Why Are You the Only One Who Can Lead Your Preventive Health?
Nearly 1/3 of all new U.S. jobs in the past year came from health care. In 38 states, it’s now the largest single employer. But chronic disease rates are rising, provider burnout has reached record highs, and patient satisfaction is lower than ever—because the expansion is concentrated in late-stage approach, not prevention.
- Every new diabetes center represents people who didn’t need to develop diabetes; every cardiac unit expansion reflects preventable heart disease. Adding disease management infrastructure doesn’t create health—it manages its absence.
- You are the only one who lives in your body 24/7. No 15-minute appointment can replicate your daily awareness of changing energy, sleep patterns, and digestion.
- Personalized preventive care means proactive screening when you feel well, biomarker tracking to catch changes before they become disease, and arriving at appointments with your own observed patterns and questions.
- When more people engage proactively with their own health, the healthcare infrastructure can focus on complex problems rather than managing conditions that could have been caught earlier.
- No drug or AI tool drives longevity the way consistent, informed self-observation does—combined with medical expertise at the right time.
Preventive Health: You’re the only one who lives in your body 24/7. Here’s why that matters more than any doctor visit.
More Americans now work in health care than any other sector—so why are outcomes still getting worse?
In the last year alone, nearly 1/3 of all new jobs in the U.S. came from one sector: health care.
More than manufacturing. More than tech. In 38 states, health care is now the largest single employer.
On paper, this looks like progress—more jobs, more access, more resources devoted to keeping us well.
But that assumption deserves a closer look:
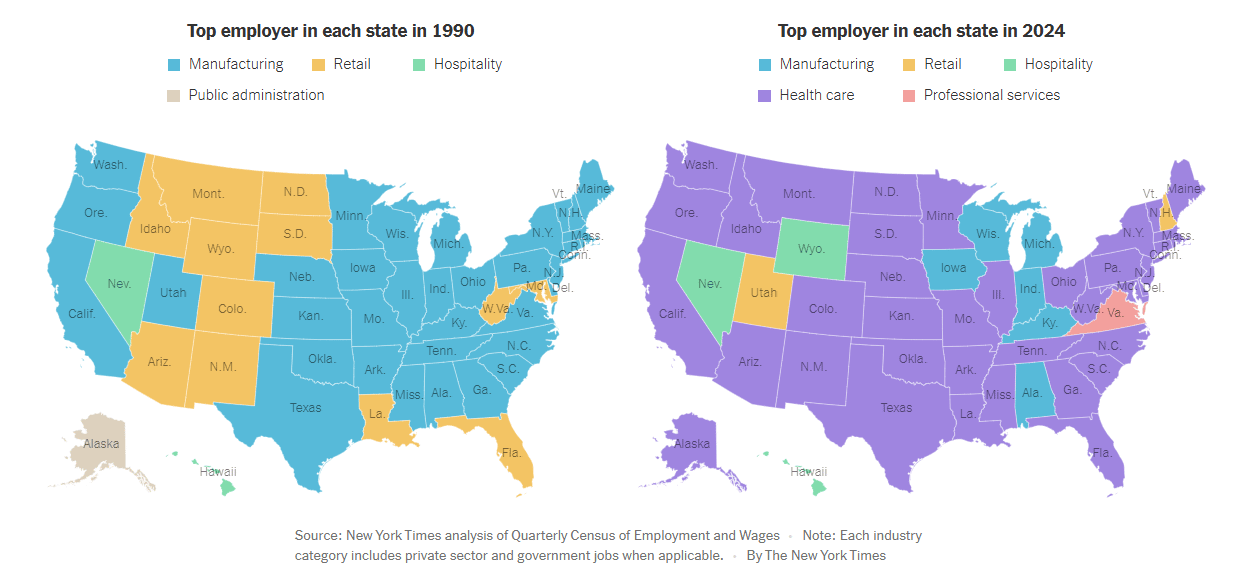
Because most of this expansion isn’t happening in prevention.
It’s happening in treatment. In late-stage, symptom-driven care. In patching up the downstream effects of poor health—not preventing them in the first place.
This is what happens when a system grows without evolving. We expand the infrastructure of disease management, not health creation.
And it’s costing us more than money.
Why Doesn’t More Health Care Lead to Better Health?
Every new diabetes center represents thousands of people who didn’t need to develop diabetes. Every cardiac unit expansion signals preventable heart disease. Every oncology wing reflects missed opportunities for cancer prevention.
Chronic disease rates are rising. Burnout among providers is at record highs.
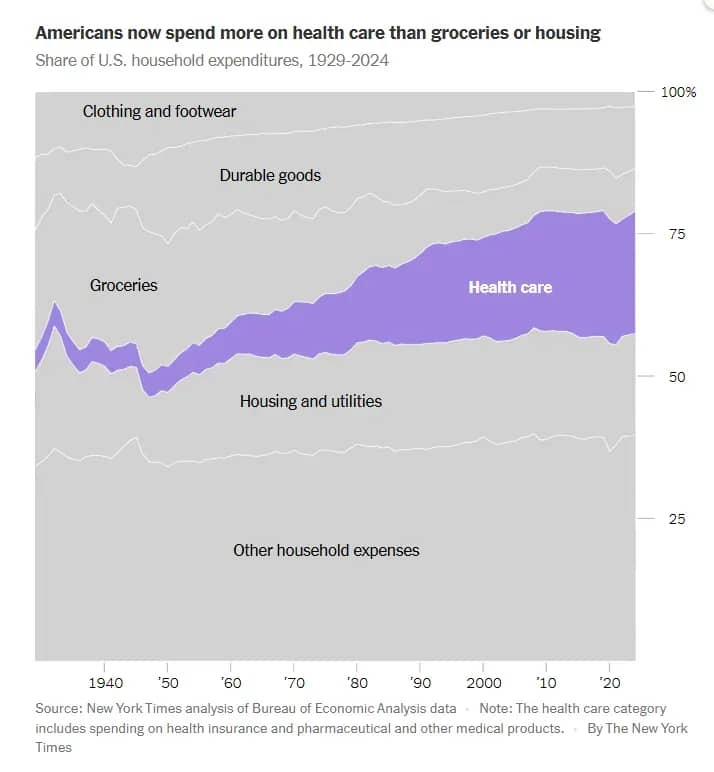
And what about patient satisfaction? Lower than ever.
