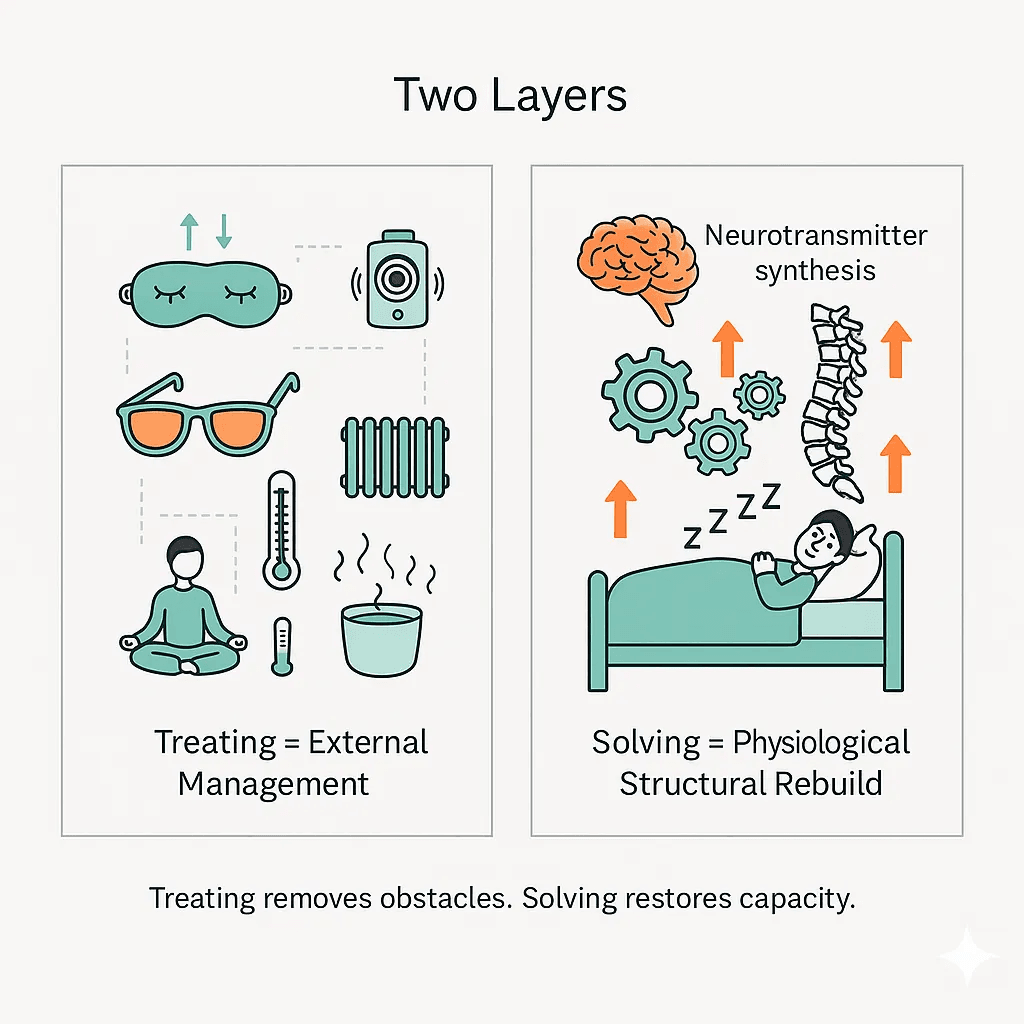
The distinction between treating and solving sleep problems explains why considerable effort can produce minimal lasting change. Treating removes obstacles—environmental adjustments like cooling your room, blue light blockers, and white sound machines that prevent disruption or make poor sleep more manageable. Solving targets what generates sleep capacity in the first place: the underlying architecture that makes consistent, restorative sleep possible without external scaffolding.
- Environmental controls (room temperature 65–68°F, blue light blockers, blackout curtains, white sound) prevent disruption—they don’t build the physiological capacity needed to initiate or sustain sleep
- Blue light reduction prevents melatonin suppression after sunset, but if the body lacks the materials to synthesize melatonin, removing the light source doesn’t restore the internal pathway
- Treating approaches serve a function—they prevent worsening and make the condition manageable—but don’t rebuild what enables sleep to happen on its own
- Results that feel “sometimes, somewhat, a little” are consistent with an approach designed to remove disruption rather than restore sleep-generating capacity
- This framework for distinguishing treating from solving applies to any sleep recommendation—and forms the basis of Part 3 in the Vault Sleep Clarity Series
What Is the Difference Between Managing Sleep and Resolving Sleep?
Last time, we explored poor sleep as a symptom—a signal pointing to underlying issues rather than the source problem itself. We used back pain as our comparison: the pain itself tells us something needs attention, but managing the pain doesn’t rebuild the structural support your spine requires (If you’re jumping in mid-series or need a refresh, start with Part 1 here).
