GABA (gamma-aminobutyric acid) is the brain’s primary inhibitory neurotransmitter — the calming neurotransmitter responsible for dampening arousal-promoting neural circuits during sleep. When GABAergic function is impaired, those arousal circuits stay active during hours when they should be suppressed.
This article covers what impaired GABAergic function feels like at night, what brain imaging has revealed, and how to distinguish GABA-related sleep disruption from other causes. For the mechanism in depth, see Can Low GABA Cause Waking Up at 3am?. Impaired GABA is one of several hormonal and neurochemical mechanisms that fragment sleep in men — the full overview is in Why Men’s Hormones Disrupt Sleep.
What Does Low GABA Feel Like at Night?
What Does Racing Thoughts From Low GABA Look Like?
Plante et al. (2012) measured GABA in 20 non-medicated adults with insomnia and 20 matched healthy controls. GABA was reduced in the ACC (p = 0.03) and the occipital cortex (p = 0.0005), but not in the thalamus — indicating the deficit is region-concentrated rather than brain-wide.
The racing thoughts are not a character problem or a stress management issue. They reflect insufficient inhibitory neurotransmission in the region of the brain that suppresses repetitive thinking.
Why Does the Wired-but-Tired Feeling Happen?
GABA is what allows sleep-promoting regions (including the ventrolateral preoptic nucleus) to suppress the wakefulness-promoting circuits in the hypothalamus and brainstem. When GABAergic tone is insufficient, both states coexist: the body’s fatigue and the brain’s activation — that distinctly uncomfortable feeling of being wired rather than tired at the hour you need to be sleeping.
How Is Nighttime Anxiety From Low GABA Different From Daytime Anxiety?
If you wake at 2am or 3am and your mind is immediately sharp — fully alert, not drowsy — that pattern is more consistent with impaired GABAergic inhibition than with blood sugar fluctuation (which tends to produce grogginess) or nocturia (which produces a physical urge). Once the arousal circuit fires without sufficient GABAergic restraint, it tends to self-sustain — returning to sleep can take 45 minutes to two hours.
How Do You Know If Your GABA Is Low?
Why Don’t Blood Tests Detect Low GABA?
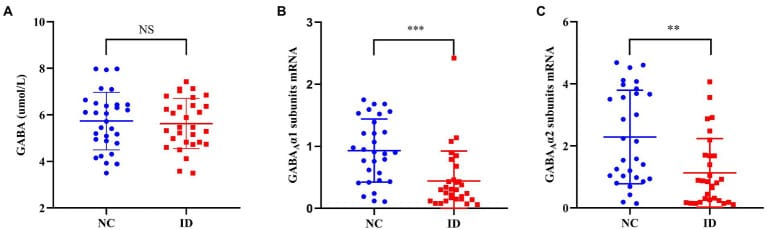
Xiang et al. (2023) compared 30 adults with insomnia against 30 healthy controls, measuring both serum GABA and GABA-A receptor subunit mRNA from peripheral blood:
- Serum GABA: No difference between groups (p = 0.733)
- GABA-A receptor alpha-1 subunit mRNA: Reduced in insomnia (p < 0.001)
- GABA-A receptor alpha-2 subunit mRNA: Reduced in insomnia (p = 0.001)
In healthy controls, serum GABA correlated positively with receptor expression — a relationship absent in the insomnia group. The problem may not be how much GABA is present, but whether the brain’s inhibitory receptors can respond to it.
What Does Brain Imaging Show About GABA and Insomnia?
Winkelman et al. (2008): Sixteen unmedicated adults with insomnia had approximately 30% lower whole-brain GABA than 16 matched controls. Lower GABA correlated with more nighttime wakefulness (r = -0.71, p = 0.002).
Plante et al. (2012): GABA reductions were concentrated in the ACC (p = 0.03) and occipital cortex (p = 0.0005), but not the thalamus — region-concentrated, not brain-wide.
Park et al. (2020): In 166 adults, those sleeping fewer than 6 hours had lower ACC GABA than those sleeping 6 or more hours (p = 0.03). Glutamate and glutamine did not differ — the deficit was limited to the inhibitory neurotransmitter.
What Nighttime Pattern Identifies Low GABA?
- Racing thoughts at sleep onset or upon waking — an inability to stop the stream of thought
- Full alertness upon waking — the mind is sharp within seconds (contrast with the grogginess of blood sugar-related waking)
- Difficulty returning to sleep — once awake, the return to sleep takes 30 minutes or longer
- Nighttime anxiety without an identifiable trigger — diffuse unease rather than worry about something particular
- Wired rather than tired — physical fatigue and mental activation coexisting
If this cluster is present in the absence of an obvious external cause (caffeine, alcohol, acute stress), impaired GABAergic function is a plausible contributor.
Does Low GABA Cause Anxiety at Night?
Why Do Anxiety and Insomnia Co-Occur So Often?
MRS studies confirm GABA deficits in both conditions, and the same receptor subtypes (GABA-A alpha-1 and alpha-2) are implicated in both (Jiang et al., 2025). The ACC governs both rumination suppression and emotional self-regulation — lower GABA in this region can produce both experiences from a single deficit.
What Weakens GABA Function Over Time?
Jiang et al. (2025) reviewed three pathways by which gut-derived GABA may influence the brain: direct absorption from the gastrointestinal tract into circulation, vagal afferent transmission from GABA-producing gut microbes to the brainstem, and microbiome-mediated modulation of central GABA receptor expression.

