Dr. Bronce Rice, a psychologist and psychoanalyst in our community, asked me recently:
“If my sleep has moved from 5–6 hours to ~7 hours, but I’m still waking up around 4 a.m., how do I tell if that’s good enough? I used to go to bed around 10 and get up at 5 or 6. But the older I’ve gotten the earlier I’ve been waking up. It seems no matter what time I go to bed, 3 or 4am—sometimes 4:30—is the wake time now. To help, I now go to bed on the earlier side, 8 or 9. How can I tell if its good enough?
The honest answer is: it depends.
7 hours can be good for some people. For others, 7 hours that ends at 4am still leaves them under-recovered—because the question is not only “how many hours,” but also
“are those hours landing in the part of the 24-hour cycle when your brain is set up to produce your most restorative sleep?”
Two anchors decide which side you’re on:
- how that window lines up with your circadian sleep phase, and
- how your days and health markers respond over months and years.
The rest of this note walks through both.
Why “it depends”: morning type vs evening type, and circadian alignment
A big part of “it depends” comes down to your chronotype (genotype + phenotype): how your circadian sleep phase tends to run.
- Morning-type (early) people naturally feel sleepy earlier and wake earlier.
- Evening-type (late) people naturally feel sleepy later and wake later.
- Many sit in the middle, but still lean slightly earlier or later.
Where REM sleep fits in
Across the night, sleep architecture is not evenly distributed. In most adults:
- Deep N3 sleep is concentrated in the first third of the night.
- REM sleep becomes more prominent in the second half
REM is strongly shaped by your circadian clock. When sleep is moved away from your internal night (for example, going to bed and waking in a window that doesn’t match your clock), REM in the later part of the night can be reduced.
In one controlled experiment where people slept on schedules that did not match their internal timing, reduced REM in the second half of the night was associated with changes in cortisol, insulin, and insulin resistance the next day.
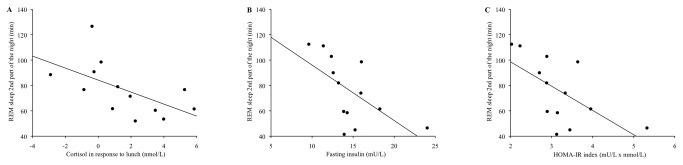
That finding illustrates a practical point for you:
- It’s not only how many minutes of REM you get.
- It’s whether your REM-heavy part of the night is happening at a circadian time that your body recognizes as late in the sleep period toward morning.
- Circadian phase varies between people (including chronotype), so the same clock-time sleep window can land at a different circadian phase across individuals.
This is one reason an “8 p.m.–3 a.m.” schedule can be different for different people:
- For a true morning type, 8–3 might still sit mostly inside their circadian sleep phase.
- For a neutral or evening type on a very early bedtime, that same schedule may not be optimal.
Sleep Pressure ≠ Circadian Alignment
At the population level, aging trends earlier in timing, and that still leaves the question of circadian alignment for an individua.
One classic way researchers separated “sleep pressure” (how long you’ve been awake) from circadian timing was by running a forced-desynchrony study.
(In a forced-desynchrony study, the lab deliberately “breaks” the normal link between clock time and the body clock. People live without time cues and follow a 28-hour schedule for sleep and wake. Their circadian clock keeps running near its natural ~24-hour rhythm, so each new sleep episode occurs at a different internal time. That lets researchers map REM and other sleep features across circadian phases while keeping sleep opportunity controlled.)
The researchers found a robust circadian rhythm in REM sleep, with the peak positioned shortly after the minimum of core body temperature (a circadian marker) and showed that REM has a strong dependence on circadian timing that’s separable from sleep pressure.
Sleep pressure can make you sleepy at many clock times; circadian phase still shapes REM and other features, so sleep can be better-timed or worse-timed even when falling asleep is easy
In other words, feeling sleepy at a given clock time doesn’t necessarily guarantee that your usual sleep window is lining up with your circadian sleep phase.
There’s also the question of REM organization, not just REM minutes.
Researchers have also shown that circadian timing influences features within REM, not only how many minutes of REM you get.
In a forced-desynchrony study, REM density (the frequency of eye movements during REM) increased across the sleep episode, and circadian modulation was most detectable late in the sleep opportunity.
This is why “I got 90 minutes of REM” on a wearable isn’t the whole story.
The same number of REM minutes can be organized differently depending on whether your sleep window matches your circadian sleep phase, and consumer devices are not built to read out finer REM features or place your sleep on a circadian-phase map the way a lab can.
