relay provides a plausible route for indirect activation of orexin neurons.
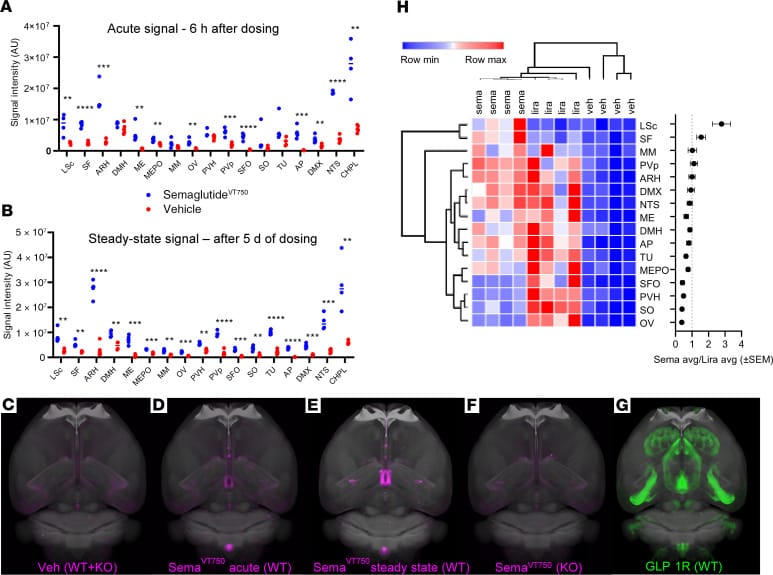
A 2025 review by Hankir and Lutz described the distributed neural pathways through which GLP-1 receptor agonists act, identifying the zona incerta — a brain region implicated in functions ranging from sleep to predator avoidance — as part of the GLP-1 receptor agonist network (Hankir & Lutz, 2025). Because the zona incerta is anatomically connected to hypothalamic arousal regions, this suggests another potential route through which GLP-1 drugs may influence wakefulness signaling, though direct evidence for this specific pathway remains limited.
Why Do You Feel Wired After Your Ozempic Shot
Semaglutide’s pharmacokinetic profile produces maximum plasma concentration (Cmax) approximately 1-3 days after subcutaneous injection. Because the drug accesses the brain through circumventricular organs rather than crossing the blood-brain barrier directly (Gabery et al., 2020), peak brain exposure follows peak plasma levels with a slight delay. The highest orexin neuron activation is therefore predicted to occur roughly 24-72 hours post-injection — the exact window when users most commonly report the wired feeling.
A 2024 study in Nature Neuroscience revealed how orexin neurons respond to the type of metabolic signals that GLP-1 drugs alter. Viskaitis et al. (2024) used two-photon imaging to record from 913 individual orexin neurons in freely behaving mice and found that approximately 98% of orexin neurons tracked blood glucose in a derivative fashion — responding to the rate of glucose change rather than the absolute glucose level. Although the study did not investigate GLP-1 drugs directly, the finding is relevant because GLP-1 is released postprandially in direct response to glucose dynamics, and semaglutide mimics this signal continuously. This suggests the drug provides a sustained input to a system designed to respond to rapid metabolic shifts.
