Melatonin is one of the first supplements women reach for when sleep deteriorates during perimenopause. For many, it helps at first — then stops working, or never improves sleep continuity in a way that lasts. Sleep problems during menopause are rarely melatonin problems. Melatonin is one part of a longer production chain, and supplementing the end product does not correct what is happening earlier in that chain.
This article covers why melatonin supplementation does not improve sleep during menopause — the estrogen-serotonin-melatonin pathway, the meta-analytic evidence, and how the melatonin-sleep relationship itself changes after menopause. Hormonal changes are one of several causes of sleep disruption during this stage. For the full picture, see Hormonal Sleep Disruption in Women.
Does Estrogen Affect Melatonin Production?
The connection between estrogen and melatonin runs through serotonin. Estradiol — the primary form of estrogen before menopause — upregulates TPH2, the enzyme that converts tryptophan into serotonin (Hernandez-Hernandez et al., 2019). TPH2 is rate-limiting: the amount of serotonin a neuron can produce depends on how much TPH2 is available. When estradiol declines, TPH2 expression drops, and serotonin production decreases.
Serotonin is the biochemical precursor to melatonin. In the pineal gland, serotonin is acetylated and then methylated to form melatonin. If serotonin availability is reduced at the source, melatonin production is reduced downstream — regardless of how much supplemental melatonin is taken. The supplement adds the end product but does nothing to restore the production chain.
Estradiol also affects serotonin availability at points beyond synthesis. Bendis et al. (2024) showed that estradiol slows serotonin reuptake through estrogen receptor beta (ERbeta), modulates receptor sensitivity, and downregulates monoamine oxidase A and B (MAO-A/B) — the enzymes that break down serotonin. When estradiol declines, serotonin is produced less efficiently, removed from the synapse faster, and degraded more readily. The disruption is not limited to one step in the pathway; it occurs at multiple points simultaneously.
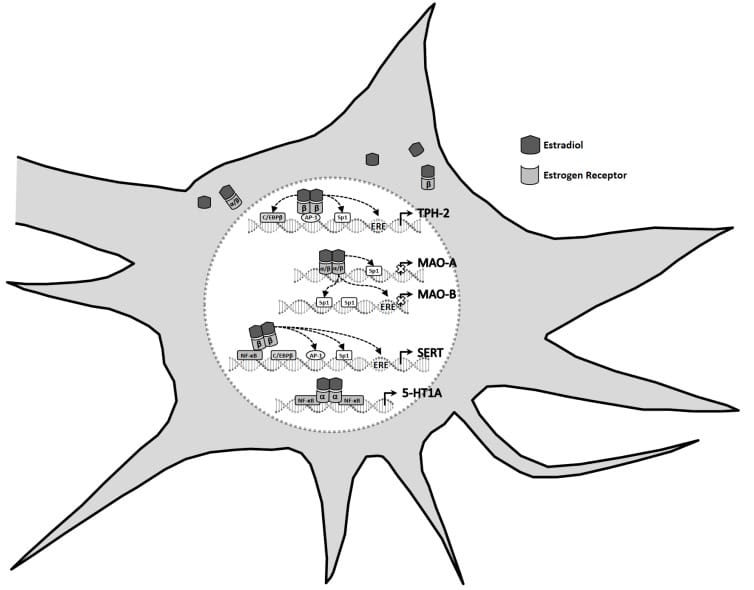
Supplementing melatonin during menopause often does not produce the expected result. The supplement adds melatonin to a body that may still be producing some of its own — but the upstream serotonin deficit, the increased serotonin degradation, and the reduced receptor sensitivity all remain. The production chain is impaired at multiple points, and melatonin supplementation addresses none of them.
Does Melatonin Supplementation Improve Sleep in Menopausal Women?
The meta-analytic evidence is consistent. Yi et al. (2021) pooled data from 8 randomized controlled trials involving 812 menopausal women. Melatonin doses ranged from 1 mg to 5 mg, taken over 3 to 12 months. The analysis found no improvement in sleep quality, general menopausal discomfort, mood, estradiol levels, or BMI. The one area where melatonin showed an effect was physical discomfort — but that did not translate into better sleep.
