➤ Someone recently asked me this question, and it captures a pattern I see constantly:
“I have no trouble falling asleep. I’m out within minutes. But I wake up at 3 a.m.—sometimes to pee, sometimes for no reason—and I can’t get back to sleep. I drift in and out until 5 a.m. and nothing I’ve tried fixes it.”
They’d tried melatonin. Magnesium. No screens. No caffeine.
Nothing worked.
Here’s what I told them: falling asleep and staying asleep are different problems.
What Does the Opposite Sleep Pattern — Difficulty Falling Asleep but Sleeping Through — Tell You?
If someone has difficulty falling asleep but then sleeps deeply and continuously for seven to eight hours, a circadian or timing-related adjustment can often resolve the issue entirely. The fix tends to be relatively contained.
Staying asleep is more complex.
Why Is Staying Asleep Harder to Solve Than Falling Asleep?
In the individuals I work with, difficulty staying asleep is usually related to being in a lighter-than-ideal sleep state during a specific window—and therefore more vulnerable to disruption from various things: bathroom trips, thoughts, a noise outside, pain, or dreams that wake the individual and keep them awake.
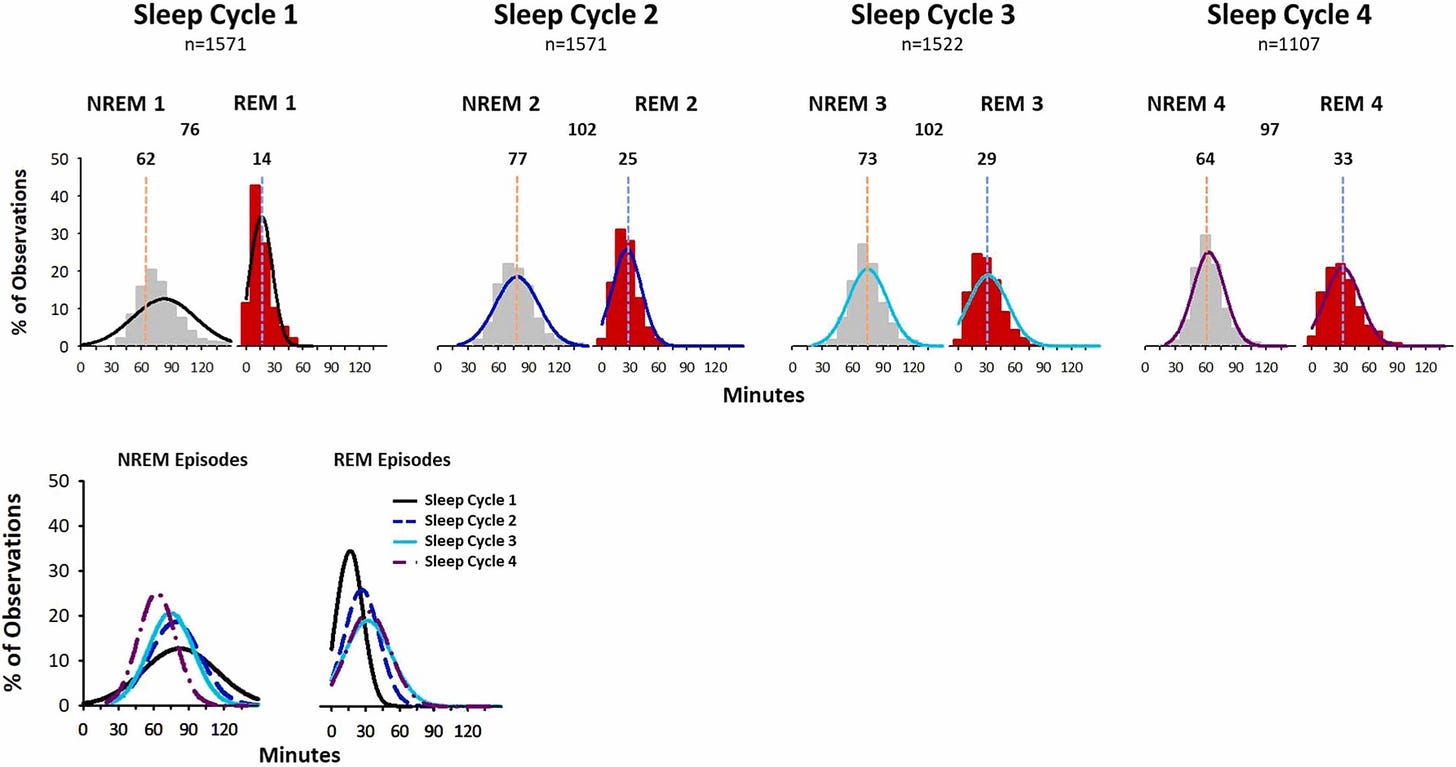
During sleep, your brain cycles through 80- to 120-minute ultradian cycles. At the end of each cycle—and during transitions between sleep stages—the brain has brief arousals on the order of seconds to minutes. Many of these aren’t remembered.
It is during these moments that you become vulnerable to triggers that can turn a brief, normal arousal into sustained wakefulness and alertness.
Why Are You Easily Woken and Then Unable to Return to Sleep?
It’s not the drinking too much water. It’s typically not the life responsibilities causing the thinking. It’s not the dreaming.
- If you pop awake briefly and fall back asleep fast, that often fits typical sleep architecture.
- If your awakenings are long, frequent, and leave you feeling wired and alert, then something is amplifying what should be a normal sleep transition into sustained wakefulness.
Why Does This Distinction Change What You Should Focus On?
If your solutions target the triggers—drink less water, block noise, meditate before bed—instead of the internal state that’s amplifying them, you’ll keep cycling through partial fixes. The trigger changes. The wakeup stays.
This distinction is the foundation of how I approach sleep work. Falling asleep and staying asleep need different investigations, different timelines, and different tools.
Warmly,
—Kat
P.S. If your sleep has changed since midlife and you want a structured, mechanism-based approach to addressing your sleep, here’s how I help.
