If you wake around 3am and melatonin has not fixed it, you’ve likely encountered GABA supplements as a next option. GABA (gamma-aminobutyric acid) is the brain’s primary calming neurotransmitter — it reduces neural excitability and is directly involved in initiating and maintaining sleep. The logic behind supplementing it sounds reasonable: if you’re wired rather than tired in the second half of your sleep, maybe you need more GABA.
The question is whether swallowing GABA in capsule form delivers it to the brain in useful concentrations.
This article covers the trial evidence for oral GABA supplements, the difference between fermented and synthetic forms, the blood-brain barrier question, and how magnesium and L-theanine relate to GABA function. It does not cover the mechanism of how GABA maintains sleep (see Can Low GABA Cause Waking Up at 3am?, publishing soon) or non-supplement approaches (see How Do You Increase GABA Levels Naturally for Better Sleep?, publishing soon). GABA-related sleep disruption is one of several hormonal mechanisms behind nighttime waking — the full picture is in Why Men’s Hormones Disrupt Sleep.
Can GABA Supplements Stop Waking Up at 3am?
What does the overall evidence say?
The broadest assessment is a 2020 review by Hepsomali et al., published in Frontiers in Neuroscience, which analyzed 14 placebo-controlled human trials of oral GABA (Hepsomali et al., 2020). The conclusion: there is “limited evidence” that oral GABA improves sleep in humans. The authors flagged small sample sizes across studies and noted that many of the positive trials were conducted by researchers with potential industry ties — raising questions about publication bias.
That’s the honest landscape. It doesn’t mean GABA supplements don’t work. It means the evidence base isn’t large enough or independent enough to draw confident conclusions.
Where the evidence is stronger
Within that landscape, several individual trials show positive results — especially those using fermented GABA rather than synthetic forms.
Byun et al. (2018) conducted a randomized, double-blind, placebo-controlled trial with 40 participants who had insomnia, giving the group 300 mg daily of GABA extracted from fermented rice germ for four weeks. Sleep latency — the time it takes to fall asleep — dropped from 13.4 minutes to 5.7 minutes in the GABA group, measured by polysomnography (Byun et al., 2018). The placebo group showed no change. Sleep efficiency improved from 79.4% to 86.1%, and Pittsburgh Sleep Quality Index (PSQI) scores improved from 11.0 to 9.8.
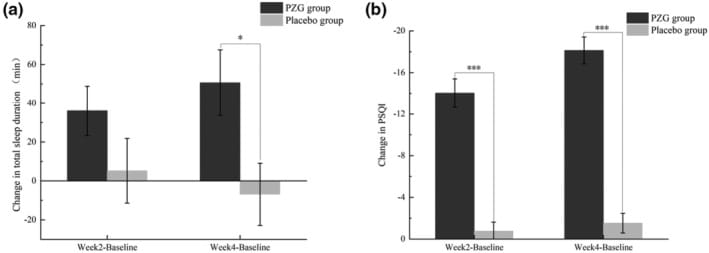
Hao et al. (2024) ran a double-blind RCT with 70 participants using a GABA-containing formula (combined with Poria cocos and Ziziphus spinosa) for four weeks. Sleep duration increased by 12.96% relative to placebo, measured by wrist actigraphy, and PSQI scores improved by 59.94% (Hao et al., 2024). The multi-ingredient design means GABA’s independent contribution can’t be isolated, but the actigraphy-confirmed results are notable.
Guimarães et al. (2024) tested 200 mg oral GABA daily for 90 days in 30 sedentary overweight women alongside a structured exercise program. The GABA group showed improved sleep efficiency, increased heart-rate variability (indicating greater parasympathetic tone), and reduced depression scores compared to placebo (Guimarães et al., 2024). The concurrent exercise program is a confound, but the autonomic changes suggest GABA may support sleep partly through parasympathetic activation rather than direct sedation.
The gap that matters: sleep onset vs. sleep maintenance
The majority of these trials measured falling asleep — sleep latency and early-night sleep quality. Fewer measured staying asleep through the night. If your primary problem is waking at 3am rather than difficulty falling asleep at 10pm, the existing trial data is less directly applicable. This is a gap in the evidence base, not a reason to rule out GABA supplements, but a reason to set realistic expectations about what the current research has tested.