Grant et al. (2026) tested this in a randomized, double-blind, placebo-controlled trial of 139 adults. After six weeks on a GABA-modulating probiotic (Lactiplantibacillus plantarum Lp815), 77.3% achieved a 4-point or greater insomnia improvement vs. 57.8% in placebo (p = 0.02). Anxiety scores were also reduced (p < 0.05), and urinary GABA rose within one week (p < 0.05) — inversely correlated with both insomnia severity (r = -0.30) and anxiety (r = -0.48) at week 2.
Does GABA Deficiency Affect Men Differently Than Women?
Testosterone is metabolized into androstanediol, a positive allosteric modulator of GABA-A receptors — it enhances the receptor’s response to GABA (Reddy & Jian, 2010). As testosterone declines with age, this neurosteroid-mediated enhancement declines as well, compounding the age-related loss of GABA production and receptor density.
This may partly explain why sleep disruption in men during their 40s and 50s often presents with the wired-but-tired, racing-thought pattern characteristic of GABAergic impairment. The Grant et al. (2026) trial showed women had a stronger anxiety reduction (p < 0.01 for women vs. p < 0.05 overall), suggesting sex-differentiated GABAergic responses not yet fully understood. A fuller discussion is in Does GABA Affect Testosterone and Sleep in Men?.
The racing thoughts, wired-but-tired pattern, and 3am waking associated with impaired GABA overlap with other sleep disruption mechanisms. Cortisol rhythm changes, testosterone decline, metabolic instability, and inflammatory processes might all be contributing alongside weakened GABAergic function. In many people, more than one of these is involved — and addressing only one while the others persist can leave the sleep disruption partially unresolved.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
What Causes GABA Deficiency?
Is GABA Deficiency the Cause of Primary Insomnia?
How Do You Test for GABA Deficiency?
Related Reading
- Hormonal Sleep Disruption in Men — How testosterone, cortisol, growth hormone, and GABA interact to fragment sleep in men
- Can Low GABA Cause Waking Up at 3am? — The GABAergic mechanism behind 3am waking
- Do GABA Supplements Help You Stay Asleep Through the Night? — Trial evidence for oral GABA and the blood-brain barrier question
- Does GABA Affect Testosterone and Sleep in Men? — How testosterone-derived neurosteroids modulate GABA-A receptors
- How Do You Increase GABA Levels Naturally for Better Sleep? — Exercise, yoga, fermented foods, and gut health for GABA support
- Does Low Testosterone Cause Sleep Problems in Men? — The bidirectional testosterone-sleep feedback loop
- Can a Cortisol Spike Wake You Up at 3am? — Cortisol-testosterone axis and nocturnal waking
- Does Growth Hormone Decline Affect Your Sleep After 40? — GH-SWS coupling and age-related decline
- Does Andropause Cause Insomnia? What Men Over 50 Need to Know — Compound hormonal decline in aging men
- Can Belly Fat Lower Your Testosterone and Disrupt Your Sleep? — How visceral fat suppresses testosterone through aromatase and disrupts sleep
- Can Ultra-Processed Food Lower Testosterone and Disrupt Sleep? — How endocrine-disrupting chemicals in processed food suppress testosterone and degrade sleep
- Can Inflammation Suppress Testosterone and Disrupt Your Sleep? — How inflammatory cytokines suppress testosterone production at the brain and testicular level
- Does Testosterone Replacement Therapy Affect Sleep? — How TRT affects sleep quality, its interaction with sleep apnea, and the role of body weight
References
1. Winkelman JW, Buxton OM, Jensen JE, et al. Reduced brain GABA in primary insomnia: preliminary data from 4T proton magnetic resonance spectroscopy (1H-MRS). Sleep. 2008;31(11):1499-1506. PubMed
2. Plante DT, Jensen JE, Schoerning L, Winkelman JW. Reduced gamma-aminobutyric acid in occipital and anterior cingulate cortices in primary insomnia: a link to major depressive disorder? Neuropsychopharmacology. 2012;37(6):1548-1557. PubMed
3. Park S, Kang I, Edden RAE, et al. Shorter sleep duration is associated with lower GABA levels in the anterior cingulate cortex. Sleep Medicine. 2020;71:1-7. PubMed
4. Xiang T, Liao J, Cai Y, et al. Impairment of GABA inhibition in insomnia disorders: evidence from the peripheral blood. Frontiers in Psychiatry. 2023;14:1134434. PubMed
5. Zhu W, Yuan H, Bhatt S, et al. GABA and its receptors in insomnia. Heliyon. 2024;10(24):e40665. PubMed
6. Jiang C, Chen Y, Sun T. From the gut to the brain: mechanisms and applications of gamma-aminobutyric acid (GABA) for anxiety and insomnia. Frontiers in Neuroscience. 2025;19:1570173. PubMed
7. Grant AD, et al. Lactiplantibacillus plantarum Lp815 improves sleep and increases urinary GABA in a randomized, double-blind, placebo-controlled study of sleep disturbance. Scientific Reports. 2026. PubMed
8. Reddy DS, Jian K. The testosterone-derived neurosteroid androstanediol is a positive allosteric modulator of GABAA receptors. Journal of Pharmacology and Experimental Therapeutics. 2010;334(3):1031-1041. PubMed
Written by Kat Fu, M.S., M.S. · Last reviewed: April 2026 · 8 references cited
