Resetting your circadian rhythm takes different amounts of time depending on which clock you are resetting and what caused the misalignment. The suprachiasmatic nucleus — the brain’s master pacemaker — re-entrains to a new light schedule in 1 to 3 days. Peripheral clocks in the liver, gut, and muscle take 5 to 8 additional days because they respond to feeding, temperature, and glucocorticoids rather than light. A complete reset requires realigning central and peripheral clocks using the right zeitgeber for each one.
“Reset your circadian rhythm” is among the top health-related searches online. The standard advice covers morning sunlight, avoiding screens at night, and keeping a consistent schedule. These recommendations address the suprachiasmatic nucleus (SCN) — but the body runs dozens of peripheral clocks, and they do not all respond to the same cues or on the same timeline.
This article covers why different clocks reset at different speeds, evidence-based timelines for common scenarios — jet lag, night-work schedules, social jetlag, age-related phase advance — and which tools re-entrain which clocks. Each section synthesizes the mechanisms covered across the circadian cluster series: from melatonin’s role as a chronobiotic to how caffeine delays circadian timing. For individual mechanisms, see the linked sibling articles throughout.
Why Does the Master Clock Reset Faster Than the Rest of Your Body?
The suprachiasmatic nucleus responds directly to light via melanopsin-containing retinal ganglion cells and can re-entrain to a new light schedule within 1 to 3 days. Peripheral clocks in the liver, kidney, gut, and muscle are not directly light-sensitive — they rely on downstream cues from the suprachiasmatic nucleus (glucocorticoids, autonomic innervation, body temperature) and on behavioral zeitgebers (feeding-fasting cycles, physical activity). These indirect pathways run on slower timescales, producing a 5- to 8-day lag after any schedule change.
The speed difference comes down to how each clock receives its timing information.
The SCN sits behind the optic chiasm and receives photic input from melanopsin-expressing retinal ganglion cells. When the light-dark cycle changes, the SCN detects the new pattern and adjusts within 1 to 3 days. Cuesta et al. (2015) demonstrated that glucocorticoid-mediated entrainment of peripheral clock genes in human cells follows a slower timeline, with peripheral tissues showing significant phase shifts after 6 days of consistent cortisol rhythm exposure (Cuesta et al., 2015).
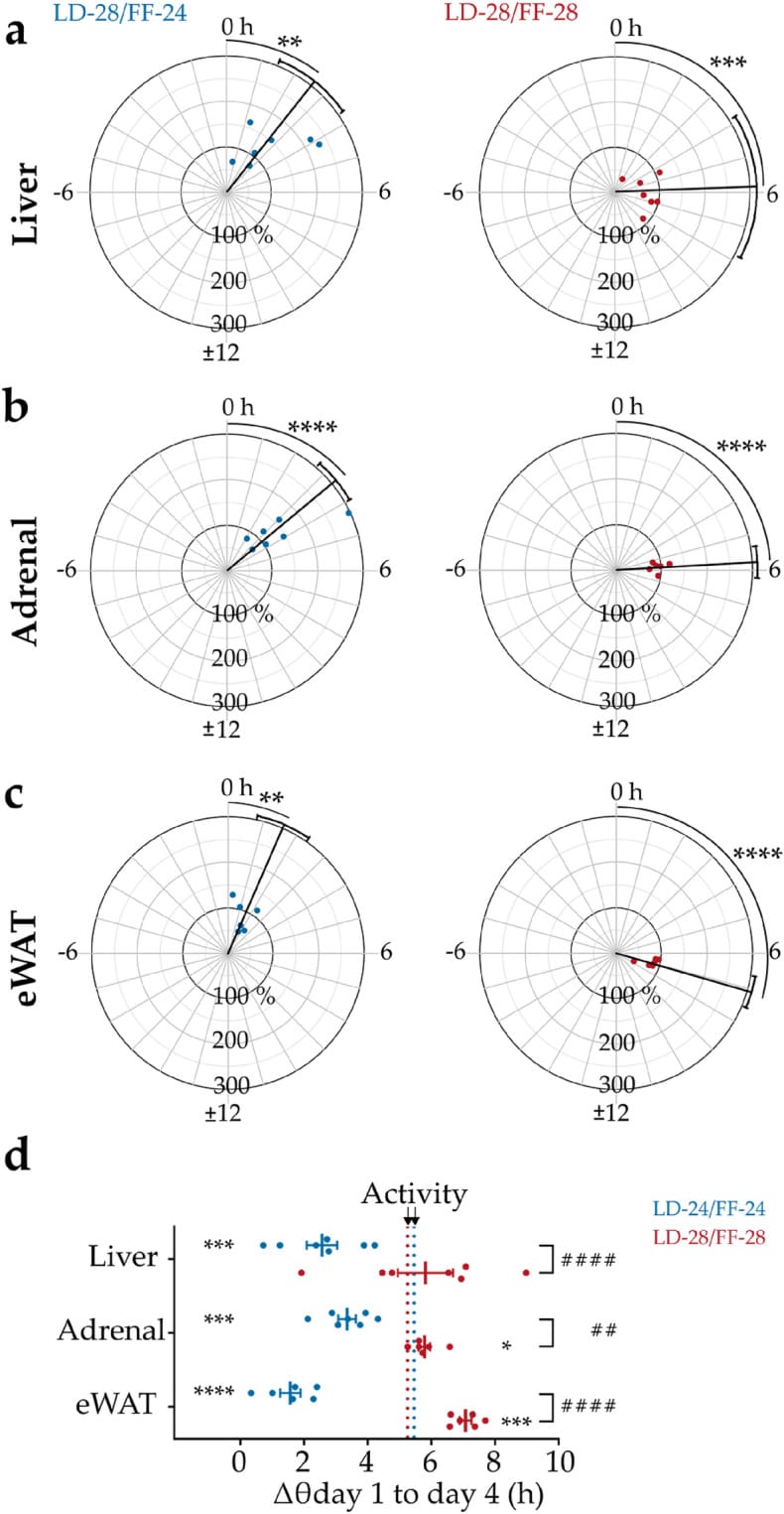
