Travelers crossing multiple time zones know eastbound flights feel harder to recover from. The mechanism behind the asymmetry also explains the day-3 crash, why digestive recovery lags sleep recovery by days, and why maximizing bright light after an eastbound flight can slow adjustment in certain cases. This article covers the circadian math behind the east-west asymmetry, quantified recovery timelines for both directions, how peripheral organs re-entrain at different speeds than the brain’s master clock, and why the worst day of jet lag sometimes arrives days after landing. It does not cover all forms of travel fatigue — only what is driven by the circadian clock. For the broader picture of how circadian disruption causes 3 AM wakeups at home, see the Circadian Rhythm Disruption overview: Circadian Rhythm Disruption.
Why Does Your Circadian Clock Re-Entrain Faster Going West Than East?
The suprachiasmatic nucleus (SCN) — the brain’s master circadian pacemaker — does not run on a 24-hour cycle. Measured under constant conditions without light-dark cues, the average human circadian period is approximately 24.2 hours. Each day, morning light anchors the clock forward to stay synchronized with the 24-hour day. Without that anchoring, the clock would progressively delay — wake time sliding later, sleep onset moving into the early morning hours.
This natural tendency toward delay is the core of the east-west asymmetry. Westbound travel requires the clock to delay — to extend the day — which aligns with what the SCN already tends to do. Eastbound travel requires the opposite: the clock must advance, compressing the day into fewer hours than its natural period. Phase advance opposes the clock’s intrinsic delay tendency.
A 2016 study by Lu and colleagues modeled the SCN as a population of coupled oscillators using the Kuramoto framework, parameterized from published circadian data. The model demonstrated that even a small tau excess above 24 hours is mathematically sufficient to produce the multi-day recovery differences that travelers experience. By analyzing phase-space dynamics after simulated time-zone transitions, the researchers showed that eastward travel pushes the SCN’s coupled oscillator network into a region of phase space where resynchronization dynamics slow down. Westward travel avoids this region. The direction of the phase change — advance versus delay — determines whether the oscillator network passes through the slow-recovery region or bypasses it.
The model also generated a prediction about individual differences. People whose tau is further above 24 hours experience a greater eastbound disadvantage. Individual tau is not something travelers typically know about themselves, but variation in this parameter predicts who will have the hardest time recovering from eastbound flights — and opens a path toward personalized pre-travel preparation once tau can be routinely measured.
How Many Days Does Your Jet Lag Last — and What Sets the Rate?
A 2024 PRISMA-compliant review by Ahmed and colleagues analyzed 23 studies to quantify east-west re-entrainment rates. The data confirmed the directional formula: westward travel requires approximately 0.5 days per time zone crossed for circadian realignment (roughly 2 hours of adjustment per calendar day), while eastward travel requires approximately 1 day per time zone. This means eastbound travel is approximately twice as disruptive per zone crossed.
The review attributed the asymmetry directly to endogenous tau exceeding 24 hours, making phase delay (westward) more facile than phase advance (eastward). Mental health consequences also diverged by direction: eastward travel over extended or repeated itineraries was associated with elevated anxiety and depression risk, while westbound travel was associated with elevated depression risk.
A separate study by Lemmer and colleagues provides rare human biomarker data comparing both directions. Thirteen male elite athletes flew westbound from Frankfurt to Atlanta (6 time zones), and 6 athletes flew eastbound from Munich to Osaka (8 time zones). All participants completed standardized twice-daily training sessions with blood pressure, heart rate, oral temperature, grip strength, salivary cortisol, and melatonin measured at baseline and on days 1, 4, 6, and 11 post-arrival.
All monitored physiological functions were disturbed on day 1 in both directions. Westbound recovery was achieved by day 5-6. Eastbound disruption persisted through day 7 and beyond.
A cardiovascular pattern emerged that differed by direction: blood pressure increased after westbound travel and decreased after eastbound travel. This indicates that circadian desynchrony manifests differently across organ types depending on whether the clock is advancing or delaying. Training performance impairment peaked within the first 4 days following westbound travel — earlier than the eastbound impairment peak — and salivary melatonin and cortisol profiles showed phase displacement that took longer to realign in the eastbound group.