Real healthcare progress would look different:
- Fewer people needing intensive interventions
- More resources directed toward prevention and health creation
- Technology advancing longevity, not just treating decline
But that’s not the system we’re building.
We train more nurses, hire more support staff, and build more facilities—but most of that growth still revolves around diagnosing and treating illness after it shows up.
We’re doubling down on reactive medicine while prevention gets virtually no economic support.
And while some of that is certainly necessary, it’s not where real progress lies.
Why Is Your Own Observation the Underutilized Asset in Preventive Health?
Here’s the part that rarely gets said: you are the only one who lives in your body 24/7.
Not your doctor. Not your insurer. Not your lab report.
You notice when energy shifts. When sleep patterns change. When your digestion doesn’t feel quite right.
And no 15-minute appointment can replace that level of daily awareness.
The most powerful health intervention isn’t a new drug or procedure. It’s recognizing that you’re the primary observer of your own biology.
Upgrade for personalized roadmaps—systematic implementation frameworks you can personalize to your specific biomarkers and risk factors.
This means:
- Proactive screening when you feel optimal, not when symptoms force your hand
- Biomarker tracking to catch changes ahead of disease
- Making decisions with both data and intuition
- Seeking expert interpretation when needed—but showing up informed
Too often, the healthcare system treats your body like a black box that only experts can interpret. But you’re not a passive recipient of your own biology.
You’re the chief of a system you inhabit every moment. You have access to real-time data no laboratory or device can replicate: how you feel, what’s changing, and what inputs you are feeding into your body.
That’s where smart partnerships begin.
Do you want to empower someone you care about?
Share The Longevity Vault with them so they can join the free Longevity Essentials Masterclass series—where I break down how to test, track, and take action before symptoms show up.
When you come to the table:
- With your own baseline metrics
- With patterns you’ve observed
- With specific questions and an idea about direction
- With a prevention mindset, not just a treatment need
This isn’t about rejecting medical expertise—it’s about bringing irreplaceable intelligence to the collaboration.
Because your job isn’t just to comply and wait for instructions. It’s to notice, to track, to intervene early. To take ownership of your baseline—and your trajectory.
That’s not anti-medical.
That’s what true partnership looks like.
Why Does the Transition From Health Care to Health Creation Matter?
The more of us who approach health this way, the better the outcomes. Not just for individuals—but for society.
Because every time someone catches a deficiency before it becomes disease, every time someone course-corrects based on early warning signs, we free up the system to do what it was meant to do: provide specialized, high-quality care for complex problems.
Innovate.
Advance.
But if we keep using the system to manage lifestyle-driven breakdowns that could have been prevented, it will never catch up.
No matter how many jobs it creates.
And no matter how many dollars we throw at it.
What Is the Longevity Vault’s Approach to Health Creation?
If prevention & self-regulation don’t become the default, we risk codifying decline—turning dysfunction into policy, and passivity into public health strategy.
That’s why I’m focused on building usable, individualized systems for health sovereignty—tools that make prevention, staying well the baseline, not the outlier.
Not just because prevention should be the economic model. But because the most powerful force in your longevity isn’t a new drug, or AI diagnostic tool, or even a great specialist.
It’s you—showing up consistently, with the right inputs, at the right time.
Let’s build around that.
If this shifted how you think about your health—pass it on.
Forward this email to someone you care about—or share The Longevity Vault with them—where I share the practical & personalized tools for health creation.
See you next time,
—Kat
Upgrade for personalized roadmaps—systematic implementation frameworks you can personalize to your specific biomarkers and risk factors.
Frequently Asked Questions
Does more health care spending lead to better health outcomes?
Not necessarily. In the last year, nearly 1/3 of all new U.S. jobs came from health care—in 38 states, it’s now the largest single employer. Yet chronic disease rates are rising, provider burnout is at record highs, and patient satisfaction is lower than ever. The expansion is concentrated in approach, not prevention.
Why do we have more health care workers but worse health outcomes?
The growth is happening in late-stage, reactive care—managing illness after it appears, not preventing it. Every new diabetes center represents people who didn’t need to develop diabetes; every cardiac unit expansion reflects preventable heart disease. Expanding disease management infrastructure without investing in prevention doesn’t improve health creation.
What does personalized preventive care involve?
It means tracking biomarkers to catch changes ahead of disease, doing proactive screening when you feel well—not waiting for something to go wrong—and bringing your observed patterns and specific questions to medical appointments. You are the only one who lives in your body 24/7, with access to information no laboratory or device can replicate.
How can I take a proactive approach to health without rejecting medical expertise?
This approach isn’t anti-medical—it means bringing irreplaceable intelligence to the collaboration. You show up with your baseline metrics, observed patterns, and specific questions, with a prevention focus rather than a approach need. Your job is to notice, track, and intervene early; medical expertise interprets and advances from there.
References
- DePillis, L., & Zhang, C. (2025, July 3). How health care remade the U.S. economy. The New York Times.