Nicholls et al. (2019) reviewed the evidence for internal desynchrony caused by circadian clock resetting: during light-induced phase resetting (such as simulated jet lag), SCN markers re-entrain while peripheral tissue clock gene rhythms in the liver and other organs take days longer to realign (Nicholls et al., 2019).
When the timing cues themselves conflict — for example, when light exposure says “daytime” but food intake says “nighttime” — the peripheral clocks face competing instructions. Heyde and Oster (2022) induced full internal desynchrony within 4 days by misaligning the light-dark cycle and feeding schedule. When timed food was added as a consistent cue, peripheral clock synchrony improved — but at the cost of reduced clock gene amplitude (Heyde & Oster, 2022).
This is the core reason that a “circadian reset” takes longer than standard advice suggests. Moving the SCN is the first step. Waiting for the liver, gut, and muscle clocks to follow is the rest. The weekly version of this mismatch is social jetlag — a two-hour weekend sleep-schedule change can desynchronize peripheral clocks for days after the SCN has already corrected.
How Long Does Each Common Scenario Take to Re-Entrain?
Jet lag recovery averages approximately 1 day per timezone crossed without targeted light and melatonin timing — faster westward (1.5 hours per day of phase delay) than eastward (1 hour per day of phase advance). Night-work re-entrainment is incomplete even after years on a fixed schedule, because the suprachiasmatic nucleus remains anchored to the light-dark cycle. Social jetlag repeats weekly: the suprachiasmatic nucleus corrects by Monday but peripheral clocks lag through midweek. Natural-light camping advanced the circadian clock by approximately 1.4 hours in just two days — representing roughly 69% of the advance achieved after a full week of natural light exposure.
Jet Lag
The direction of travel determines re-entrainment speed. Roach and Sargent (2019) documented that re-entrainment is faster westward than eastward. For a 9-timezone shift, their model estimates complete adaptation in approximately 7 days westward versus 8 days eastward. General circadian literature estimates approximately 1 hour per day of phase advance (eastward) and 1.5 hours per day of phase delay (westward). Phase delays are faster because the human circadian period runs slightly longer than 24 hours — westward travel aligns with this natural tendency (Roach & Sargent, 2019).
Vosko et al. (2010) documented that eastward flights produce longer-lasting desynchrony than westward flights. For a 6-timezone eastward crossing, full SCN re-entrainment can take 6 or more days without targeted light and melatonin timing (Vosko et al., 2010). Peripheral clock recovery extends beyond this — the liver, gut, and metabolic rhythms lag the SCN by the additional 5-to-8-day window.