This is one of 40 circadian strategies I cover in my free Circadian Mastery Protocol. If you want the full picture, download it here:
The concept of ‘circadian REM amplitude’
In a 2024 study of healthy older adults, researchers tracked REM across a 40-hour, tightly controlled lab stay with repeated naps and mapped it to each person’s circadian clock, using melatonin release timing to define their circadian sleep phase (not clock time).
Instead of just asking “how many minutes of REM did they get,” they measured how strongly REM was concentrated at each person’s circadian sleep phase versus appearing across the rest of the 24-hour day — a measure they called circadian REM amplitude.
People whose REM was more strongly pulled into their circadian sleep phase had healthier-looking white matter and deeper brain regions (including hippocampus and thalamus) on quantitative MRI.
Those with a flatter REM rhythm—less of a circadian-phase peak (lower circadian REM amplitude)—showed MRI brain microstructural differences consistent with age-associated tissue variation, even after adjusting for overall REM%.
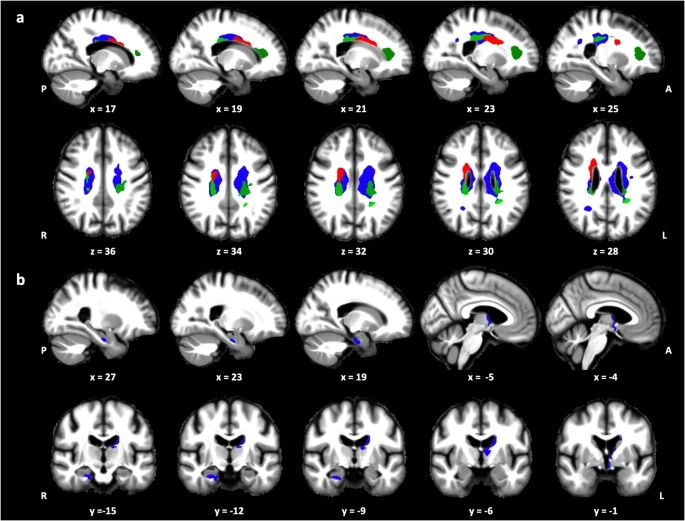
This tells us that it’s not only how much REM you get, but how tightly REM expression is coupled to your circadian sleep phase that relates to brain health.
The practical constraint: you can’t see your clock directly
In a research lab, we can define circadian timing by measuring melatonin onset in dim light or tracking core body temperature. With functional testing, we can use a multi-sample melatonin profile test to estimate this, but it requires controlled dim-light conditions and careful sampling, and many people either can’t access it or don’t want to do it.
So, outside those settings, you’re left with:
- your long-term history (what timing feels best),
- how you function across the day now, and
- how your health markers behave over time.
That’s why, when Bronce or a client asks whether their “8/9 p.m.–4 a.m., ~7 hours” pattern is good enough, I don’t start with the clock. I start with questions.
Questions I ask clients (and you can ask yourself)
For someone moving from a 10–5 / 10–6 pattern to an 8–3/4 pattern, a good first step is to compare how you function on the earlier 7-hour window vs your old timing, as carefully as you can.
Think back to a run of years and decades, not days or weeks.
A. How do your days feel?
- When you wake, do you feel refreshed — or do you feel like you are pulling yourself into the day?
- How eager are you to tackle the day’s work or responsibilities?
- Does your energy feel as steady as it did on a different schedule e.g., 0–5 / 10–6, or do you notice more variability?
- How is your mental sharpness — focus, working memory, problem-solving — compared with your better years?
- Do you hit a new energy drop that wasn’t part of your baseline before you changed your schedule (for example, a heavier crash around late morning, after lunch, or early afternoon)?
- Do you need a nap to function (not just enjoy one)?
- Do you need caffeinated drinks to get through normal days, or are they more of a preference?
If most of those answers lean positive on the newer 8–3/4 pattern, that is one indication your current window may be closer to your personal optimal. If the opposite is true — then the earlier window might not be supporting your physiology as well as the later window, even if total hours increased.
B. Compare to the last time your sleep felt satisfying
Another useful anchor:
When was the last time your sleep felt genuinely satisfying?
Was that 5 years ago? 10 years ago? 30 years ago?
Once you have a time in mind, reconstruct two things:
- What did the pattern look like?
- Bed and wake times on most nights.
- Rough total sleep duration.
- What made it satisfying?
- Maybe it was a non-event — you went to bed, woke up, and got on with your day.