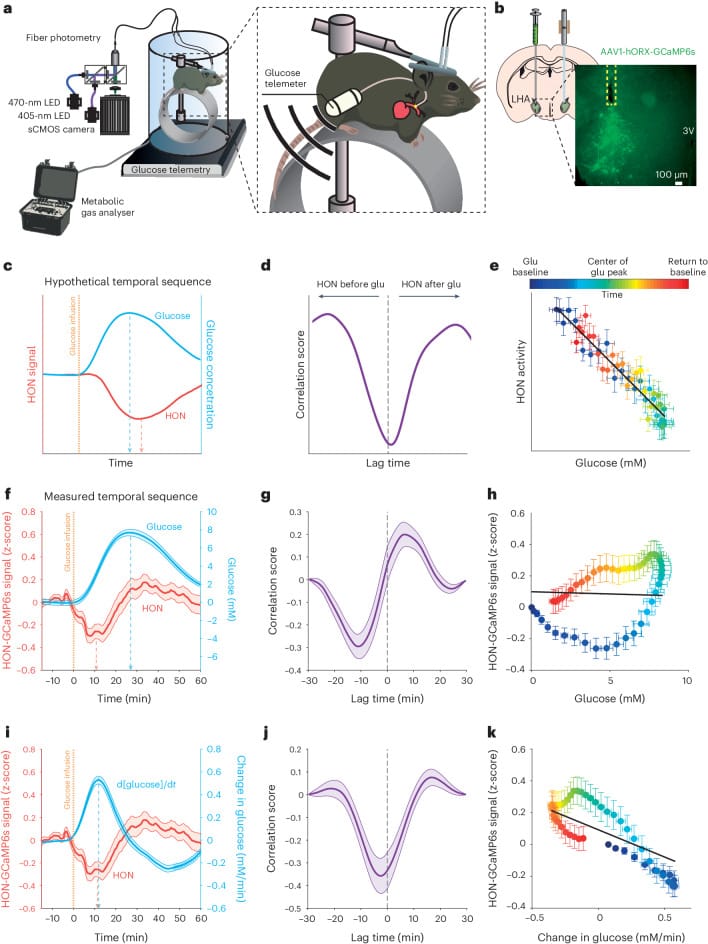
The wired feeling is not unique to semaglutide (Ozempic, Wegovy). Because tirzepatide’s GLP-1 component binds the same receptor, Mounjaro and Zepbound activate the same orexin pathway. Users of both drug classes describe the same pattern: physical exhaustion paired with an inability to fall asleep.
Clinical data supports the arousal side of this equation. Gomez-Peralta et al. (2015) found that liraglutide — another GLP-1 receptor agonist — significantly reduced Epworth Sleepiness Scale scores in obese adults with type 2 diabetes. While the study did not investigate the specific mechanism behind this effect, reduced daytime sleepiness reflects increased wakefulness drive, and the same increased wakefulness that reduces daytime drowsiness could produce unwanted alertness at night.
Why Are You Exhausted During the Day When Ozempic Is Activating Your Brain
Multiple systems contribute to the paradox. Orexin neuron activation, driven by semaglutide binding GLP-1 receptors, promotes cortical arousal. Caloric deficit, driven by semaglutide’s appetite suppression, depletes peripheral energy stores — your muscles, liver glycogen, and metabolic output are all reduced. Adding complexity, orexin neurons are also activated by low energy states (Yamanaka et al., 2003), meaning the caloric deficit itself may further drive the very wakefulness signal that prevents sleep. The “wired but tired” sensation persists because peripheral fatigue and central arousal are driven by converging inputs that reinforce rather than cancel each other.
Semaglutide-driven wakefulness operates through the lateral hypothalamic orexin circuit described above, where GLP-1 receptor activation selectively excites orexin neurons without engaging the adjacent sleep-promoting melanin-concentrating hormone neurons (Acuna-Goycolea & van den Pol, 2004). The fatigue operates through peripheral energy signaling — reduced caloric intake lowers glucose availability, depletes glycogen stores, and decreases the substrates needed for muscle repair and thermoregulation.
The caloric deficit is substantial. Clinical trials in the STEP program documented approximately 15% body weight loss with semaglutide 2.4 mg in non-diabetic populations (STEP 1: -14.9%), reflecting sustained daily caloric deficits maintained over months. Users commonly report eating 500-1,000 fewer calories per day, which produces the same type of physical exhaustion seen in any sustained caloric restriction.
Nausea — reported by approximately 44% of users in STEP clinical trials — compounds the fatigue by further reducing nutrient absorption and causing dehydration. Overall gastrointestinal side effects were reported by approximately 74% of semaglutide users.
The paradox is unlikely to self-resolve at a given dose. As long as semaglutide is present in the brain at concentrations sufficient to activate GLP-1 receptors on orexin neurons (Gabery et al., 2020), the wakefulness signal persists. And as long as caloric intake remains suppressed, the fatigue persists. The two states coexist because the arousal inputs converge and reinforce rather than oppose each other.