Do Your Organs Re-Synchronize at Different Speeds After a Flight?
When travelers report feeling “better” after 3-4 days, what has often happened is that the SCN has begun to realign with the new light-dark cycle. But the clocks embedded in peripheral organs — the gut, liver, pancreas, heart, and immune tissues — run on a separate entrainment timeline. These peripheral clocks receive timing cues from the SCN through the sympathetic pathway, and they are also entrained by the feed-fast cycle (meal timing). After a time-zone change, the SCN begins adjusting to local light within 1-2 days. Peripheral organs follow later.
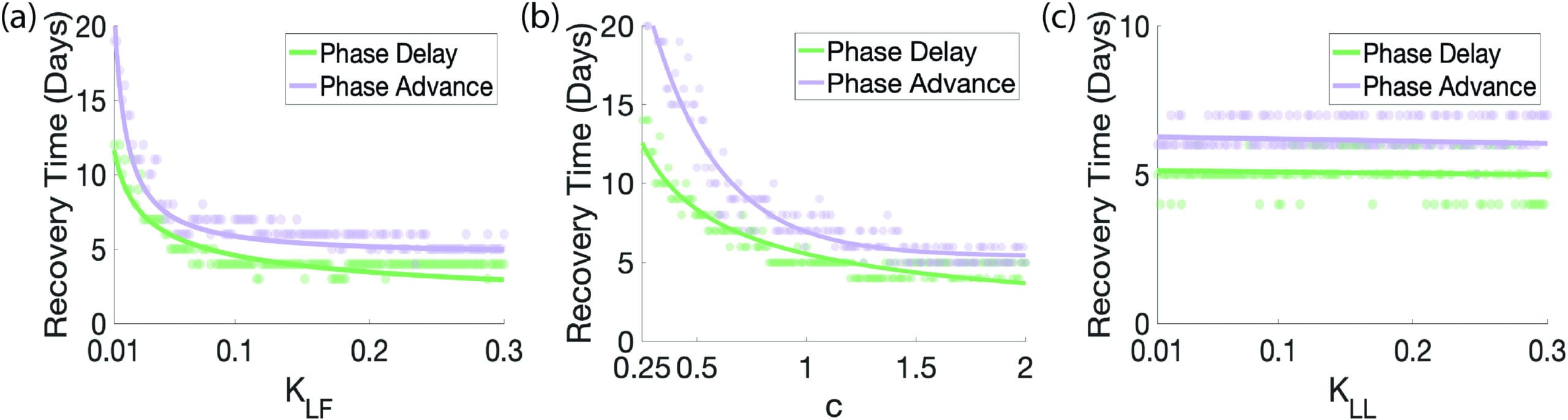
A 2023 study by Huang, Zhang, and Braun built a mathematical model of coupled central (SCN) and peripheral oscillators to quantify this lag and understand why it worsens with age. The model identified two age-related factors that impede peripheral re-entrainment: attenuated sympathetic pathway coupling from the SCN to peripheral tissues, and reduced light responsiveness in the central pacemaker.
When sympathetic coupling strength was reduced from 0.065 to 0.035 — representing the aging transition — peripheral clock re-entrainment extended from 5-6 days to 7-9 days. That is a 2-4 day delay with direct practical consequences for post-flight recovery. Weakening of central clock coupling alone, without altering peripheral coupling, did not affect peripheral re-entrainment rate. The sympathetic pathway from SCN to peripheral organs is the rate-limiting link in age-related recovery slowing, not the central pacemaker itself.
This architecture explains why peripheral organ-driven experiences — digestive disruption, immune suppression, metabolic impairment — can persist well after sleep timing feels restored. Even in younger travelers, peripheral clocks lag behind the SCN. The difference is less pronounced, but present.
The model also predicted a specific countermeasure: concentrating caloric intake at breakfast while omitting or minimizing dinner during the first 3 days post-arrival can accelerate peripheral re-entrainment back to 5 days — matching recovery rates seen in younger individuals. The feed-fast cycle serves as a potent circadian time cue for peripheral clocks that does not require any pharmacological approach. This partially explains why fasted arrival strategies used by experienced long-haul travelers and aircrew produce faster functional recovery.