Five years later, Du & Tan (2026) conducted an updated meta-analysis of 7 randomized controlled trials (n=497), including newer studies. The conclusion was the same: melatonin supplementation did not improve sleep quality. It also did not improve anxiety or depression scores. Two independent research groups, analyzing overlapping but distinct sets of trials, reached the same finding.
The estrogen-serotonin-melatonin pathway explains this result. Melatonin supplementation adds the end product of the chain. But in menopause, the upstream cause — declining estrogen and its downstream effect on serotonin — remains. Supplementing melatonin does not restore serotonin production, does not correct the increased serotonin reuptake, and does not address the receptor sensitivity changes that estradiol withdrawal produces.
Melatonin can help with circadian timing — for people whose sleep-wake schedule is misaligned (e.g., jet lag, delayed sleep phase). But menopause insomnia is typically a sleep maintenance problem: difficulty staying asleep, waking in the early morning hours, fragmented sleep architecture. Circadian timing and sleep maintenance are different problems, and melatonin is better suited to the former than the latter.
Supplementing melatonin on the assumption that declining melatonin is the cause risks addressing a downstream effect while the upstream cause remains. As the research shows, in menopausal women, this approach has not produced measurable improvements in sleep quality across two decades of trials.
Does the Melatonin-Sleep Relationship Change After Menopause?
Toffol et al. (2021) used polysomnography (overnight sleep recording) in 17 perimenopausal and 18 postmenopausal women, measuring both nighttime melatonin concentrations and sleep architecture in detail.
In the perimenopausal group, the relationship was as expected: higher melatonin levels were associated with more slow-wave activity (the electrical pattern that defines deep sleep). Women with more melatonin had deeper sleep. This is the relationship that makes melatonin supplementation seem logical — if melatonin correlates with deep sleep, then adding melatonin should increase deep sleep.
In the postmenopausal group, the relationship reversed. Higher melatonin concentrations were associated with less slow-wave sleep and more awakenings. The women with more melatonin had lighter, more fragmented sleep — the opposite of the perimenopausal pattern.
The study did not establish a causal mechanism for the reversal, but several possibilities exist. Melatonin receptor sensitivity may change after prolonged estrogen decline. The downstream environment that melatonin acts on — including GABA availability, thermoregulation, and serotonin tone — has changed enough that melatonin alone cannot produce the same sleep architecture. Or the relationship may reflect compensatory melatonin production in women with worse sleep, rather than melatonin driving poor sleep.
Regardless of the mechanism, the practical implication is the same: in postmenopausal women, the assumption that more melatonin equals better sleep does not hold. Adding exogenous melatonin to a postmenopausal hormonal environment may not produce the result it would in a premenopausal or perimenopausal body.
What Addresses the Upstream Cause of Melatonin Decline in Menopause?
Haufe & Leeners (2023) reviewed the role of reproductive hormones in sleep across a woman’s lifespan and found that both estrogen and progesterone are positively associated with sleep during the menopausal transition. When hormone therapy restores estrogen and progesterone levels, sleep improvements follow — and the mechanism is upstream: estrogen restores serotonin production and receptor function, progesterone supports GABA-mediated sedation through its metabolite allopregnanolone, and both hormones contribute to thermoregulation and circadian timing.