Why Do GABA Supplements Wear Off During the Night?
The blood-brain barrier question
For decades, the standard position in neuroscience was that GABA cannot cross the blood-brain barrier (BBB) — the selective membrane that separates circulating blood from brain tissue. If that’s true, swallowing GABA is pointless: it would circulate in the blood but never reach the neurons that need it.
This is why many neurologists remain skeptical of oral GABA supplements. And as a blanket position, it’s outdated. Two 2025 reviews — Jiang et al. in Frontiers in Neuroscience and Li et al. in Foods — identify three pathways that resolve or complicate the old “GABA can’t cross the BBB” position.
Three pathways from gut to brain
Pathway 1: Transporter-mediated BBB entry. GABA doesn’t need to diffuse passively across the BBB. Two active transporters — GAT2 and BGT-1 — can carry GABA across the barrier (Jiang et al., 2025). This is active transport, not passive diffusion, meaning the brain has a mechanism for importing GABA from the bloodstream.
Pathway 2: Conversion to GHB. GABA can be metabolically converted to gamma-hydroxybutyrate (GHB), which crosses the BBB readily and activates GABA-B receptors — the receptor subtype involved in promoting slow-wave (deep) sleep (Li et al., 2025). This pathway is particularly relevant for sleep maintenance because GABA-B receptor activation is associated with deeper, more consolidated sleep architecture.
Pathway 3: Gut-brain axis via the vagus nerve. Oral GABA interacts with GABA receptors in the gut lining. Those gut receptors transmit information through the vagus nerve — the major nerve connecting the gut to the brain — which can influence central sleep circuits without GABA itself ever entering the brain (Jiang et al., 2025; Li et al., 2025). Gut bacteria, particularly Bifidobacterium and Lactobacillus species, also produce GABA endogenously, adding another dimension to this gut-brain communication.
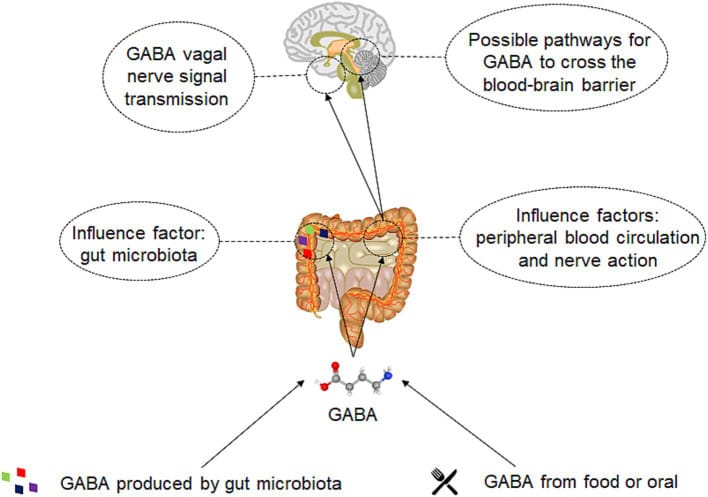
Fermented vs. synthetic GABA
This is where the distinction between PharmaGABA (fermented) and synthetic GABA becomes relevant. Fermented forms appear to bind more effectively to gut receptors (Jiang et al., 2025), which may explain why fermented GABA trials tend to show stronger results than synthetic GABA trials. If a large part of oral GABA’s effect comes through gut-vagal communication rather than direct BBB crossing, receptor binding affinity in the gut matters.
The timing problem
Yamatsu et al. (2016) conducted the only study that simultaneously measured plasma GABA levels and EEG sleep data. After 100 mg oral GABA, plasma concentrations peaked at approximately 30 minutes and then declined. Sleep latency shortened and non-REM sleep increased — but both effects were strongest around the sleep-onset window (Yamatsu et al., 2016).