Why Does the Worst Jet Lag Hit on Day 3, Not Day 1?
Many travelers report feeling surprisingly functional on day 1 after an eastbound flight, followed by a crash on day 2 or day 3.
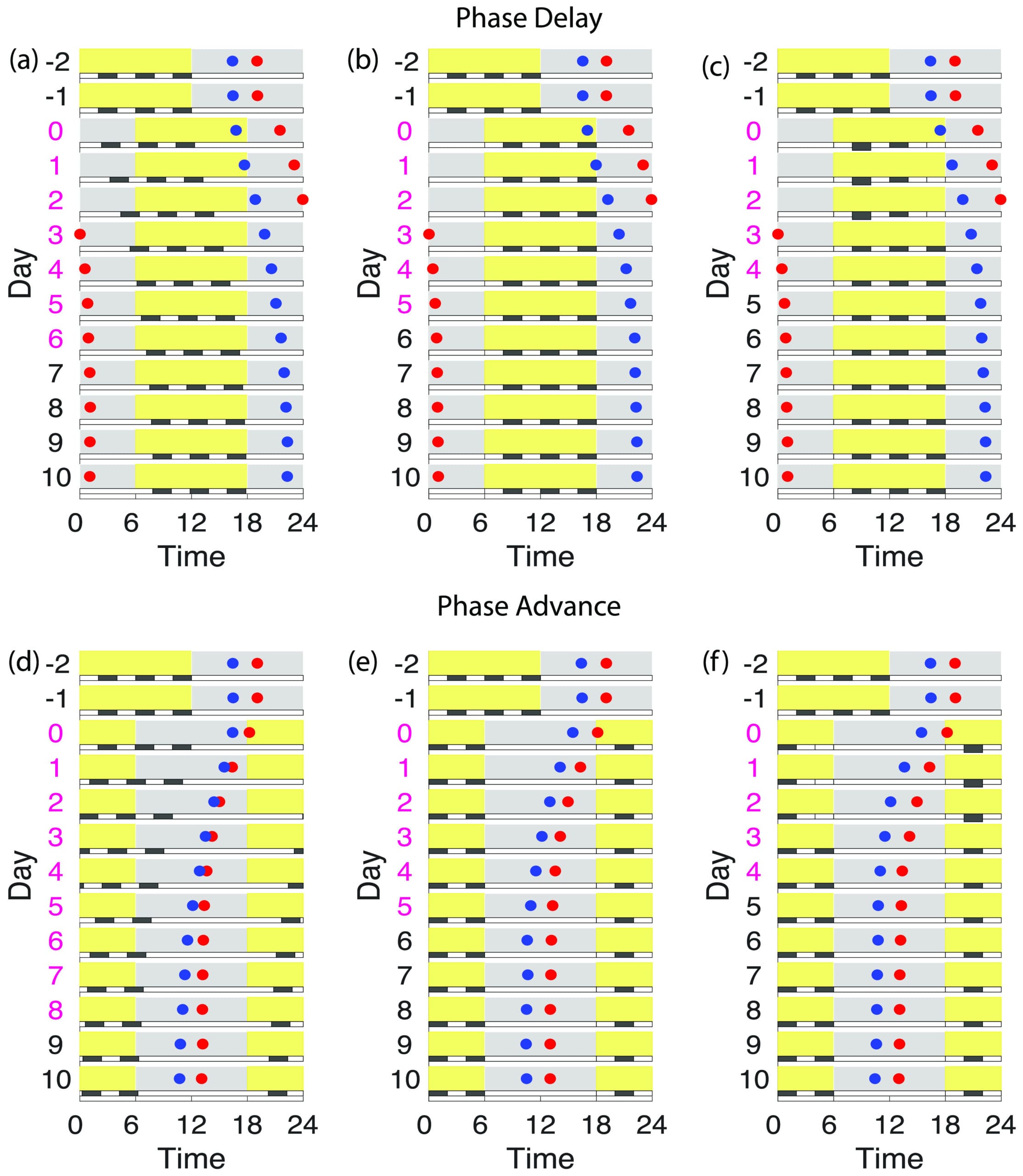
The SCN is not a uniform structure. It contains a ventrolateral core that receives direct light input and responds quickly to zeitgeber changes, and a dorsomedial shell that adapts more slowly. After a time-zone change, the core begins adjusting within hours. The shell, coupled to the core but governed by its own dynamics, follows at a slower rate.