Can Ozempic Trigger Nighttime Anxiety or Restlessness
The distinction between pharmacological arousal and psychiatric anxiety matters because the mechanism and treatment differ. Orexin-driven arousal produces many of the same subjective sensations as anxiety — elevated heart rate, restlessness, an inability to quiet the mind — but the cause is direct receptor activation in the lateral hypothalamus rather than a mood disorder.
Pharmacovigilance data and controlled trial data tell different stories about anxiety on GLP-1 drugs. In the EudraVigilance database, anxiety accounted for 38.7% of psychiatric adverse event reports for GLP-1 receptor agonists (Tobaiqy & Elkout, 2024). But in a post-hoc psychiatric safety analysis of the STEP 1, 2, 3, and 5 trials, psychiatric disorder adverse events were generally balanced between semaglutide and placebo groups, with no signal for increased anxiety (Wadden et al., 2024).
The discrepancy likely reflects measurement differences. Controlled trials capture diagnosed psychiatric disorders assessed by clinicians at scheduled visits. Real-world pharmacovigilance reports capture the subjective experience of nighttime restlessness and unease — symptoms consistent with subclinical orexin-driven hyperarousal that would not meet diagnostic criteria for an anxiety disorder.
Orexin neuron activation drives sympathetic nervous system output, increasing heart rate and alertness. The zona incerta — identified by Hankir and Lutz (2025) as part of the GLP-1 receptor agonist neural network, and implicated in functions ranging from sleep to predator avoidance — may represent another route through which GLP-1 drugs influence arousal, though direct evidence linking this region to GLP-1-driven wakefulness effects remains limited.
Orexin-driven wakefulness is one of several mechanisms through which metabolic changes can disrupt sleep. GLP-1 drugs also affect blood sugar stability, appetite-related neurotransmitter production, and circadian timing — each of which might compound the arousal effect. Sleep disruption from metabolic causes often overlaps with hormonal, circadian, or autonomic factors.
Find out which causes might be driving your 3am wakeups →
Does This Happen With All Glucagon-Like Peptide-1 Drugs or Just Ozempic
The orexin activation mechanism is class-wide because every GLP-1 receptor agonist binds the same receptor on orexin neurons in the lateral hypothalamus. Tirzepatide’s additional GIP receptor agonism may produce different intensity of arousal effects, but the GLP-1 component activates the same wakefulness pathway. In the SURMOUNT-OSA trials, tirzepatide reduced the apnea-hypopnea index by up to 29.3 events per hour compared to 5.3 with placebo — though these improvements in obstructive sleep apnea likely reflect structural changes from weight loss rather than direct effects on sleep-related neural circuitry (Malhotra et al., 2024).
Does the Wired Feeling Go Away After Your Body Adjusts
The standard Wegovy titration schedule moves from 0.25 mg to 0.5 mg to 1.0 mg to 1.7 mg to 2.4 mg over several months (Ozempic follows a similar schedule up to 2.0 mg). Because higher doses produce higher peak plasma concentrations and greater brain exposure through circumventricular organs (Gabery et al., 2020), each dose increase delivers a stronger activation signal to orexin neurons. Users frequently describe the wired feeling receding at a given dose, only to return when the dose is escalated. Some users report persistent effects throughout treatment.
Could Orexin-Blocking Sleep Medications Help With Ozempic Insomnia
The mechanistic logic is straightforward: if GLP-1 receptor agonists activate orexin neurons through GLP-1 receptors on those neurons (Acuna-Goycolea & van den Pol, 2004), then orexin receptor antagonists block the downstream output of those same neurons. Whether this translates to clinical benefit for GLP-1 users with insomnia has not been tested in any published trial. Dual orexin receptor antagonists (suvorexant, lemborexant) block both orexin-1 and orexin-2 receptors, which would suppress the wakefulness signal regardless of what activated the orexin neurons upstream. Any use of these medications requires evaluation by a prescribing physician who can assess the full clinical picture.