- Energy across the day felt steady.
- Mood was flexible rather than thin.
- You didn’t think about sleep much.
The more your current pattern resembles that “last satisfying pattern”— adjusted for the realities of your current life — the closer you likely are to your personal ideal, regardless of your age.
💡 Something I want to underline: in the generally healthy individual, there is no fundamental reason that worse sleep is a requirement with age. What changes with age is susceptibility—your sleep becomes more sensitive to disruptors. That’s different from sleep decline is inevitable.
There is no single correct answer here. These questions ground your decision in your physiology rather than in what’s common or what’s worked for someone else.
Broader implications — when to look beyond “how I feel”
In a Stanford study of over 4,000 cognitively healthy adults aged 65–85, those who slept 6 hours or less had higher body mass index and more amyloid-β (one of the proteins that accumulates in Alzheimer’s disease) in the brain than those sleeping about 7–8 hours, even after accounting for age, education, race/ethnicity, and APOE genotype.
Taken together with other work, it suggests that 7–8 hours is still a better anchor range for brain and metabolic health in later life than 5–6 h.
So, if you have lived with a short or very early pattern for years, I would also pay attention to:
- Blood pressure trends over several years.
- Fasting glucose and HbA1c or other markers of blood sugar handling.
- Body composition changes (especially extra weight around the midsection) that appeared without a meaningful change in nutrition or movement.
- Recovery capacity dropping given the same training load
If these patterns move in the a direction you don’t want while you are running on an early 5–6-hour window, that is a clue that the sleep pattern may be under-supporting.
Bringing it back to you—If you are asking Bronce’s question for yourself, here is a concise way to approach it:
- Total hours: Aim for a pattern that gives you 7–8 hours whenever your life allows it. That is the range where long-term data lsooks more favorable for mood, metabolism, and brain health.
- Timing: Look at your history. If your best-feeling years were anchored earlier, a stable 8:30–4:00 pattern with 7+ hours may be acceptable. If your best years ran later, try nudging your schedule later in small steps.
- How your days feel: Use the questions above over a few weeks.
- Health markers: If your blood pressure, glucose handling, or body composition have worsened while your lifestyle hasn’t changed, consider that as feedback regarding your sleep.
For someone like Bronce, who has always been an early sleeper and feels and functions better on a 7-hour early window than on a shorter one, an 8/9 p.m.–4 a.m. pattern can be a reasonable destination.
For someone whose best years were centered later sleep window, or who moved to an early 5–6-hour window only in midlife and never truly adapted, that same pattern is a prompt to keep going: add hours if possible, and adjust timing in small steps so that your sleep lines up better with your own biological circadian night.
—Kat
P.S. If you found this useful, you’ll get a lot out of my free Circadian Mastery Protocol — the 40-part baseline I walk through with every client before we do deeper recovery work. It maps every timing cue from morning to midnight so you can see exactly where your foundation has gaps. Download it here.
References
- Baron KG, Reid KJ. Circadian misalignment and health. Int Rev Psychiatry. 2014 Apr;26(2):139-54. doi: 10.3109/09540261.2014.911149. PMID: 24892891; PMCID: PMC4677771.
- Gonnissen HK, Mazuy C, Rutters F, Martens EA, Adam TC, Westerterp-Plantenga MS. Sleep architecture when sleeping at an unusual circadian time and associations with insulin sensitivity. PLoS One. 2013 Aug 8;8(8):e72877.
- Deantoni, M., Reyt, M., Dourte, M. et al. Circadian rapid eye movement sleep expression is associated with brain microstructural integrity in older adults. Commun Biol 7, 758 (2024).
- Khalsa SB, Conroy DA, Duffy JF, Czeisler CA, Dijk DJ. Sleep- and circadian-dependent modulation of REM density. J Sleep Res. 2002 Mar;11(1):53-9.
- Kim JH, Elkhadem AR, Duffy JF. Circadian Rhythm Sleep-Wake Disorders in Older Adults. Sleep Med Clin. 2022 Jun;17(2):241-252.
- Duffy JF, Zitting KM, Chinoy ED. Aging and Circadian Rhythms. Sleep Medicine Clinics. 2015 Dec;10(4):423-434.
- Winer JR, Deters KD, Kennedy G, Jin M, Goldstein-Piekarski A, Poston KL, Mormino EC. Association of Short and Long Sleep Duration With Amyloid-β Burden and Cognition in Aging. JAMA Neurol. 2021 Oct 1;78(10):1187-1196.