A 2025 study by Aleixo and colleagues modeled this core-shell architecture and found that after eastward zeitgeber changes, the shell oscillators can be pushed into a slow dynamical state — a region of their phase space from which escape is disproportionately slow relative to the magnitude of the time-zone change. Because the core responds faster, the first day or two after arrival may feel relatively manageable. The mismatch between core and shell becomes maximal as the core pulls further ahead while the shell remains trapped — and that maximal internal desynchrony is what produces the day-2 or day-3 crash.
The model also generated a counterintuitive prediction about light therapy. Moderate-intensity light pulses delivered at the appropriate circadian phase reduced simulated recovery time after eastward travel. But high-intensity or long-duration light was predicted to impede rather than accelerate readjustment — because intense light can push the shell oscillators deeper into the slow dynamical region rather than guiding them out of it. The common practice of maximizing bright light exposure on arrival after eastbound flights may be counterproductive for a subset of travelers.
Direction-specific light recommendations emerge from the core-shell dynamics: morning light for eastbound travel, evening light for westbound travel. Both the direction and the dose matter. On eastbound trips, moderate, correctly timed morning light appears more effective than high-intensity uncontrolled exposure, particularly during the first 2-3 days when the slow dynamical state is active.
The same 2-3 day window is also the period where meal timing produces the largest re-entrainment benefit. Concentrating caloric intake at breakfast and omitting or minimizing dinner during the first 3 days post-arrival reduces peripheral clock re-entrainment time from 9 days to 5 days in modeled older subjects — and it works additively alongside correctly timed light.
Jet lag compounds with other circadian disruptors. If your clock was already misaligned by irregular schedules, late eating, or caffeine, transmeridian travel adds additional misalignment on top. Identifying which causes might be contributing to your sleep disruption is a useful next step.
Find out which causes might be driving your 3 AM wakeups →
Frequently Asked Questions
Can Melatonin Timing Reduce Jet Lag?
Ahmed and colleagues found that multimodal approaches — combining dietary timing, structured light exposure, and exercise — yielded superior circadian realignment outcomes compared to any single approach, with the strongest outcomes coming from travelers who combined melatonin with direction-specific light exposure and meal timing. Melatonin functions as a phase-changing cue rather than a sedative in the jet lag context: the dose is low (0.5-3mg is sufficient — higher doses do not produce greater phase change), and timing relative to the destination clock matters more than the dose. Sustained-release formulations may support sleep architecture in addition to phase adjustment.
Does Mood State Predict Jet Lag Severity More Than Circadian Phase?
Ruscitto and colleagues collected paired pre-trip and post-trip data from 28 long-haul cabin crew members using wrist actigraphy, urinary melatonin peak time as the objective circadian phase marker, and validated questionnaires assessing multidimensional jet lag, mood, and sleep quality.
Pre-trip analysis found that later baseline chronotype predicted worse post-trip jet lag — consistent with the tau-asymmetry prediction that evening chronotypes (longer tau) are more vulnerable to eastbound travel. However, the post-trip analysis revealed a dissociation: objective circadian phase measured by melatonin timing was a weak predictor of subjective jet lag, while depressed mood was a stronger predictor. Mood contributed more unique variance than circadian phase alone within the combined model.
This challenges the assumption that jet lag is a purely circadian phenomenon and implicates affective state as both a moderator and a distinct component of the jet lag experience. Mood-targeted approaches — not only circadian phase-changing strategies — may be necessary for comprehensive recovery in occupationally exposed populations such as aircrew. The n=28 sample is modest, but the within-subjects pre/post design improves statistical power relative to sample size.
Is the Phase Advance Worse for Older Travelers?
Monk and colleagues enrolled 20 healthy elderly participants (mean age 81 years) in a 15-day laboratory isolation study. Participants were assigned to either a 6-hour phase advance (eastbound equivalent, n=10) or a 6-hour phase delay (westbound equivalent, n=10) in a between-subjects design. Polysomnographic sleep and continuous rectal temperature were monitored throughout.