Today, we’re making a distinction that explains why considerable effort may have produced minimal lasting change: the difference between “treating” vs. “solving”.
Let’s first return to the back pain comparison to see why this matters.
What Does Managing Back Pain Teach Us About Managing Sleep?
Treating back pain manages the symptom:
- Wearing a back brace for external support
- Avoiding prolonged sitting to prevent aggravation
- Using anti-inflammatory medications to reduce pain signals
- Applying heat or ice to affected areas
These strategies serve an important function.
They prevent worsening.
They make the condition manageable.
But here’s what they don’t do: they don’t create the structural integrity needed for healthy movement. Avoiding sitting doesn’t strengthen your core. A back brace doesn’t rebuild the muscular support your spine requires for proper load distribution.
What Does Resolving Back Pain Teach Us About Resolving Sleep?
Solving back pain targets the source:
- Strengthening core musculature to provide spinal support
- Correcting movement patterns that created the initial dysfunction
- Restoring proper joint mechanics and load distribution
- Addressing muscular imbalances that compromise stability
These approaches rebuild the system’s capacity to function without external support. They don’t just manage symptoms or prevent worsening—they restore the underlying architecture that prevents the problem from happening again.
Why Do Comprehensive Sleep Protocols Still Leave You Awake at 3 A.M.?
Think about the most common strategies: blue light blockers, cooling mattresses, new pillows, meditation tracks, white noise machines…
Now, ask yourself: When you use these, does it feel like you are correcting the original source of the problem, or does it feel like you are managing the day-to-day symptom of being unable to sleep?
If results have felt temporary—”sometimes, somewhat, a little”—there’s a concrete reason for that pattern.
Most sleep recommendations fall into the “treating” category:
- Room temperature optimization (65-68°F)
- Cooling mattress technology
- Blackout curtains and eye masks
- White noise machines
- Calming pre-bed routines
These environmental controls are useful. They remove obstacles and can prevent disruption. But they don’t build or create the physiological capacity for initiating or sustaining sleep.
Consider blue light exposure. Reducing blue light after sunset prevents melatonin suppression. This is valuable. But if your body lacks the materials to synthesize melatonin in the first place, removing blue light won’t restore the signaling pathway.
You can’t solve an internal signaling problem with external environmental adjustments, just as you can’t solve structural spinal instability by avoiding sitting.
What Changes When You Distinguish Between Managing and Resolving Sleep?
Here’s what changes with this understanding:
Many approaches we’ve implemented—with considerable effort and consistency—were designed to remove disruption (like blue blockers) or prevent worsening (like calming prebed routines).
They are not designed to restore the body’s core sleep-generating system.
The reason our results have been “somewhat better” or “sometimes helpful” rather than consistently restorative is this: we’ve been treating when we needed to solve.
What Comes Next After Understanding the Difference?
Next time, I’ll show you a simple framework that distinguishes treating approaches from solving approaches—a lens you can use to categorize any sleep recommendation you encounter.
This framework is also what helped me make sense of my own 15 years sleep struggle (why I had a 50-step prebed ritual, yet still found myself staring at the ceiling at 3 AM several nights a week.)
It’s a clarifying lens worth having.
See you next time.
Upgrade for personalized roadmaps—systematic implementation frameworks you can personalize to your specific biomarkers and risk factors.
Frequently Asked Questions
Why do sleep hygiene routines produce results that feel inconsistent or temporary?
Sleep hygiene approaches—room temperature, blackout curtains, calming pre-bed routines—are designed to remove obstacles and prevent disruption. They don’t build or restore the physiological capacity your body needs to initiate and sustain sleep. When results feel like “sometimes, somewhat, a little,” the approach is treating the indicator rather than addressing what creates it.
Do blue light blockers fix sleep problems?
Blue light blockers serve a specific purpose: preventing melatonin suppression after sunset. But if your body lacks the materials needed to synthesize melatonin in the first place, removing blue light won’t restore that internal pathway. An external environmental adjustment can’t resolve an internal production problem.
What is the difference between treating and solving sleep problems?
Treating sleep problems manages the indicator—environmental controls and behavioral adjustments that prevent disruption or make the condition more manageable. Solving targets the underlying architecture that generates sleep capacity. The distinction matters because treating can make sleep feel somewhat better without producing durable, consistent restoration.
Why did a 50-step pre-bed routine still leave someone unable to sleep?
A 50-step pre-bed routine is an elaborate treating approach—each step manages a potential disruption or obstacle. Without addressing what builds the body’s core sleep-generating capacity, even comprehensive pre-sleep preparation leaves the underlying problem intact. That’s why effort and consistency alone don’t produce lasting results.