Night-Work Schedules
The SCN does not re-entrain to an overnight work schedule, even after years of consistent night work. Boivin et al. (2022) documented that the SCN remains anchored to the outdoor light-dark cycle, producing persistent misalignment between the master clock and the imposed work schedule (Boivin et al., 2022).
Kosmadopoulos et al. (2024) documented the same pattern in police officers working rotating schedules: circadian adaptation of melatonin and cortisol rhythms was both slow and incomplete, with only 30% and 24% of officers achieving adaptation based on melatonin and cortisol rhythms, respectively (Kosmadopoulos et al., 2024).
Social Jetlag
A 2-hour weekend sleep delay desynchronizes peripheral clocks for days after the SCN has already corrected. The SCN re-entrains to the Monday alarm within a day, but peripheral clocks in the liver, gut, and metabolic tissues take until midweek or later to catch up. This weekly cycle is covered in the social jetlag article.
Natural Light Reset
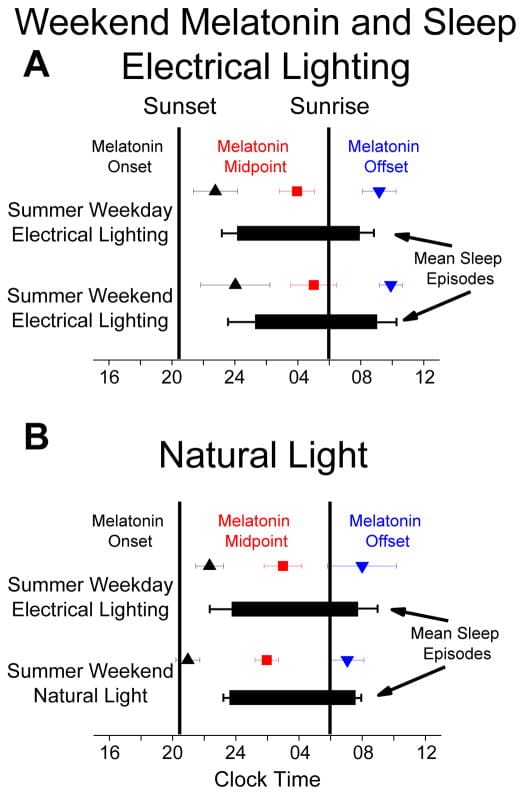
Stothard et al. (2017) sent participants camping for a weekend — two days with no electric light. The circadian clock advanced by approximately 1.4 hours, and melatonin onset moved earlier relative to the sleep period. This advance represented roughly 69% of the circadian timing change achieved after a full week of natural light exposure (Stothard et al., 2017). This demonstrates the SCN’s capacity for rapid adjustment when light-dark timing is unambiguous. But even under these optimal conditions, peripheral re-entrainment takes longer.
Age-Related Phase Advance
After age 40 to 50, the SCN itself begins to change: VIP neuron count declines, reducing the amplitude of the master clock’s output, and the aging lens filters more 480-nanometer light before it reaches the retina. These structural changes slow re-entrainment and reduce the SCN’s ability to recover from schedule disruptions. The full mechanism is covered in the aging circadian article.
What Tools Reset Which Clocks — and How Fast?
Morning bright light re-entrains the suprachiasmatic nucleus and can produce 2 or more hours of circadian phase advance in 3 days when combined with timed low-dose melatonin. Meal timing re-entrains peripheral clocks in the liver and gut — and retains full entrainment power even when age-related sympathetic decline weakens other peripheral zeitgebers. Combined light, melatonin, and meal timing address both central and peripheral clocks, producing faster and more complete re-entrainment than any single tool.
Morning Bright Light
Light is the primary zeitgeber for the SCN. Crowley and Eastman (2015) tested a 3-day phase advance approach using intermittent morning bright light (~5,000 lux) combined with 0.5 mg afternoon melatonin and a gradually advancing sleep schedule. The 2-hour bright light group achieved a mean DLMO (dim light melatonin onset) advance of 2.4 hours over 3 days. Notably, 30 minutes of morning bright light produced 75% of the maximum phase advance achieved by 2 hours, meaning a practical morning light exposure of 30 minutes captures the majority of the benefit (Crowley & Eastman, 2015).