This creates a timing problem for 3am waking. Cortisol begins rising between 2am and 6am as part of the normal cortisol awakening response. If a GABA supplement taken at bedtime peaks around midnight and wanes by 2am, it misses the window when GABAergic support is needed. The supplement may help you fall asleep without helping you stay asleep — which is consistent with the trial data showing stronger effects on sleep latency than on sleep maintenance.
Can Magnesium Improve GABA and Help You Stay Asleep?
How magnesium supports GABA directly
Magnesium has a dual relationship with GABA. First, it is a natural GABA-A receptor agonist — meaning magnesium binds to and activates the same receptor that GABA itself uses to reduce neural excitability. Second, magnesium is a required cofactor for glutamic acid decarboxylase (GAD), the enzyme that converts glutamate (an excitatory neurotransmitter) into GABA (a calming neurotransmitter). Without adequate magnesium, GAD activity is reduced, and glutamate activity can increase relative to GABA.
This is why magnesium deficiency and poor sleep tend to co-occur. Magnesium directly participates in the biochemistry that produces and activates GABA.
Why magnesium glycinate in particular
Magnesium comes in many forms — oxide, citrate, threonate, glycinate, taurate. For sleep, magnesium glycinate has become the commonly recommended form in both health-focused communities and practitioner recommendations. The reason is the glycine component. Glycine is an amino acid with its own calming effects — it lowers core body temperature and has independent sleep-promoting properties. In magnesium glycinate, you get both the magnesium (supporting GABA receptor function and GABA production) and the glycine (supporting sleep through a separate mechanism).
L-theanine and the GABA connection
L-theanine — the amino acid found in green tea — is often recommended alongside GABA and magnesium. L-theanine is not a GABA supplement itself, but it supports GABAergic tone indirectly by increasing brain GABA concentrations through modulation of glutamate receptors. It also increases alpha brain wave activity, which is associated with a state of calm alertness.
The practical question for someone waking at 3am is whether these compounds are complementary or redundant. They work through different mechanisms: GABA acts directly on GABA receptors, magnesium supports both GABA production and receptor activation, and L-theanine modulates the glutamate-GABA balance from the glutamate side. They are complementary, not redundant — which is why they often appear together in sleep-support formulations.
What supplements can and can’t address
Supplementation addresses availability — whether enough GABA, magnesium, or L-theanine is present for the relevant biochemistry to function. It does not address receptor sensitivity, hormonal disruption, or circadian misalignment. If GABA receptors are downregulated due to chronic stress or inflammation, adding more GABA to the bloodstream may not produce the expected effect. If the 3am waking is driven primarily by cortisol disruption or testosterone decline rather than low GABA, a GABA supplement is addressing the wrong contributor.
Supplements address one piece of the picture. GABA-related sleep maintenance difficulties often overlap with cortisol elevation, testosterone decline, metabolic instability, or circadian disruption — and these mechanisms compound each other. Understanding which factors might be contributing helps determine whether supplements, lifestyle changes, or both make sense for your situation.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
What Supplements Help You Stay Asleep Through the Night?
These three compounds address different parts of GABA-related sleep maintenance. GABA supplementation targets the neurotransmitter directly — though as discussed above, the evidence is stronger for sleep onset than for staying asleep. Magnesium supports both GABA production and receptor function. L-theanine modulates the excitatory-calming balance from the glutamate side.
If melatonin has not resolved your nighttime waking, that’s informative — it suggests the issue is downstream of circadian timing. GABA, magnesium, and L-theanine address different downstream mechanisms, which is why they are often combined.
Can GABA Supplements Help With Chronic Insomnia in Men?
Chronic insomnia is different from occasional poor sleep. When waking persists night after night for months, it usually reflects a self-reinforcing pattern: cortisol elevation fragments sleep, fragmented sleep elevates cortisol, and both can reduce GABA receptor sensitivity over time. Supplementing GABA in this context may help at the margins, but addressing the upstream drivers — stress load, inflammation, hormonal status — tends to produce more durable results.
In men, testosterone decline compounds this picture. Testosterone supports GABAergic tone, so declining testosterone can weaken GABA receptor function independent of GABA availability. See Does GABA Affect Testosterone and Sleep in Men? for the full mechanism.