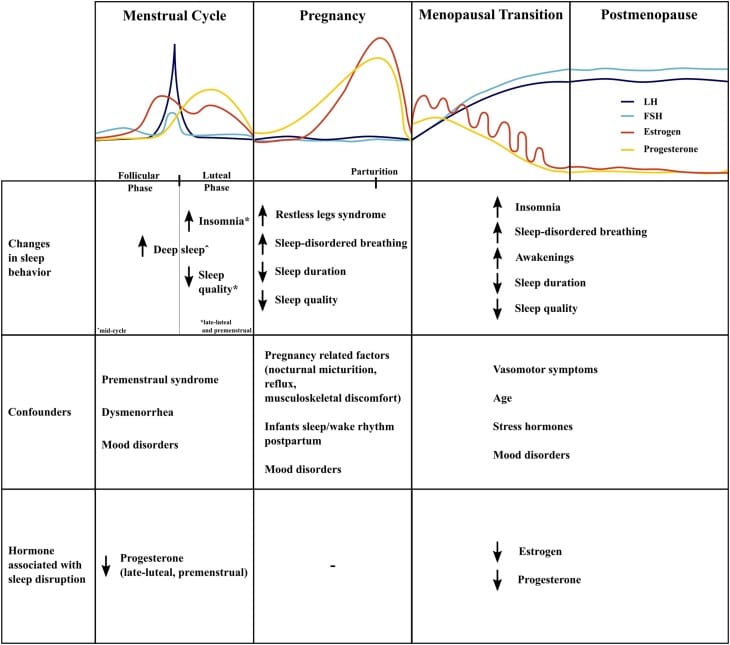
Melatonin supplementation adds the downstream product. Hormone therapy, when appropriate, addresses the upstream hormonal environment that produces melatonin (and supports sleep through several additional pathways). Jehan et al. (2017) noted the same pattern in their review — exogenous melatonin may reduce some nocturnal awakenings, but it does not address the upstream hormonal cause of disrupted melatonin synthesis.
Melatonin can be useful for circadian timing, for jet lag, and for certain sleep onset difficulties unrelated to hormonal status. But for sleep disruption driven by menopausal hormone decline, understanding where in the chain the problem originates matters for choosing an approach that can address it.
For more on hormone therapy and sleep, see Does HRT Help with Sleep in Menopause?. For progesterone’s role in sleep, see Does Progesterone Help You Sleep?.
Melatonin production is one pathway affected by hormonal changes during menopause — but it is rarely the only one. Cortisol regulation, thermoregulation, and autonomic balance might also be contributing. Understanding which causes are involved is a useful next step.
Find out which causes might be driving your 3am wakeups →
Frequently Asked Questions
Does Melatonin Reduce Hot Flashes?
The Yi et al. (2021) meta-analysis found that melatonin supplementation was associated with improvements in physical discomfort scores in menopausal women, which could include hot flash reduction. However, this physical discomfort improvement did not carry over into sleep quality improvements. The two outcomes were decoupled.
Even if melatonin reduces hot flash frequency or intensity through a separate mechanism, sleep quality during menopause is driven by multiple factors — serotonin decline, GABA changes, cortisol patterning, thermoregulatory instability. Reducing one contributor (hot flashes) without addressing the upstream hormonal cause of sleep disruption is unlikely to restore sleep architecture.
Should Sleep Apnea Be Ruled Out Before Relying on Melatonin?
Postmenopausal women have a higher prevalence of obstructive sleep apnea compared to premenopausal women (Haufe & Leeners, 2023). Progesterone supports upper airway dilator muscle tone, and estrogen contributes to fat distribution patterns that affect airway anatomy. When both decline, the risk of airway obstruction during sleep increases.
If melatonin supplementation is not improving sleep, sleep apnea is one explanation — particularly if sleep is fragmented with multiple awakenings, daytime fatigue, or reports of snoring or gasping. Melatonin cannot open an obstructed airway. For more on this connection, see Does Menopause Cause Sleep Apnea in Women?.
How Does Serotonin Affect Sleep During Menopause?
Serotonin’s role in menopause sleep disruption is often underestimated because the conversation focuses on melatonin. But serotonin contributes to sleep in two ways: directly, through its role in regulating sleep-wake transitions and promoting non-REM sleep; and indirectly, as the raw material from which melatonin is synthesized.
Estradiol supports serotonin at multiple points — increasing TPH2 expression (production), reducing MAO-mediated degradation, and modulating receptor sensitivity (Bendis et al., 2024). When estrogen declines, serotonin is affected across all of these mechanisms. This is part of why SSRIs (selective serotonin reuptake inhibitors) are sometimes used for menopause-related sleep and mood disruption — they increase available serotonin by slowing its reuptake, partially compensating for the reduced production.