Is the Wired-But-Tired Feeling Worse at Higher Ozempic Doses
The dose-response relationship is pharmacokinetically predictable. Higher semaglutide doses produce proportionally higher plasma concentrations and greater brain exposure (Gabery et al., 2020). Because GLP-1-mediated depolarization of orexin neurons is dose-dependent — higher agonist concentrations produce greater firing rate increases — each dose increase delivers a stronger arousal signal.
Does Taking Ozempic in the Morning Instead of at Night Help With Sleep
The pharmacokinetic rationale is sound but unproven. Semaglutide has a long half-life (approximately 7 days), meaning the drug is present at some concentration throughout the entire dosing interval regardless of injection timing. Morning injection shifts the highest concentration window (Cmax at 1-3 days) toward daytime, but orexin neuron activation occurs at concentrations well below peak. Whether the timing shift produces a meaningful reduction in nighttime arousal depends on the dose-response threshold for orexin activation — a threshold that has not been characterized in human clinical studies.
Related Reading
- Metabolic Sleep Disruption — The full metabolic sleep framework covering glucose regulation, insulin resistance, mitochondrial decline, NAD+ loss, and fat metabolism
- Does Ozempic Cause Insomnia What GLP-1 Drugs Do to Your Sleep — The broad overview of GLP-1 sleep side effects and mechanisms
- Why Does Ozempic Wake You Up at 3am — How lower overnight fuel availability and counter-regulatory hormones can contribute to 3am waking
- Does Ozempic Give You Vivid Dreams — How GLP-1 drugs may affect dream intensity through arousal and neuropsychiatric pathways
- Does Eating Too Little on Ozempic Cause Insomnia — How appetite suppression can affect tryptophan, serotonin, melatonin, and overnight glucose stability
- Does Your Ozempic Injection Day Disrupt Your Sleep The 24-48 Hour Pattern — Why sleep disruption can follow a weekly pattern tied to injection timing and peak drug exposure
- Does Your Semaglutide Dose Increase Restart Your Insomnia Why Each Titration Can Disrupt Sleep Again — Why each titration step can restart sleep disruption before adaptation catches up
- Can You Take Melatonin, Magnesium, or Sleep Aids While on Ozempic — How melatonin, magnesium, DORAs, and other sleep aids intersect with GLP-1 physiology
- Does Ozempic Give You Anxiety at Night Why GLP-1 Drugs May Contribute to Nighttime Panic — How orexin activation, HPA-axis signaling, and glucose instability may contribute to nighttime anxiety
- Do GLP-1 Drugs Disrupt Your Body Clock Ozempic, Circadian Rhythms, and Melatonin — How GLP-1 secretion rhythms, food timing, peripheral clocks, and melatonin intersect
- Ozempic Night Sweats: How GLP-1 Drugs May Affect Temperature at Night — How GLP-1 drugs may affect nighttime sweating through autonomic tone and thermoregulation
- Ozempic Nausea and Sleep: How Stomach Side Effects Keep You Awake at Night — How delayed gastric emptying, reflux, and nausea can fragment sleep
- Will Your Sleep Go Back to Normal When You Stop Ozempic — What is known and not known about sleep after semaglutide discontinuation
- Does Ozempic Muscle Loss Affect Your Sleep Sarcopenia, Temperature, and Deep Sleep — How lean-mass loss, thermoregulation, and deep sleep can interact during GLP-1 weight loss
- Could Ozempic Contribute to Restless Legs at Night Iron, B12, and the Dopamine Connection — How iron, B12, dopamine, and rapid weight loss may intersect with restless legs at night