How much light is needed depends on wavelength. Melanopsin peaks at 480 nanometers, and the minimum effective dose is approximately 250 melanopic EDI (equivalent daylight illuminance) — covered in the melanopic lux article.
Low-Dose Melatonin as a Chronobiotic
Melatonin’s circadian-resetting effect is separate from its sedative effect. Burgess et al. (2010) mapped the melatonin phase response curve for 0.5 mg and 3.0 mg doses and found that both produced similarly sized maximum phase advances when taken at optimal timing — 2 to 4 hours before DLMO for the 0.5 mg dose. The low dose was as effective as the high dose, indicating that melatonin’s chronobiotic action does not require high-dose administration (Burgess et al., 2010). Note that this chronobiotic capacity depends on adequate endogenous melatonin production, which declines with pineal gland calcification over the lifespan.
This distinction between chronobiotic dosing (0.5 mg, timed to the phase response curve) and sedative dosing (3 to 10 mg, taken at bedtime) is central to understanding why melatonin works for jet lag but often does not work for chronic insomnia.
Meal Timing for Peripheral Clocks
Feeding-fasting cycles are one of the strongest peripheral zeitgebers. Engin (2024) demonstrated that time-restricted eating restores peripheral clock alignment in the liver, gut, and adipose tissue by providing a consistent metabolic timing cue (Engin, 2024).
In aging, as sympathetic innervation to peripheral organs weakens, meal timing retains full entrainment power — making it one of the more reliable tools for peripheral re-entrainment in older adults. This is discussed in the aging circadian article.
Combined Approaches
Burke et al. (2013) tested light and melatonin in a 4-condition randomized controlled trial and found that the phase-advancing effects were additive: combining bright morning light with timed melatonin produced a larger advance than either alone (Burke et al., 2013). Crowley and Eastman (2013) showed that adding afternoon melatonin to a gradually advancing sleep schedule enhanced DLMO advances over 3 days beyond what schedule adjustment alone achieved (Crowley & Eastman, 2013).
A combined approach — morning bright light, timed low-dose melatonin, and consistent meal timing — addresses both central and peripheral clocks. Light and melatonin move the SCN. Meal timing moves the liver, gut, and metabolic tissues. Running all three in parallel produces faster re-entrainment than any single tool.
What Slows Down or Prevents a Circadian Reset?
Several factors slow or prevent circadian re-entrainment. Caffeine delays the circadian phase by approximately 40 minutes per dose through the adenosine-cAMP pathway. Lens yellowing with age reduces the 480-nanometer light reaching the retina, weakening the light-based entrainment cue. Suprachiasmatic nucleus neuron loss reduces the amplitude of the master clock output. And intermittent hypoxia from sleep apnea suppresses clock genes through a pathway that may not fully recover even with prolonged CPAP use.
Caffeine
A single dose of caffeine (equivalent to a double espresso) taken 3 hours before bedtime delays the DLMO by approximately 40 minutes. Burke et al. (2015) demonstrated that this occurs through adenosine receptor blockade, which increases intracellular cAMP and lengthens the circadian period (Burke et al., 2015). For someone using morning light to advance their clock by 1 to 1.5 hours per day, a single evening caffeine dose erases roughly one-third to one-half of that progress. The full adenosine-cAMP mechanism is covered in the caffeine circadian delay article.
Lens Yellowing
The human lens yellows with age, filtering progressively more short-wavelength light. At 480 nanometers — melanopsin’s peak sensitivity — light transmission decreases by approximately 1% per year. By age 60 to 70, a large fraction of circadian-relevant light is absorbed before reaching the retinal ganglion cells that drive SCN entrainment. Compensating requires brighter light sources or longer exposure.
Suprachiasmatic Nucleus Neuron Loss
The SCN contains approximately 20,000 neurons. With aging, VIP (vasoactive intestinal peptide) neuron count declines, and the amplitude of the SCN’s electrical output weakens — VIP neuron count correlates with circadian rhythm strength. This is a structural change — no behavioral approach restores lost neurons. Reduced SCN amplitude weakens the timing cue sent to peripheral clocks, making the entire re-entrainment process slower. These mechanisms are detailed in the aging circadian article.