For the full serotonin-sleep pathway and how it connects to other hormonal changes during menopause, see Hormonal Sleep Disruption in Women.
Related Reading
- Hormonal Sleep Disruption in Women — Full overview of estrogen, progesterone, and sleep architecture
- Why Do You Wake Up at 3am During Menopause? — The cortisol amplification pattern behind early-morning waking in perimenopause and menopause
- What Causes the ‘Wired but Tired’ Feeling in Menopause? — HPA axis dysregulation and hyperarousal that leave you exhausted but unable to sleep
- Why Can’t You Sleep Before Your Period? — How the progesterone crash in the late luteal phase fragments sleep and raises core body temperature
- Does Hormone Replacement Therapy Help with Sleep in Menopause? — What the clinical evidence shows about HRT’s effect on sleep architecture and hot-flash-driven waking
- Does Progesterone Help You Sleep? — The GABA-A receptor mechanism behind progesterone’s sleep-promoting effects and why dose timing matters
- Does Low Progesterone Cause Insomnia in Perimenopause? — Sleep maintenance from progesterone decline
- Can Night Sweats Disrupt Your Deep Sleep? — Thermoregulatory disruption and sleep fragmentation
- Does Menopause Reduce Your Deep Sleep? — Estrogen-dependent slow-wave and REM changes
- Does PMDD Cause Insomnia? — Severe cyclical sleep disruption
- Does Menopause Cause Sleep Apnea in Women? — Underdiagnosed hormone-airway connection
- Does FSH Affect Your Sleep During Menopause? — FSH as active sleep disruptor
References
1. Hernandez-Hernandez, O. T., Martinez-Mota, L., Herrera-Perez, J. J., & Jimenez-Rubio, G. (2019). Role of estradiol in the expression of genes involved in serotonin neurotransmission: Implications for female depression. Current Neuropharmacology, 17(5), 459–471. https://pmc.ncbi.nlm.nih.gov/articles/PMC6520586/
2. Bendis, P. C., Zimmerman, S., Onisiforou, A., Zanos, P., & Georgiou, P. (2024). The impact of estradiol on serotonin, glutamate, and dopamine systems. Frontiers in Neuroscience, 18, 1348551. https://pmc.ncbi.nlm.nih.gov/articles/PMC10998471/
3. Yi, M., Wang, S., Wu, T., Zhang, X., Jiang, L., & Fang, X. (2021). Effects of exogenous melatonin on sleep quality and menopausal symptoms in menopausal women: A systematic review and meta-analysis of randomized controlled trials. Menopause, 28(6), 717–725. https://pubmed.ncbi.nlm.nih.gov/33784263/
4. Du, J., & Tan, Y. (2026). A systematic review and meta-analysis of randomized controlled trials investigated the effects of melatonin supplementation on bone mineral density, quality of life, and sleep in menopausal women. Frontiers in Nutrition, 13, 1687221. https://doi.org/10.3389/fnut.2026.1687221
5. Toffol, E., Kalleinen, N., Himanen, S. L., Partonen, T., Haukka, J., & Polo-Kantola, P. (2021). Nighttime melatonin secretion and sleep architecture: Different associations in perimenopausal and postmenopausal women. Sleep Medicine, 81, 52–61. https://pubmed.ncbi.nlm.nih.gov/33639482/
6. Haufe, A., & Leeners, B. (2023). Sleep disturbances across a woman’s lifespan: What is the role of reproductive hormones? Journal of the Endocrine Society, 7(5), bvad036. https://pmc.ncbi.nlm.nih.gov/articles/PMC10117379/
7. Jehan, S., Jean-Louis, G., Zizi, F., Auguste, E., Pandi-Perumal, S. R., Gupta, R., Attarian, H., Brief, E., Nowakowski, S., & McFarlane, S. I. (2017). Sleep, melatonin, and the menopausal transition: What are the links? Sleep Science, 10(1), 11–18. https://pmc.ncbi.nlm.nih.gov/articles/PMC5611767/
Written by Kat Fu, M.S., M.S. · Last reviewed: April 2026 · 7 references cited