Phase advance produced more sleep disruption and greater circadian rhythm amplitude loss than phase delay. Sleep time decreased and REM latency increased after the advance condition. Wakefulness during the first half of the night increased following phase advance but showed no equivalent disruption after the delay — consistent with misalignment between sleep pressure and the circadian temperature nadir. Subjective alertness ratings were more impaired following phase advance, indicating that the physiological asymmetry translated into waking-hour functional consequences.
This study is notable for experimentally isolating the direction variable under controlled conditions, removing travel fatigue, hypoxia, and time-pressure confounds present in field studies. The implication for older travelers: the tau-asymmetry effect is amplified by age-related circadian vulnerability, and the meal timing countermeasure identified by Huang and colleagues becomes correspondingly more important for this population.
References
1. Lu, Z., Klein-Cardena, K., Lee, S., Antonsen, T. M., Girvan, M., & Ott, E. (2016). Resynchronization of circadian oscillators and the east-west asymmetry of jet-lag. Chaos, 26(9), 094811. https://pubmed.ncbi.nlm.nih.gov/27781473/
2. Lemmer, B., Kern, R. I., Nold, G., & Lohrer, H. (2002). Jet lag in athletes after eastward and westward time-zone transition. Chronobiology International, 19(4), 743-64. https://pubmed.ncbi.nlm.nih.gov/12182501/
3. Huang, Y., Zhang, Y., & Braun, R. (2023). A minimal model of peripheral clocks reveals differential circadian re-entrainment in aging. Chaos, 33(9), 093104. https://pubmed.ncbi.nlm.nih.gov/37669108/
4. Ahmed, O., Ibrahiam, A. T., Al-Qassab, Z. M., Kannan, V., Ullah, N., Geddada, S., & Nassar, S. T. (2024). Unraveling the impact of travel on circadian rhythm and crafting optimal management approaches: A systematic review. Cureus, 16(10), e71316. https://pubmed.ncbi.nlm.nih.gov/39534813/
5. Ruscitto, C., Ogden, J., & Ellis, J. (2023). To what extent is circadian phase predictive of subjective jet lag in long-haul cabin crew pre- and post-trip? Applied Ergonomics, 106, 103882. https://pubmed.ncbi.nlm.nih.gov/36081186/
6. Aleixo, B., Yoon, S., Mendes, J. F. F., & Goltsev, A. V. (2025). Modeling of jet lag and searching for an optimal light treatment. Journal of Biological Rhythms, 40(1), 36-61. https://pubmed.ncbi.nlm.nih.gov/39851077/
7. Monk, T. H., Buysse, D. J., Carrier, J., & Kupfer, D. J. (2000). Inducing jet-lag in older people: Directional asymmetry. Journal of Sleep Research, 9(2), 101-16. https://pubmed.ncbi.nlm.nih.gov/10849237/
Related Reading
- Circadian Rhythm Disruption: How a Misaligned Internal Clock Fragments Sleep, Drives 3AM Wakeups, and Reduces Sleep Depth — the full overview of circadian sleep disruption, including melatonin, cortisol, body temperature, peripheral clocks, and early-morning waking
- How Does a Two-Hour Weekend Sleep Delay Desynchronize Your Peripheral Clocks for Days? — how repeated weekend schedule shifts create chronic circadian misalignment
- Can Rotating Night Schedules Permanently Desynchronize Your Peripheral Clocks? — how rotating night work affects peripheral clocks and metabolic timing
- Night Owl or Delayed Sleep Phase Disorder? How to Know the Difference — how delayed circadian timing differs from preference alone
- Why Does Your Wake Time Advance by Decades — and Can You Reverse Circadian Phase Advance After 60? — why aging shifts wake time earlier and which parts remain reversible
- Which Circadian Mechanisms Change After 40 — and Which Ones Are Reversible? — the broader aging mechanisms that shift circadian timing and sleep depth
- Does Evening Exercise Delay Your Circadian Clock — or Is Disruption Smaller Than You Think? — how exercise timing affects the circadian clock and sleep onset
- Does Time-Restricted Eating Entrain Your Peripheral Clocks? — how meal timing signals peripheral clocks outside the brain