Clock Gene Suppression from Sleep Apnea
Intermittent hypoxia from obstructive sleep apnea suppresses core clock genes (BMAL1, PER, CRY) in peripheral tissues. Even after prolonged periods of CPAP use, clock gene expression may not fully recover — suggesting that hypoxia-driven clock gene damage may be difficult to reverse. This is one reason individuals using CPAP may continue to feel exhausted long after their apnea-hypopnea index normalizes.
Evening Light Exposure
Evening light works against any daytime phase advance. Research shows that 2 hours of evening light exposure can produce a circadian delay of approximately 1 hour or more — nearly equivalent to the 1 to 1.5 hours of phase advance achievable with a full morning of bright light. This means an evening spent in bright artificial light can erase a full day of circadian re-entrainment progress. Managing evening light exposure is covered in the melanopic lux article.
The number of blockers present — and whether they are behavioral (caffeine, evening light) or structural (lens yellowing, SCN neuron loss, clock gene suppression) — determines whether a given reset timeline applies.
Many people have more than one cause contributing to their sleep disruption. The circadian re-entrainment challenges covered in this article may compound with metabolic, hormonal, inflammatory, or autonomic factors. Identifying which causes might be involved is a useful next step.
Find out which causes might be driving your 3 AM wakeups →
Frequently Asked Questions
Can You Reset Your Circadian Rhythm in One Day?
The suprachiasmatic nucleus can move by 1 to 1.5 hours in a single day with bright morning light. Stothard et al. (2017) showed that after two days of camping in natural light, the circadian clock advanced by approximately 1.4 hours — representing roughly 69% of the advance achieved after a full week of natural light exposure. But peripheral clocks take 5 to 8 days to re-entrain. A one-day reset addresses the central clock, not the full circadian architecture — central and peripheral re-entrainment requires consistent timing cues maintained over at least a week (Stothard et al., 2017).
Does Fasting Help Reset Your Circadian Rhythm?
Time-restricted eating can re-entrain peripheral clocks in the liver and gut by providing a feeding-fasting zeitgeber that functions independently of light (Engin, 2024). When meal timing and light timing are misaligned, timed food intake improves internal synchrony between peripheral clocks, though it may simultaneously weaken clock gene amplitude (Heyde & Oster, 2022). Fasting does not re-entrain the SCN directly — light remains the primary zeitgeber for the master clock. But as a peripheral clock reset tool, consistent meal timing is one of the strongest available cues.
Should You Pull an All-Nighter to Fix Your Sleep Schedule?
No evidence supports all-nighters as a circadian reset strategy. Sleep deprivation disrupts cognitive function and glucose metabolism without producing a lasting phase change. The evidence-based alternative: gradual sleep schedule advances of approximately 1 hour per day combined with timed melatonin and morning light. Crowley and Eastman (2015) tested a 3-day approach where 30 minutes of morning bright light combined with 0.5 mg of afternoon melatonin produced a 1.8-hour DLMO advance — without sleep deprivation (Crowley & Eastman, 2015).
Related Reading
- Circadian Rhythm Disruption: How a Misaligned Internal Clock Fragments Sleep, Drives 3AM Wakeups, and Reduces Sleep Depth — the full overview of circadian sleep disruption, including melatonin, cortisol, body temperature, peripheral clocks, and early-morning waking
- Why Does Melatonin Work for Jet Lag but Not Chronic Insomnia? — why melatonin works as a timing cue, not a general sleep-depth fix
- Is Your Pineal Gland Calcifying? How Age-Related Melatonin Production Loss Differs From Receptor Decline — how pineal calcification, melatonin output, and receptor decline diverge with age