- Does Compounded Semaglutide Affect Sleep Differently Than Brand-Name Ozempic — How dose variability, formulation differences, and adverse-event tracking can affect sleep side effects
- Ozempic and Sleep After 40: Why GLP-1 Side Effects Can Feel Different as You Age — Why GLP-1 sleep effects can land differently after 40 because of muscle, hormones, and glucose regulation
References
- Acuna-Goycolea, C., & van den Pol, A. N. (2004). Glucagon-like peptide 1 excites hypocretin/orexin neurons by direct and indirect mechanisms: Implications for viscera-mediated arousal. The Journal of Neuroscience, 24(37), 8141-8152. https://pubmed.ncbi.nlm.nih.gov/15371515/
- Gabery, S., Salinas, C. G., Paulsen, S. J., Ahnfelt-Rønne, J., Alanentalo, T., Baquero, A. F., Buckley, S. T., Farkas, E., Fekete, C., Frederiksen, K. S., Helms, H. C. C., Jeppesen, J. F., John, L. M., Pyke, C., Nøhr, J., Lu, T. T., Polex-Wolf, J., Prevot, V., Raun, K., … Hogendorf, W. F. J. (2020). Semaglutide lowers body weight in rodents via distributed neural pathways. JCI Insight, 5(6), e133429. https://pubmed.ncbi.nlm.nih.gov/32213703/
- Gomez-Peralta, F., Abreu, C., Castro, J. C., Alcarria, E., Cruz-Bravo, M., Garcia-Llorente, M. J., Albornos, C., Moreno, C., Cepeda, M., & Almodóvar, F. (2015). An association between liraglutide treatment and reduction in excessive daytime sleepiness in obese subjects with type 2 diabetes. BMC Endocrine Disorders, 15, 78. https://pubmed.ncbi.nlm.nih.gov/26637348/
- Hankir, M. K., & Lutz, T. A. (2025). Novel neural pathways targeted by GLP-1R agonists and bariatric surgery. Pflugers Archiv: European Journal of Physiology, 477(2), 171-185. https://pubmed.ncbi.nlm.nih.gov/39644359/
- Malhotra, A., Grunstein, R. R., Fietze, I., Weaver, T. E., Redline, S., Azarbarzin, A., Sands, S. A., Schwab, R. J., Dunn, J. P., Chakladar, S., Bunck, M. C., Bednarik, J., & SURMOUNT-OSA Investigators. (2024). Tirzepatide for the treatment of obstructive sleep apnea and obesity. The New England Journal of Medicine, 391(13), 1193-1205. https://pubmed.ncbi.nlm.nih.gov/38912654/
- Tobaiqy, M., & Elkout, H. (2024). Psychiatric adverse events associated with semaglutide, liraglutide and tirzepatide: A pharmacovigilance analysis of individual case safety reports submitted to the EudraVigilance database. International Journal of Clinical Pharmacy, 46(2), 488-495. https://pubmed.ncbi.nlm.nih.gov/38265519/
- Viskaitis, P., Tesmer, A. L., Liu, Z., Karnani, M. M., Arnold, M., Donegan, D., Bracey, E., Grujic, N., Patriarchi, T., Peleg-Raibstein, D., & Burdakov, D. (2024). Orexin neurons track temporal features of blood glucose in behaving mice. Nature Neuroscience, 27(7), 1299-1308. https://pubmed.ncbi.nlm.nih.gov/38773350/
- Wadden, T. A., Brown, G. K., Egebjerg, C., Frenkel, O., Goldman, B., Kushner, R. F., McGowan, B., Overvad, M., & Fink-Jensen, A. (2024). Psychiatric safety of semaglutide for weight management in people without known major psychopathology: Post hoc analysis of the STEP 1, 2, 3, and 5 trials. JAMA Internal Medicine, 184(11), 1290-1300. https://pubmed.ncbi.nlm.nih.gov/39226070/
- Yamanaka, A., Beuckmann, C. T., Willie, J. T., Hara, J., Tsujino, N., Mieda, M., Tominaga, M., Yagami, K., Sugiyama, F., Goto, K., Yanagisawa, M., & Sakurai, T. (2003). Hypothalamic orexin neurons regulate arousal according to energy balance in mice. Neuron, 38(5), 701-713. https://pubmed.ncbi.nlm.nih.gov/12797956/
Written by Kat Fu, M.S., M.S. – Last reviewed: May 2026 – 9 references cited