Why Does GABA Wear Off During the Night?
This timing mismatch is one reason some people report that GABA helps them fall asleep but doesn’t prevent 3am waking. The supplement is active in the first half of the night, while the cortisol-driven arousal that wakes you occurs in the second half.
Some approaches to this include split dosing (a second smaller dose if you wake), extended-release formulations, or combining GABA with magnesium and L-theanine to support GABAergic tone through multiple mechanisms rather than relying on a single GABA bolus at bedtime. None of these approaches have been tested in dedicated sleep-maintenance trials, so they remain plausible strategies rather than evidence-confirmed solutions.
Related Reading
- Hormonal Sleep Disruption in Men — How testosterone, cortisol, growth hormone, and GABA interact to fragment sleep in men
- Can Low GABA Cause Waking Up at 3am? — The GABAergic mechanism behind 3am waking
- What Are the Signs of Low GABA at Night? — How to recognize impaired GABAergic function
- Does GABA Affect Testosterone and Sleep in Men? — How testosterone-derived neurosteroids modulate GABA-A receptors
- How Do You Increase GABA Levels Naturally for Better Sleep? — Exercise, yoga, fermented foods, and gut health for GABA support
- Does Low Testosterone Cause Sleep Problems in Men? — The bidirectional testosterone-sleep feedback loop
- Can a Cortisol Spike Wake You Up at 3am? — Cortisol-testosterone axis and nocturnal waking
- Does Growth Hormone Decline Affect Your Sleep After 40? — GH-SWS coupling and age-related decline
- Does Andropause Cause Insomnia? What Men Over 50 Need to Know — Compound hormonal decline in aging men
- Can Belly Fat Lower Your Testosterone and Disrupt Your Sleep? — How visceral fat suppresses testosterone through aromatase and disrupts sleep
- Can Ultra-Processed Food Lower Testosterone and Disrupt Sleep? — How endocrine-disrupting chemicals in processed food suppress testosterone and degrade sleep
- Can Inflammation Suppress Testosterone and Disrupt Your Sleep? — How inflammatory cytokines suppress testosterone production at the brain and testicular level
- Does Testosterone Replacement Therapy Affect Sleep? — How TRT affects sleep quality, its interaction with sleep apnea, and the role of body weight
References
1. Hepsomali P, Groeger JA, Nishihira J, Scholey A. Effects of oral gamma-aminobutyric acid (GABA) administration on stress and sleep in humans: a systematic review. Frontiers in Neuroscience. 2020;14:923. PubMed
2. Byun JI, Shin YY, Chung SE, Shin WC. Safety and efficacy of gamma-aminobutyric acid from fermented rice germ in patients with insomnia symptoms: a randomized, double-blind trial. Journal of Clinical Neurology. 2018;14(3):291-295. PubMed
3. Yamatsu A, Yamashita Y, Pandharipande T, Maru I, Kim M. Effect of oral γ-aminobutyric acid (GABA) administration on sleep and its absorption in humans. Food Science and Biotechnology. 2016;25(2):547-551. PubMed
4. Hao Y, Song W, Qu L. Effects of a combination of Poria cocos, Ziziphus spinosa, and gamma-aminobutyric acid (GABA) on sleep quality and skin health: a randomized double-blind placebo-controlled clinical trial. Food Science & Nutrition. 2024;12:3883-3894. PubMed
5. Guimarães AP, et al. GABA supplementation, increased heart-rate variability, emotional response, sleep efficiency and reduced depression in sedentary overweight women undergoing physical exercise. Journal of Dietary Supplements. 2024. PubMed
6. Jiang C, Chen Y, Sun T. From the gut to the brain, mechanisms and clinical applications of γ-aminobutyric acid (GABA) on the treatment of anxiety and insomnia. Frontiers in Neuroscience. 2025;19:1570173. PubMed
7. Li S, et al. Progress in research on the mechanism of GABA in improving sleep. Foods. 2025;14(22):3856. PubMed
Written by Kat Fu, M.S., M.S. · Last reviewed: April 2026 · 7 references cited