- How Many Melanopic Lux Do You Need for Circadian Entrainment? — how melanopic light exposure sets the clock more directly than ordinary lux
- How Much Blue Light From Your Phone Suppresses Melatonin? The Dose-Duration Relationship — how screen brightness, duration, and melanopic irradiance affect melatonin timing
- Do Blue Light Glasses Help You Sleep? Amber vs Standard Lenses — What Studies Show — how amber lenses, clear lenses, and evening screens differ in sleep studies
- How Does Caffeine Delay Your Circadian Clock by 40 Minutes? — how caffeine delays circadian phase through adenosine and clock-gene timing
References
- Burgess, H. J., Revell, V. L., Molina, T. A., & Eastman, C. I. (2010). Human phase response curves to three days of daily melatonin: 0.5 mg versus 3.0 mg. The Journal of Clinical Endocrinology & Metabolism, 95(7), 3325–3331. https://pubmed.ncbi.nlm.nih.gov/20410229/
- Burke, T. M., Markwald, R. R., McHill, A. W., Chinoy, E. D., Snider, J. A., Bessman, S. C., Jung, C. M., O’Neill, J. S., & Wright, K. P., Jr. (2015). Effects of caffeine on the human circadian clock in vivo and in vitro. Science Translational Medicine, 7(305), 305ra146. https://pubmed.ncbi.nlm.nih.gov/26378246/
- Burke, T. M., Markwald, R. R., Chinoy, E. D., Snider, J. A., Bessman, S. C., Jung, C. M., & Wright, K. P., Jr. (2013). Combination of light and melatonin time cues for phase advancing the human circadian clock. Sleep, 36(11), 1617–1624. https://pubmed.ncbi.nlm.nih.gov/24179293/
- Boivin, D. B., Boudreau, P., & Kosmadopoulos, A. (2022). Disturbance of the circadian system in shift work and its health impact. Journal of Biological Rhythms, 37(1), 3–28. https://pubmed.ncbi.nlm.nih.gov/34969316/
- Crowley, S. J., & Eastman, C. I. (2013). Melatonin in the afternoons of a gradually advancing sleep schedule enhances the circadian rhythm phase advance. Psychopharmacology, 225(4), 825–837. https://pubmed.ncbi.nlm.nih.gov/23001190/
- Crowley, S. J., & Eastman, C. I. (2015). Phase advancing human circadian rhythms with morning bright light, afternoon melatonin, and gradually shifted sleep: Can we reduce morning bright-light duration? Sleep Medicine, 16(2), 288–297. https://pubmed.ncbi.nlm.nih.gov/25620199/
- Cuesta, M., Cermakian, N., & Boivin, D. B. (2015). Glucocorticoids entrain molecular clock components in human peripheral cells. The FASEB Journal, 29(4), 1360–1370. https://pubmed.ncbi.nlm.nih.gov/25500935/
- Engin, A. (2024). Misalignment of circadian rhythms in diet-induced obesity. Advances in Experimental Medicine and Biology, 1460, 27–71. https://pubmed.ncbi.nlm.nih.gov/39287848/
- Heyde, I., & Oster, H. (2022). Induction of internal circadian desynchrony by misaligning zeitgebers. Scientific Reports, 12, 1601. https://pubmed.ncbi.nlm.nih.gov/35102210/
- Kosmadopoulos, A., Boudreau, P., Kervezee, L., & Boivin, D. B. (2024). Circadian adaptation of melatonin and cortisol in police officers working rotating shifts. Journal of Biological Rhythms, 39(1), 49–67. https://pubmed.ncbi.nlm.nih.gov/37750410/
- Nicholls, S. K., Casiraghi, L. P., Wang, W., Weber, E. T., & Harrington, M. E. (2019). Evidence for internal desynchrony caused by circadian clock resetting. Yale Journal of Biology and Medicine, 92(2), 259–270. https://pubmed.ncbi.nlm.nih.gov/31249487/
- Roach, G. D., & Sargent, C. (2019). Interventions to minimize jet lag after westward and eastward flight. Frontiers in Physiology, 10, 927. https://pubmed.ncbi.nlm.nih.gov/31417411/
- Stothard, E. R., McHill, A. W., Depner, C. M., Birks, B. R., Moehlman, T. M., Ritchie, H. K., Guzzetti, J. R., Chinoy, E. D., LeBourgeois, M. K., Axelsson, J., & Wright, K. P., Jr. (2017). Circadian entrainment to the natural light-dark cycle across seasons and the weekend. Current Biology, 27(4), 508–513. https://pubmed.ncbi.nlm.nih.gov/28162893/
- Vosko, A. M., Colwell, C. S., & Avidan, A. Y. (2010). Jet lag syndrome: Circadian organization, pathophysiology, and management strategies. Nature and Science of Sleep, 2, 187–198. https://pubmed.ncbi.nlm.nih.gov/23616709/
Written by Kat Fu, M.S., M.S. ? Last reviewed: May 2026 ? 14 references cited
